Topic
Clinical Immunology
Inflammation, autoimmunity, NK cells, gut-immune axis, and evidence-based immune modulation. Understanding your immune system beyond simple 'boosting.'
Explore by Topic
Autoimmunity
Molecular mimicry, tolerance breakdown, and integrative approaches to autoimmune conditions.
Gut-Immune Axis
The microbiome-immune connection and mucosal immunity.
NK Cells
Natural killer cell function, testing, and therapeutic enhancement.
Inflammation
Chronic low-grade inflammation, cytokine storms, and resolution pathways.
Immune Modulation
Restoring immune balance through targeted intervention rather than suppression.
Free Guide
Understanding Your Immune System
Download the complete physician's guide. Evidence-based, no hype.
All Articles
40 articles
Chronic Fatigue Syndrome: A Physician's Complete Guide
A physician's complete guide to chronic fatigue syndrome. Mitochondrial dysfunction, immune dysregulation, diagnostic criteria, and the stepwise treatment approach we use at Klinik St. Georg.

CD57 Test in Lyme Disease: Useful or Unreliable?
The CD57 test in Lyme disease — what it measures, Dr. Stricker's original hypothesis, conflicting study results, and how clinicians actually use it in practice.

How to Read Your Microbiome Test Results
Practical guide to interpreting gut microbiome test results. Dysbiosis markers, keystone species, diversity metrics, and what your results actually mean for treatment.

GI-MAP vs Standard Stool Culture: Which Test to Choose
Comparing GI-MAP qPCR stool testing with standard stool culture. Detection rates, pathogen coverage, clinical utility, and when each test is the right choice.

Lyme Disease, Gut Dysbiosis, and Leaky Gut
How Lyme disease disrupts the gut microbiome. Antibiotic-driven dysbiosis, Borrelia's effect on intestinal permeability, the Hopkins microbiome findings, and recovery strategies.

Lymphocyte Subset Panel: Reading Your Immune Profile
How to read a lymphocyte subset panel. What CD4, CD8, CD19, and CD56 cells do, what abnormal ratios mean in chronic illness, and when this test changes your treatment.

Low NK Cell Function: What It Means and What to Do
Understanding low natural killer cell function in chronic illness. What NK cells do, why function drops, how to test, and evidence-based strategies to restore immune surveillance.
Hyperthermia for Cancer: Evidence, Protocols, and Clinical Experience
Hyperthermia cancer treatment evidence from RCTs and 35 years of clinical use. How moderate and extreme WBH synergize with chemo and radiation therapy.
Histamine Intolerance: Beyond Allergies
Why histamine intolerance is a systemic condition, not just allergies. Mechanisms, diagnostic pitfalls, gut-immune connections, and treatment strategies from clinical experience.
Mast Cell Activation Syndrome (MCAS): A Clinical Guide
A physician's guide to MCAS — mechanism, symptoms, diagnostic criteria, treatment, and the connection to Lyme, mold, and EBV. Based on clinical experience treating patients with complex multi-system illness.
Mistletoe Therapy (Iscador): Evidence in Integrative Oncology
Mistletoe extract (Iscador, Helixor) for cancer: mechanism, NK cell activation, quality of life evidence, injection protocols, and the German clinical tradition.
How Reactivated Viruses Suppress Your Immune System
The immune suppression cascade: how Lyme disease triggers EBV, HHV-6, and CMV reactivation, and how these viruses further suppress immunity in a vicious cycle.
Brain Fog and Neuroinflammation: The PET Scan Evidence
What causes brain fog in Lyme disease — Johns Hopkins PET scan findings showing glial activation, neuroinflammation mechanisms, and treatment implications.

PEMF for Lyme Disease and Chronic Pain
How pulsed electromagnetic field therapy supports pain relief and inflammation reduction in Lyme disease — mechanism, clinical evidence, and practical considerations.
The Vagus Nerve and Inflammation: Cholinergic Anti-Inflammatory Pathway
How the vagus nerve controls inflammation through the cholinergic anti-inflammatory pathway. Mechanism, clinical significance, and implications for chronic illness.
Integrative Oncology: What It Is and What It Is Not
A clinician's guide to integrative oncology. What complementary therapies have evidence, how they work alongside conventional treatment, and what 35 years of clinical experience at Klinik St. Georg have shown.
KPV for Gut Inflammation: IBD, Colitis, and Clinical Evidence
How the KPV tripeptide reduces gut inflammation. NF-kB inhibition, PepT1 uptake, IBD and colitis evidence, oral dosing, and clinical observations.
LL-37 and Vitamin D: The Immune Connection
How vitamin D regulates LL-37 production and why this matters for immunity. The cathelicidin pathway, optimal levels, and clinical implications.
Thymosin Alpha-1 for Cancer: Immunotherapy Support
How Thymosin Alpha-1 supports cancer immunotherapy. T-cell activation, dendritic cell maturation, clinical trial data, and practical protocols.
Thymosin Alpha-1 Dosage and Protocol
Evidence-based Thymosin Alpha-1 dosing. Subcutaneous protocols for immune support, cancer adjunct, infection, and chronic disease applications.

Curcumin: Why Most Supplements Don't Work and Which Ones Do
The bioavailability problem with curcumin explained. Comparing Meriva, Longvida, BCM-95, Theracurmin, liposomal, and piperine forms. Dosing by condition.

NAC Dosage Guide: How Much to Take for Liver, Lungs, and Immune Support
Evidence-based NAC dosing by condition. Liver support, respiratory health, immune function, mental health, and general antioxidant use. Physician-guided protocols.
Omega-3 Dosage for Inflammation: EPA and DHA for Joints, Brain, and Heart
Evidence-based omega-3 dosing for inflammation. How much EPA and DHA for joint pain, cardiovascular inflammation, neuroinflammation, and autoimmune conditions. Physician protocols.

Probiotics: Matching the Right Strain to the Right Condition
Evidence-based guide to probiotic strain selection. Which strains work for which conditions, when to avoid probiotics, CFU counts, spore-based vs traditional, and what I use in clinical practice.

Probiotics vs. Prebiotics vs. Postbiotics: What the Difference Means for Your Gut
Physician guide to probiotics, prebiotics, postbiotics, and synbiotics. Definitions, mechanisms, when to use each, and how they work together for gut health.

Immune Profiling: Lymphocyte Subsets and Cytokines
What immune profiling reveals about your health that standard blood work cannot. Lymphocyte subsets, NK cells, and cytokine panels explained.

Microbiome Testing: Stool Analysis Interpreted
What microbiome stool tests measure, how to interpret results, and which tests provide actionable clinical information. By Dr. Julian Douwes.
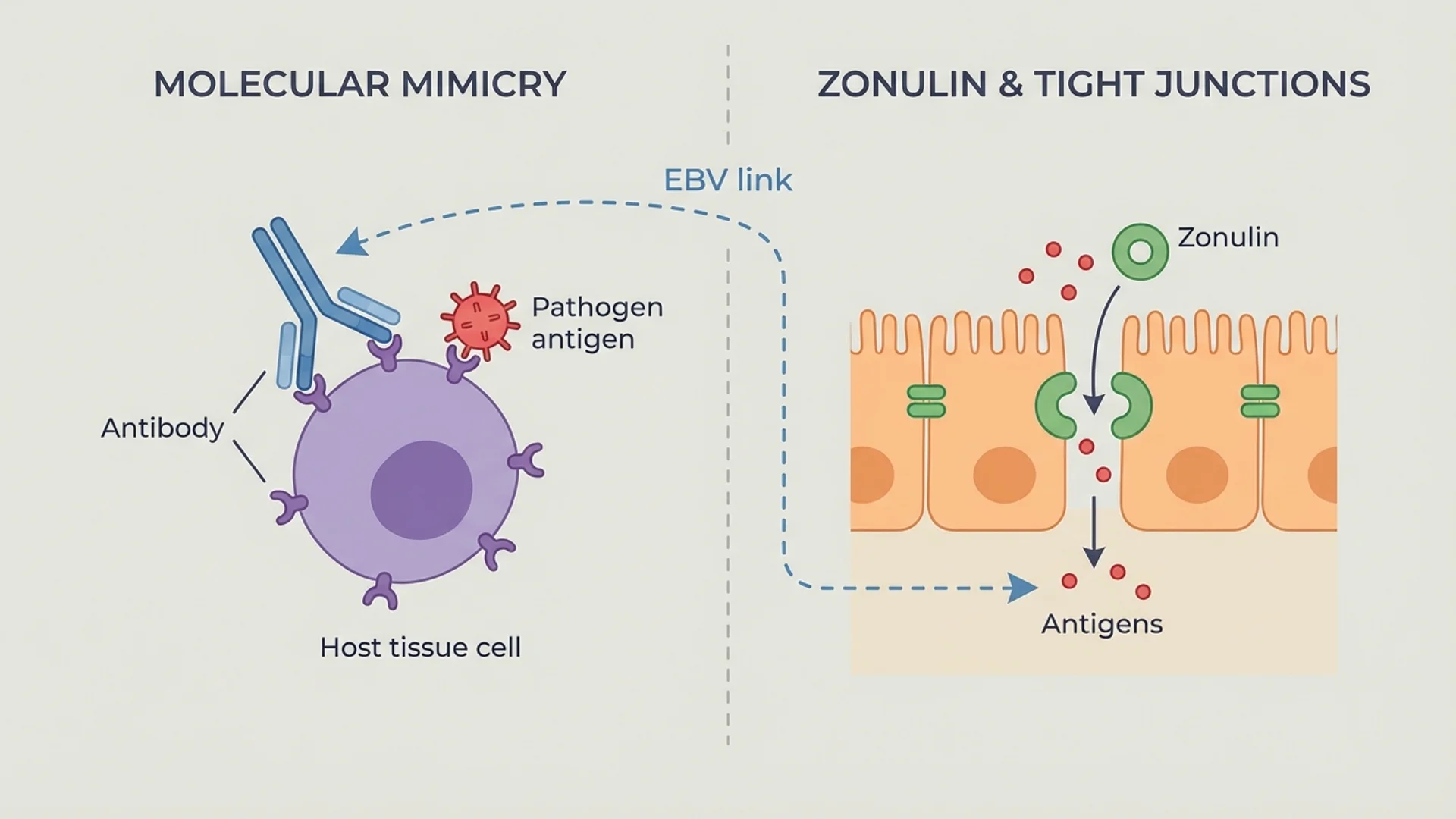
Autoimmune Disease: Mechanisms and Treatment
Why the immune system attacks itself, what triggers autoimmunity, and how integrative medicine approaches treatment. By Dr. Julian Douwes.

Cytokine Storms: When Immunity Goes Wrong
What causes a cytokine storm, how it damages the body, and what physicians can do about it. A clinical explanation by Dr. Julian Douwes.
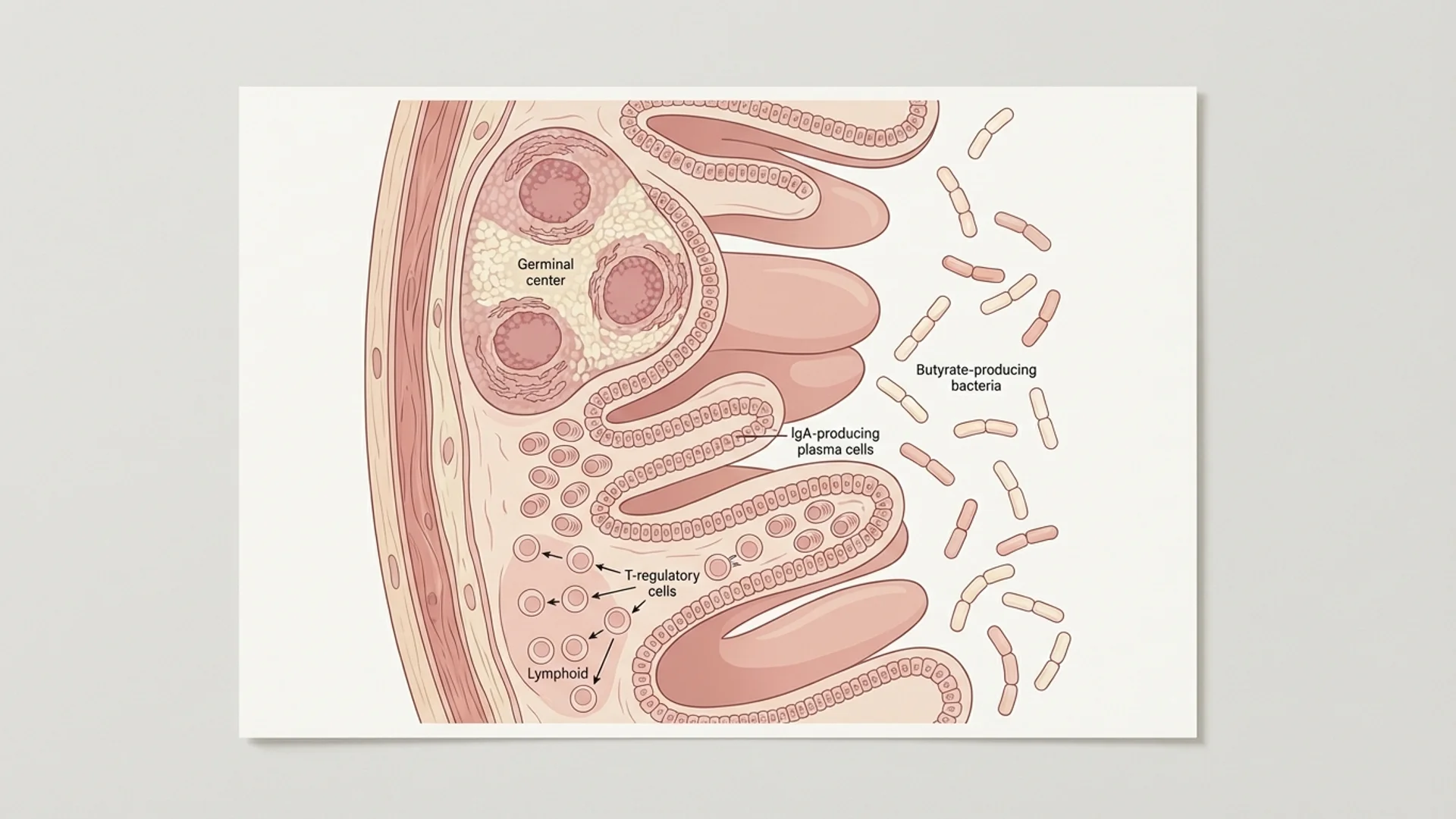
The Gut-Immune Axis: Where Immunity Begins
Why 70% of your immune tissue lives in the gut, and what this means for health, autoimmunity, and treatment. By Dr. Julian Douwes.
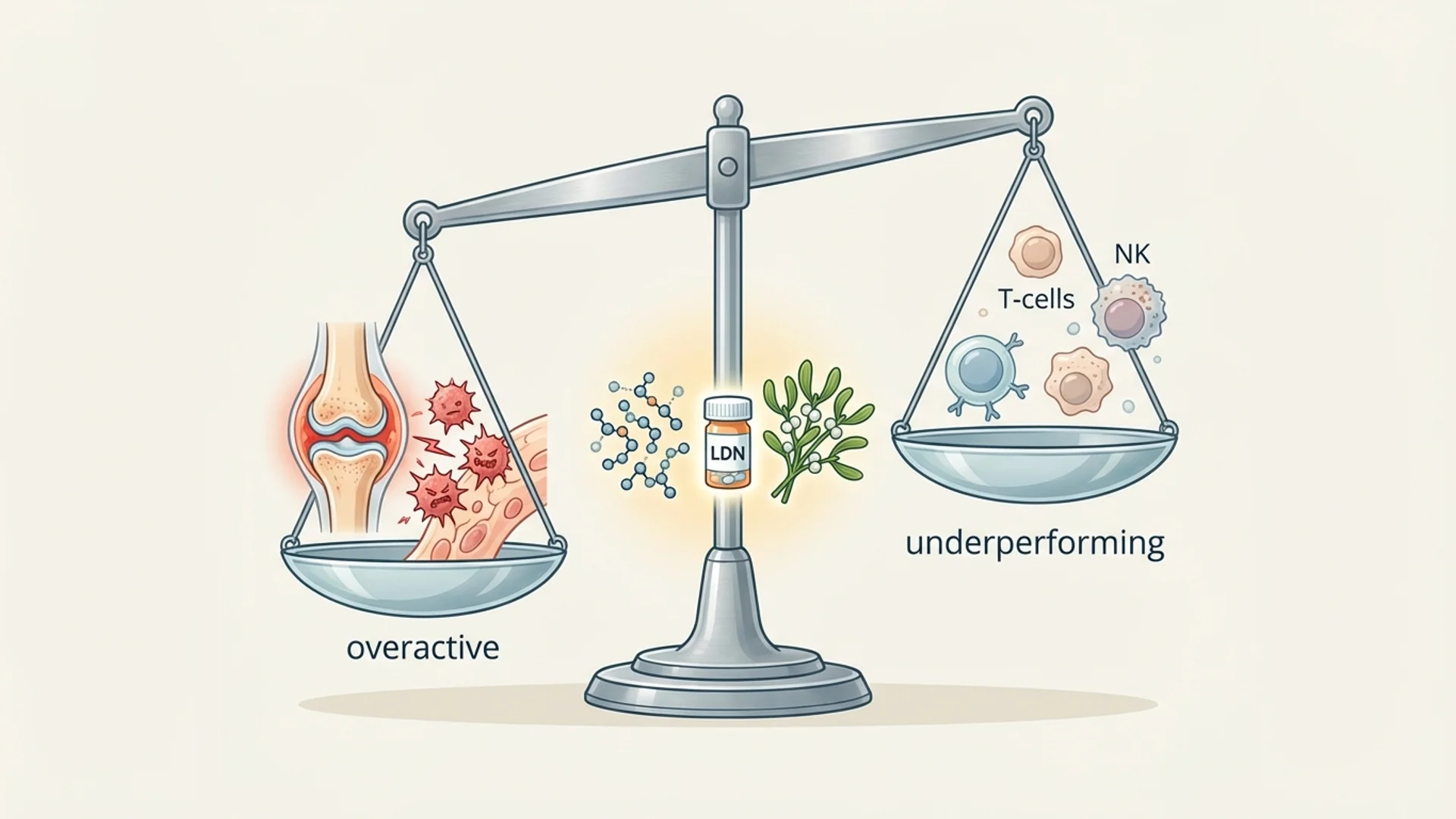
Immune Modulation: Enhancing or Calming Immunity
How physicians enhance weak immune responses and calm overactive ones. Evidence-based immune modulation explained by Dr. Julian Douwes.
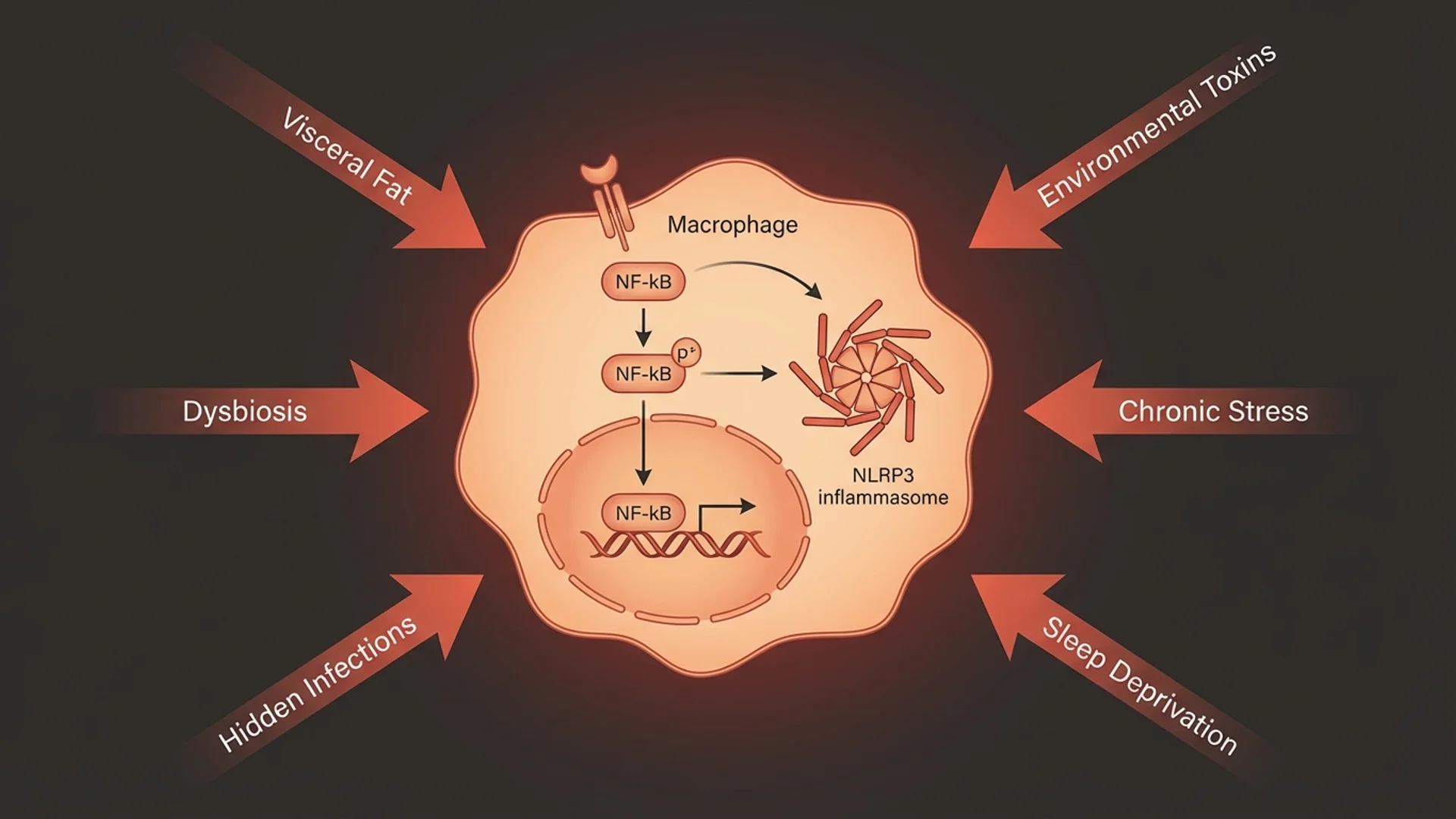
Chronic Inflammation: The Root of Disease
How chronic low-grade inflammation drives disease, what causes it, and evidence-based strategies to address it. By Dr. Julian Douwes.
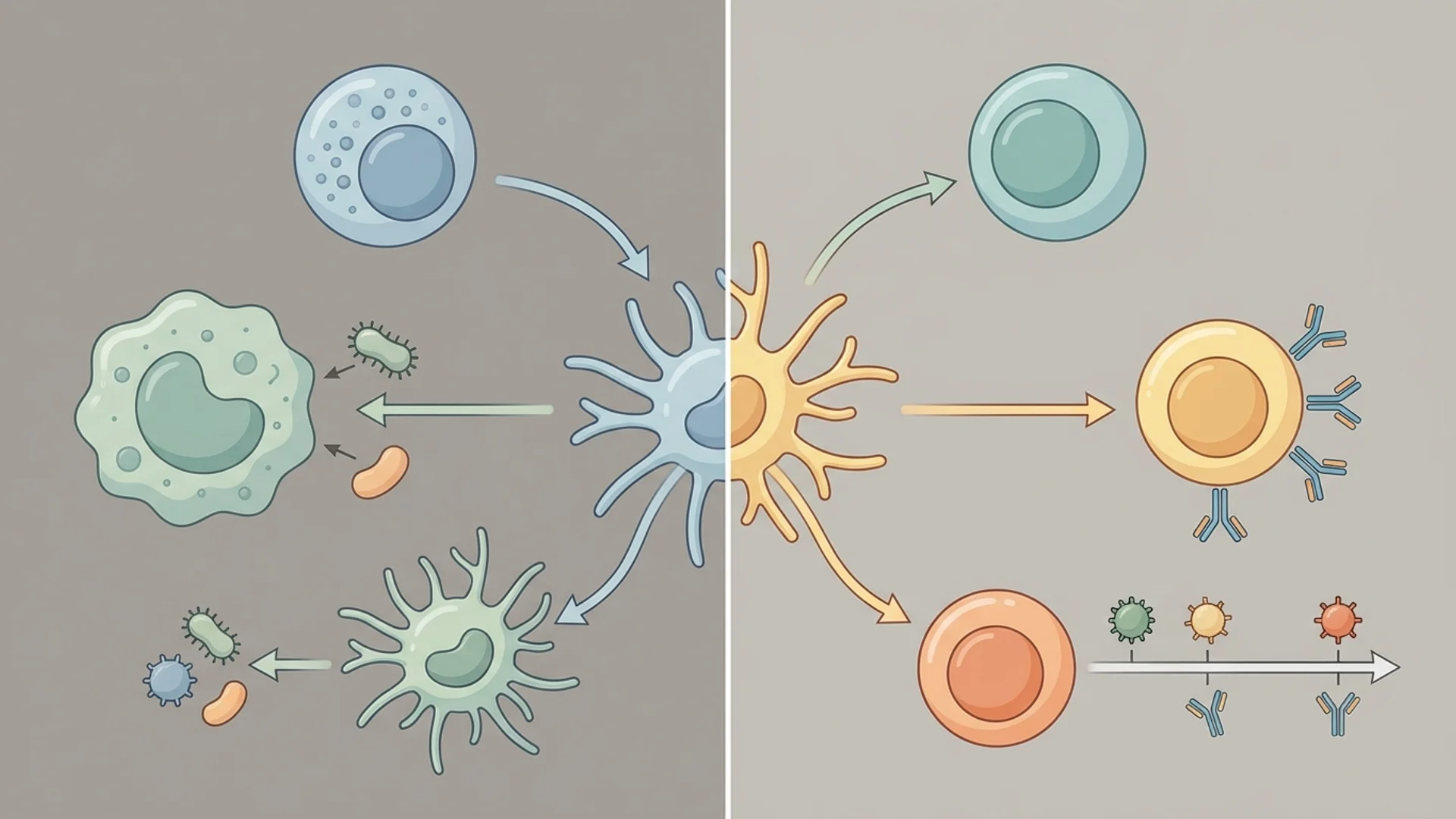
Innate vs. Adaptive Immunity Explained
How your two immune systems work together to defend against infection and disease. A clear explanation from Dr. Julian Douwes.
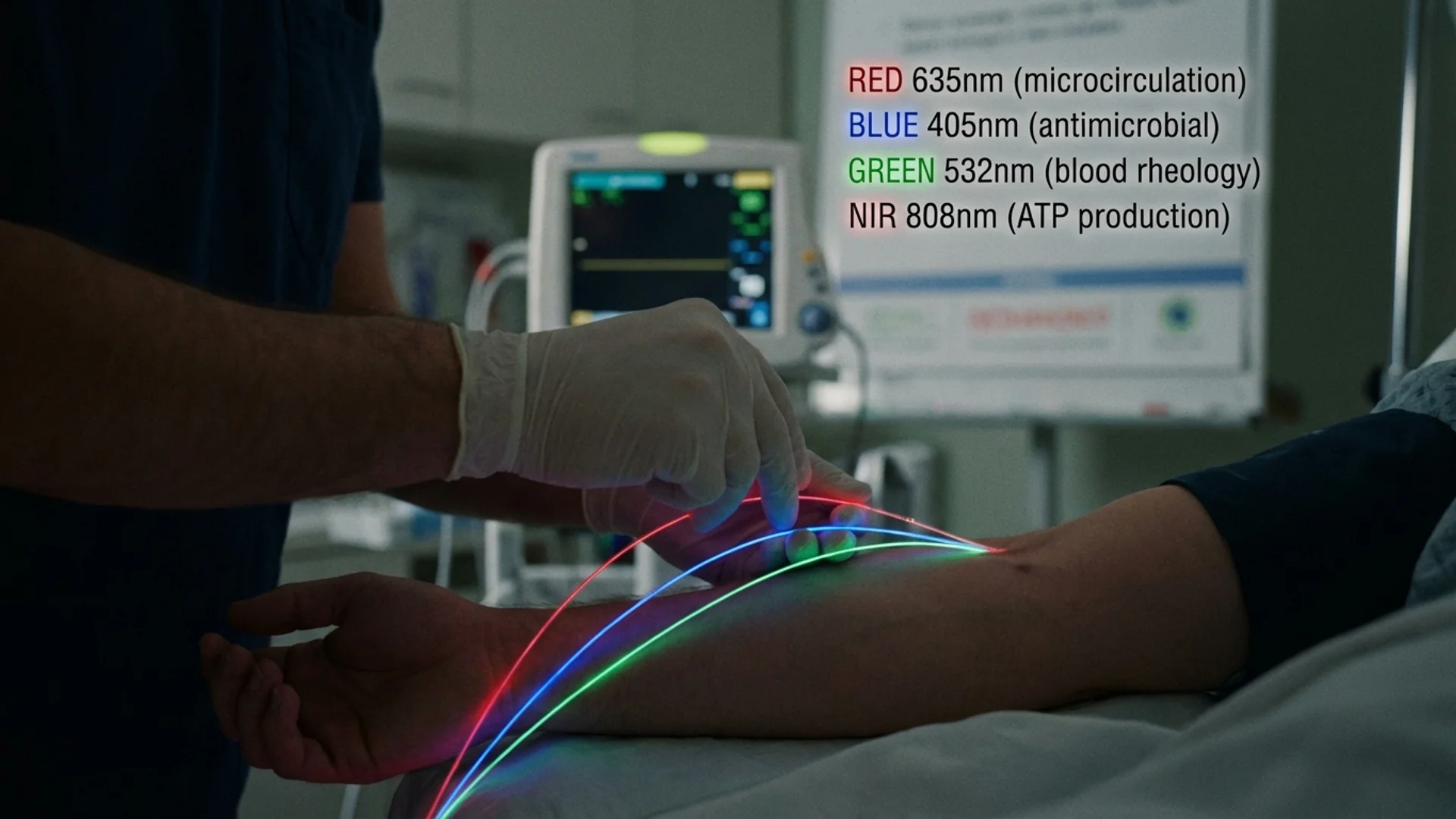
IV Laser Therapy and Immune Function
How intravenous laser therapy at different wavelengths affects immune cells. Evidence, mechanisms, and clinical applications by Dr. Julian Douwes.
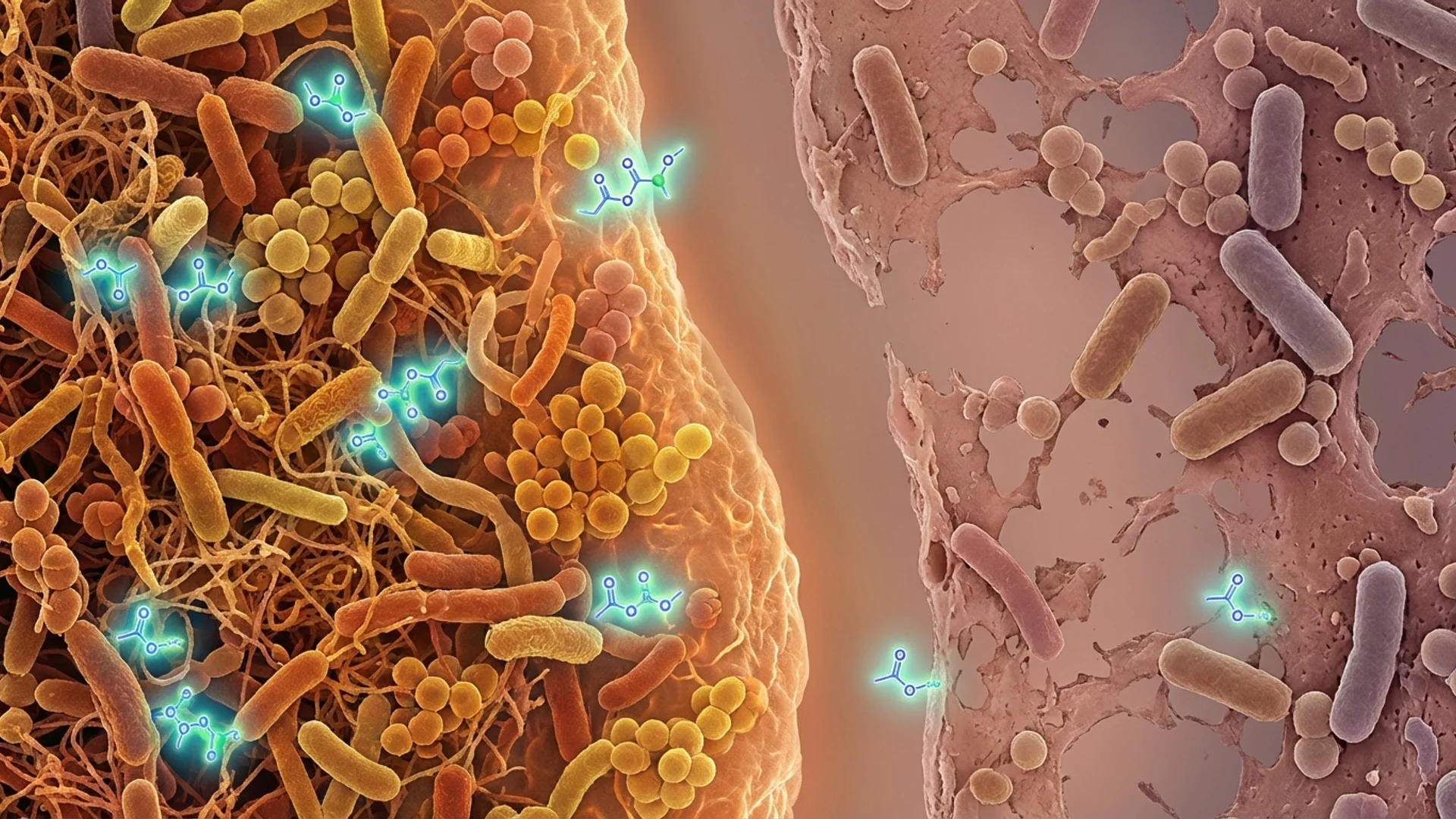
Microbiome and Immunity: A Clinical Guide
How gut microbial diversity shapes immune function, and what testing and restoration strategies the evidence supports. By Dr. Julian Douwes.
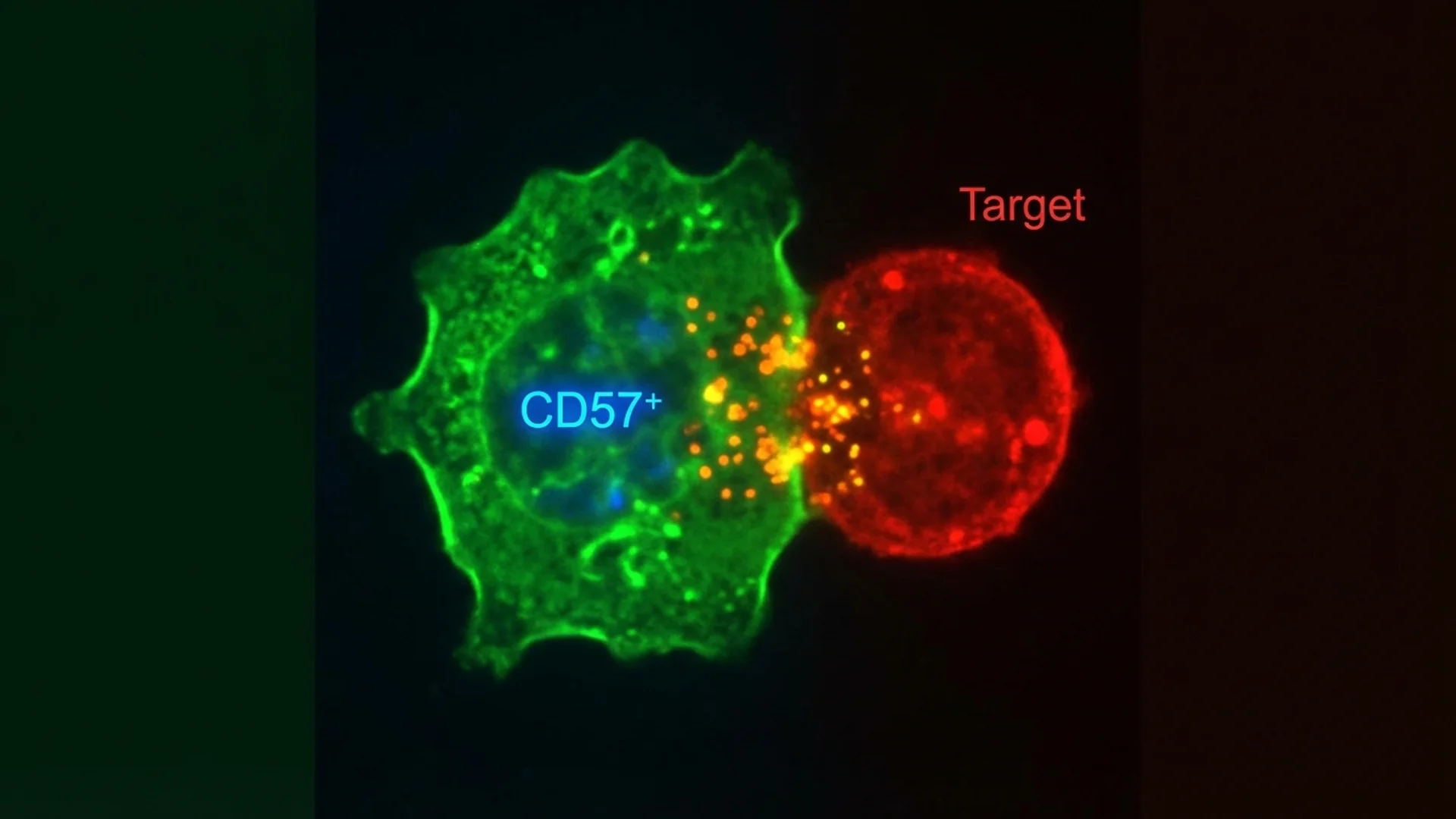
NK Cells: Natural Killer Cells and CD57
What NK cells do, why CD57 matters in Lyme disease, and how to support natural killer cell function. By Dr. Julian Douwes.
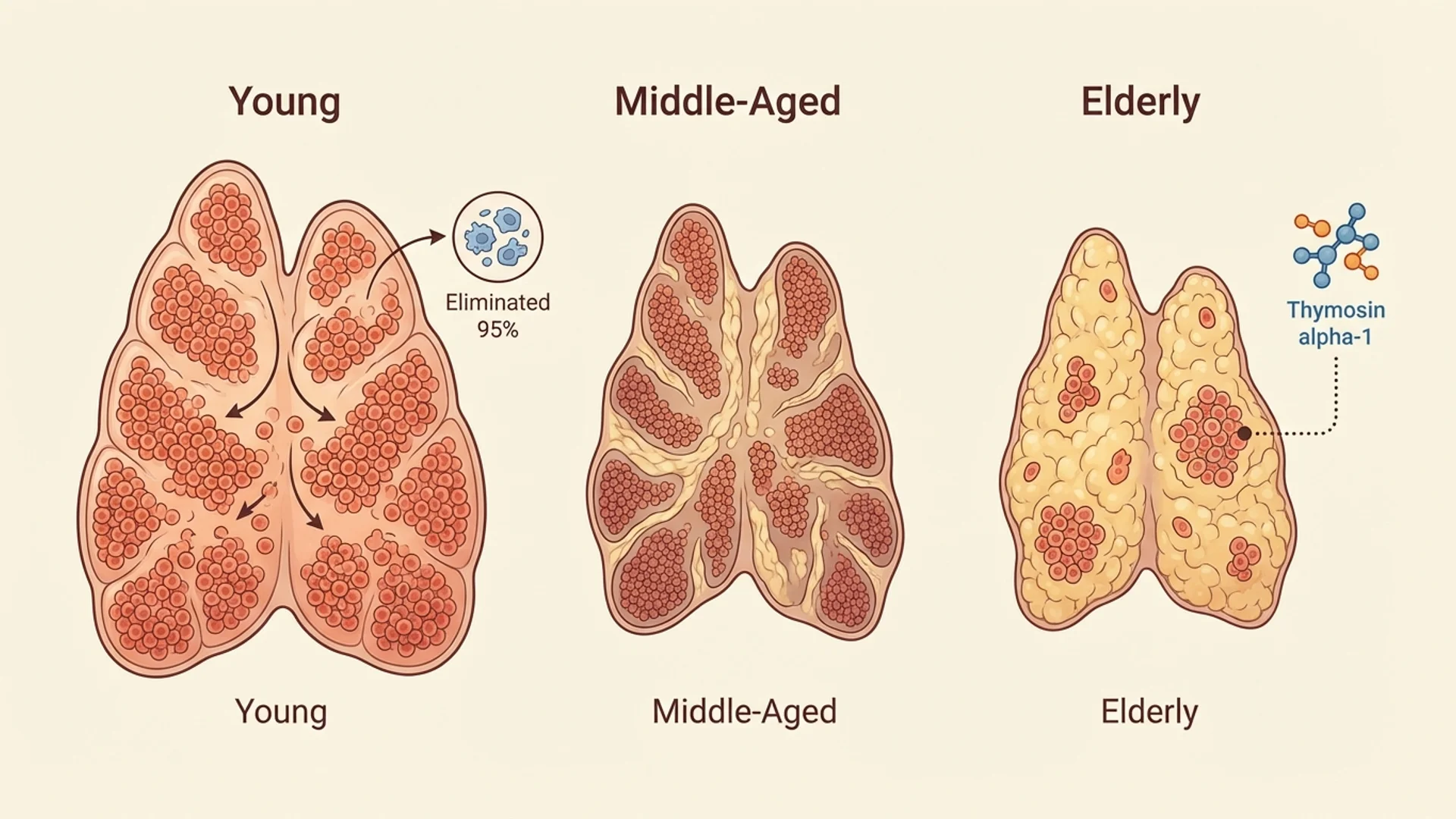
Thymus Function and T-Cell Health
How the thymus gland shapes immunity, why it declines with age, and what thymic peptide therapy can offer. By Dr. Julian Douwes.
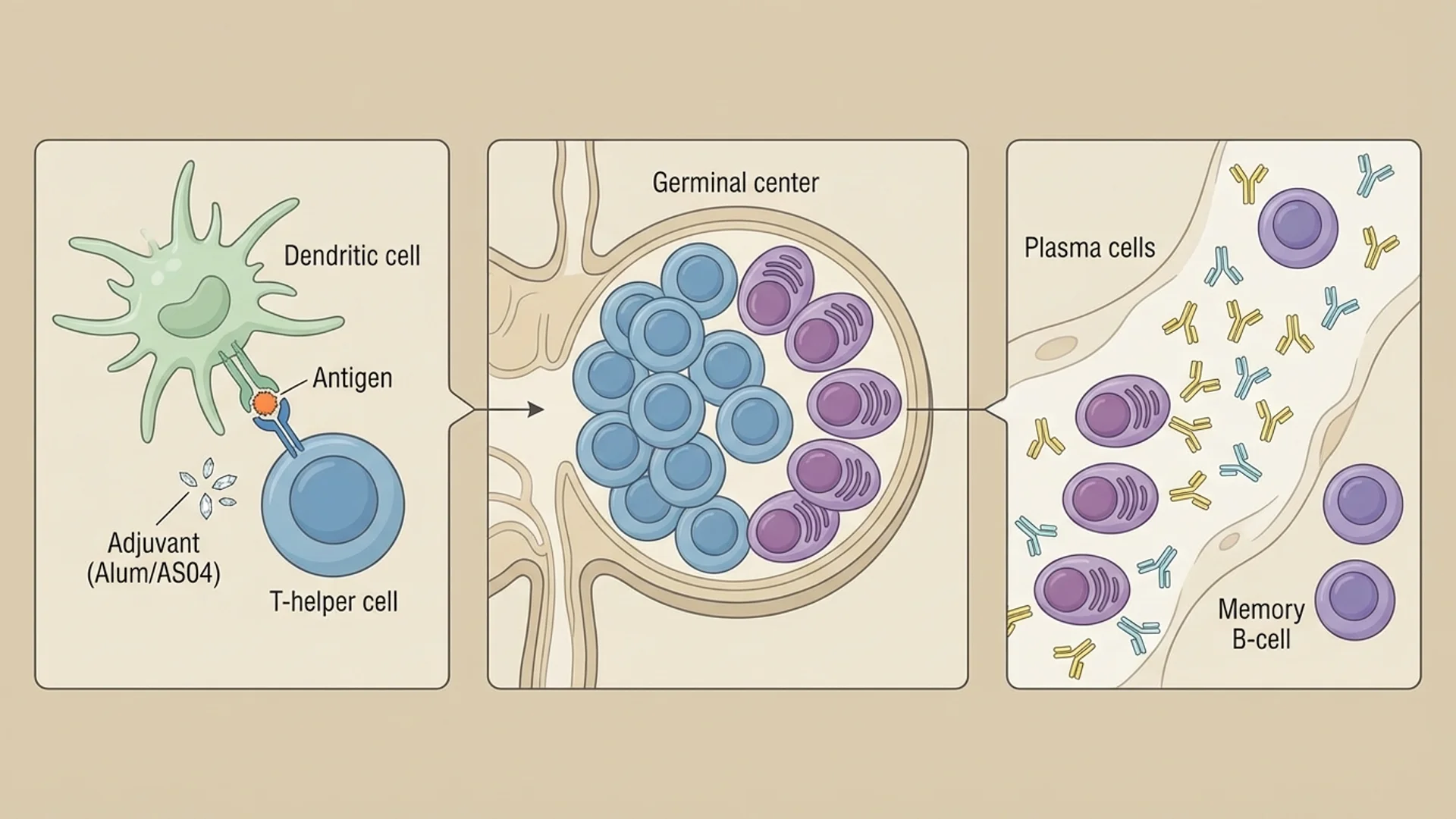
How Vaccines Interact with the Immune System
An evidence-based explanation of how vaccines work immunologically, including adjuvants, memory, and individual variation. By Dr. Julian Douwes.

Anti-Inflammation Protocol
A physician's evidence-based protocol for reducing chronic inflammation through diet, lifestyle, and targeted supplementation.

Immune Support Protocol: Seasonal and Travel
A tiered protocol for immune support -- seasonal prevention, pre-travel preparation, and acute illness response. By Dr. Julian Douwes.
Complete Guide
Your Immune System: A Physician's Guide
In-depth reference by Dr. Julian Douwes
Your Immune System: A Physician’s Guide
By Dr. Julian Douwes, M.D. — Chief Medical Officer, Klinik St. Georg
The immune system is the most sophisticated defense network in biology. It distinguishes self from non-self across trillions of cells, remembers threats it encountered decades ago, and adapts in real time to novel pathogens it has never seen before. It does all of this simultaneously, continuously, without conscious input.
And yet, for a system this remarkable, most patients — and many physicians — have only a rudimentary understanding of how it actually works.
I spend a significant portion of my clinical practice treating patients with immune dysfunction: chronic Lyme disease, post-COVID syndromes, autoimmune conditions, chronic fatigue, recurrent infections, and cancer. What I have learned over the years is that the immune system is rarely doing nothing. When patients are sick, the immune system is almost always doing something — it is just doing the wrong thing, or the right thing at the wrong time, or the right thing in the wrong place. Understanding this distinction matters, because the treatment approach changes entirely depending on what the immune system is actually doing.
This guide is my attempt to explain the immune system the way I explain it to patients in clinic — with enough detail to be genuinely useful, without the jargon that makes immunology textbooks impenetrable. Whether you are a patient trying to understand your own condition, a health professional looking for an integrative perspective, or simply someone who wants to understand the system that keeps you alive, this is written for you.
The Architecture of Immunity
Your immune system is not a single organ. It is a distributed network that includes the bone marrow, thymus, spleen, lymph nodes, tonsils, Peyer’s patches in the gut, and circulating white blood cells. Each component has a specific role, and they communicate through an extraordinarily complex signaling network of cytokines, chemokines, and cell-surface receptors.
The functional architecture divides into two broad systems:
Innate Immunity: The First Responders
The innate immune system is ancient, evolutionarily speaking. It is the system we share with insects, plants, and virtually every multicellular organism. It responds within minutes to hours, recognizes broad categories of threat rather than specific pathogens, and does not improve with repeated exposure.
Key players in innate immunity include:
- Neutrophils — the most abundant white blood cells, first to arrive at sites of infection, effective at killing bacteria but short-lived
- Macrophages — longer-lived cells that engulf pathogens, present antigens to adaptive immune cells, and orchestrate the inflammatory response
- Natural killer (NK) cells — specialized in destroying virus-infected cells and cancer cells without prior sensitization
- Dendritic cells — the bridge between innate and adaptive immunity, responsible for capturing antigens and presenting them to T cells
- The complement system — a cascade of proteins that can directly destroy pathogens, recruit immune cells, and enhance phagocytosis
- Physical barriers — skin, mucous membranes, stomach acid, and the intestinal epithelium
The innate system operates on pattern recognition. It does not need to have seen a specific pathogen before. Instead, it recognizes conserved molecular patterns common to broad categories of microorganisms — bacterial cell wall components, viral nucleic acids, fungal polysaccharides. These pattern recognition receptors (particularly toll-like receptors, or TLRs) trigger immediate defensive responses.
Adaptive Immunity: The Precision System
The adaptive immune system is unique to vertebrates and takes days to weeks to mount a full response, but it is extraordinarily specific and creates lasting memory.
Two primary cell types drive adaptive immunity:
- T cells (matured in the thymus) — include helper T cells (CD4+) that coordinate the immune response, cytotoxic T cells (CD8+) that directly kill infected cells, and regulatory T cells (Tregs) that prevent excessive immune activation
- B cells (matured in bone marrow) — produce antibodies, which are protein molecules that bind to specific antigens with remarkable precision
The adaptive system’s power comes from its ability to generate an almost infinite diversity of receptors through a process called V(D)J recombination. Your body can produce antibodies and T cell receptors that recognize virtually any molecular structure — including molecules that do not yet exist in nature. This is not metaphor. The combinatorial mathematics of immune receptor generation create a repertoire estimated at over 10^18 possible configurations.
When the adaptive system encounters a pathogen for the first time, the response is slow — five to seven days for a primary immune response. But a subset of activated cells become memory cells that persist for years or decades. The second encounter with the same pathogen triggers a response that is faster, stronger, and more targeted. This is the principle behind vaccination.
The Immune System in Communication
One of the most important concepts in modern immunology is that the immune system is fundamentally a communication system. It does not just attack and defend. It listens, interprets, and decides.
Cytokines: The Immune Language
Cytokines are signaling proteins that immune cells use to communicate with each other and with virtually every other tissue in the body. The cytokine network is the reason immune dysfunction produces symptoms that seem unrelated to immunity — fatigue, brain fog, mood changes, pain sensitivity.
Key cytokine categories include:
- Pro-inflammatory cytokines (IL-1, IL-6, TNF-alpha, IFN-gamma) — amplify the immune response, promote inflammation, signal the brain to produce sickness behavior (fatigue, reduced appetite, social withdrawal)
- Anti-inflammatory cytokines (IL-10, TGF-beta, IL-4) — resolve inflammation, promote tissue repair, prevent autoimmune responses
- Th1/Th2/Th17/Treg balance — different T helper cell subtypes produce different cytokine profiles, and the balance between them determines whether the immune response is cell-mediated (Th1), antibody-mediated (Th2), inflammatory (Th17), or regulatory (Treg)
In my clinical experience, the patients who struggle most are those whose cytokine signaling has become chronically dysregulated — persistently elevated pro-inflammatory cytokines without adequate anti-inflammatory counterbalance. This is the signature of chronic inflammation, and it underlies conditions ranging from autoimmunity to post-COVID syndrome to cancer-related fatigue.
Where the Immune System Lives
The Gut: 70% of Immune Tissue
Approximately 70% of the body’s immune tissue resides in the gastrointestinal tract — specifically in the gut-associated lymphoid tissue (GALT). This makes anatomical sense: the gut is the largest surface area exposed to the external environment, and it must constantly distinguish between harmless food antigens, beneficial commensal bacteria, and genuine pathogens.
The relationship between the gut microbiome and immune function is bidirectional. The microbiome educates the immune system during early development, teaching it what to tolerate and what to attack. In return, the immune system shapes the microbiome, selectively promoting beneficial species and controlling potentially harmful ones.
When this relationship breaks down — through antibiotic overuse, dietary changes, chronic stress, or infection — the consequences extend far beyond digestive symptoms. Gut dysbiosis has been linked to autoimmune disease, allergic disease, metabolic syndrome, and neurological conditions through well-characterized immunological mechanisms.
The Thymus: Immune Education
The thymus gland, located behind the sternum, is where T cells mature and undergo selection. During this process, T cells that react too strongly to self-antigens are eliminated (negative selection), while those that can recognize foreign antigens effectively are allowed to mature (positive selection).
The thymus begins involuting (shrinking) after puberty, and by age 50, most thymic tissue has been replaced by fat. This thymic involution is one of the primary reasons immune function declines with age — the supply of new, naive T cells diminishes, and the immune system increasingly relies on existing memory T cells. This has implications for both infection susceptibility and cancer surveillance.
Thymic peptides — particularly thymulin and thymosin alpha-1 — have been studied as a means of partially restoring thymic function. Thymosin alpha-1 is approved as a pharmaceutical in over 30 countries for immune modulation. In my practice, thymic peptide therapy is one of several tools we use to support immune function in patients with age-related immune decline or chronic infection.
Bone Marrow: The Factory
All blood cells, including immune cells, originate from hematopoietic stem cells in the bone marrow. The bone marrow produces approximately 500 billion blood cells daily, including neutrophils, monocytes, lymphocyte precursors, and platelets. Nutritional status, toxin exposure, chronic infection, and aging all affect bone marrow function, and by extension, immune cell production.
Immune Dysfunction: What Goes Wrong
In clinical practice, immune dysfunction falls into several broad categories:
1. Immunodeficiency: Not Enough Response
Primary immunodeficiency diseases are genetic and relatively rare. Secondary immunodeficiency — caused by malnutrition, chronic infection, medications, stress, or aging — is far more common and frequently underdiagnosed.
Signs that warrant investigation include recurrent infections (more than three to four per year requiring antibiotics), infections that are unusually severe or slow to resolve, and opportunistic infections that a healthy immune system would control.
2. Autoimmunity: Misdirected Response
Autoimmune disease occurs when the immune system attacks the body’s own tissues. There are over 80 recognized autoimmune conditions, and their prevalence is increasing in industrialized nations — a trend that cannot be explained by genetics alone and is almost certainly driven by environmental factors.
The mechanisms are complex and involve molecular mimicry (pathogens sharing structural similarities with self-antigens), loss of regulatory T cell function, gut barrier dysfunction (allowing bacterial products to enter the bloodstream and trigger immune activation), and chronic infection driving persistent immune stimulation.
3. Chronic Inflammation: Stuck in the “On” Position
Chronic, low-grade inflammation is arguably the most common form of immune dysfunction I see in clinical practice. It is not a disease in itself but a state that predisposes to virtually every chronic disease — cardiovascular disease, neurodegenerative disease, cancer, metabolic syndrome, depression.
The drivers are well characterized: visceral adiposity, gut dysbiosis, chronic infections (including dental infections), environmental toxin exposure, chronic psychological stress, sleep deprivation, and a pro-inflammatory diet. The solution is rarely a single intervention. It requires addressing multiple drivers simultaneously.
4. Immune Exhaustion: Worn Out by Chronic Stimulation
This is a pattern I see frequently in chronic Lyme disease and post-COVID patients. The immune system has been fighting a chronic infection or persistent inflammatory stimulus for so long that its cells become functionally impaired. T cells upregulate exhaustion markers (PD-1, LAG-3, TIM-3) and lose their ability to mount effective responses. NK cell activity declines. The patient becomes simultaneously over-inflamed and under-defended.
This is where integrative approaches have particular value. Conventional medicine has limited tools for immune exhaustion outside of oncology (where checkpoint inhibitor therapy addresses similar mechanisms). Integrative approaches — including IV therapies, hyperthermia, thymic peptides, and targeted nutritional support — offer additional options for restoring immune cell function.
An Integrative Approach to Immune Health
Here is what I tell my patients about maintaining immune function. This is not a protocol; it is a framework for thinking about immune health:
Foundation (strongest evidence):
- Sleep — 7-9 hours, consistent timing. Sleep deprivation for even a single night reduces NK cell activity by approximately 70% (human data, Irwin et al.). This is not negotiable.
- Exercise — moderate, regular physical activity enhances immune surveillance. Excessive exercise without adequate recovery can be immunosuppressive.
- Nutrition — adequate protein (essential for antibody and immune cell production), micronutrient sufficiency (zinc, selenium, vitamin D, vitamin C, vitamin A), and a diverse plant-rich diet that supports gut microbial diversity.
- Stress management — chronic cortisol elevation suppresses cellular immunity while promoting inflammatory pathways. The data on this is Level 1.
Targeted support (moderate to strong evidence):
- Vitamin D — 25(OH)D levels below 30 ng/mL are associated with impaired immune function. The relationship between vitamin D and immune regulation is supported by extensive human data. Target 40-60 ng/mL.
- Zinc — essential cofactor for over 300 enzymes including those critical for immune cell function. Deficiency is common, particularly in older adults, and impairs both innate and adaptive immunity. Supplementation at 15-30 mg daily is reasonable for most adults.
- Gut health — the connection between gut integrity, microbiome diversity, and immune function is one of the most important themes in modern medicine. Address it.
Advanced interventions (clinical context required):
- IV therapies — high-dose intravenous vitamin C, glutathione, and micronutrient formulations can provide pharmacological effects not achievable through oral supplementation. In my practice, these are used in the context of specific clinical indications, not as general wellness measures.
- Immune modulation therapies — hyperthermia, thymic peptides, mistletoe extract (Viscum album), and other modalities that modulate immune function. These require physician supervision and are tailored to individual patient needs.
- Functional diagnostics — lymphocyte subset panels, NK cell function testing, cytokine profiling, and other assessments that provide a detailed map of immune function beyond what a standard CBC offers.
The Honest Uncertainties
I want to be transparent about what we do not fully understand:
The immune system is the most complex biological system we have attempted to characterize, and our understanding remains incomplete. We do not fully understand why some people develop autoimmune disease and others do not, even when exposed to the same environmental triggers. We cannot reliably predict which post-COVID patients will develop long-term immune dysregulation. We do not have a comprehensive model for how the hundreds of identified cytokines interact in vivo.
What we do have is a sophisticated and growing understanding of immune function that allows us to make evidence-based clinical decisions for most patients most of the time. The gap between what immunology knows in the laboratory and what clinical medicine applies at the bedside remains significant, but it is narrowing — and integrative medicine, at its best, is working in that gap.
Where to Go From Here
This article provides a framework. The specific topics are explored in depth across this series:
- Innate vs. Adaptive Immunity — the two systems in detail
- Autoimmune Disease — mechanisms, triggers, and treatment
- Immune Modulation — how we enhance or calm the immune system
- The Gut-Immune Axis — why 70% of immunity lives in the gut
- Chronic Inflammation — the root of chronic disease
- NK Cells and CD57 — natural killer cells in infection and cancer
- Cytokine Storms — when immunity turns dangerous
Understanding your immune system is not an academic exercise. It is the foundation for understanding your health, your disease, and the rationale behind the treatments your physicians recommend. The more you understand, the better the conversations you can have with your medical team, and the better decisions you can make about your own care.
Disclaimer: This article is provided for educational purposes and reflects one physician’s clinical perspective. It is not a substitute for individualized medical care. Consult a qualified physician before making decisions about your health based on this information.
