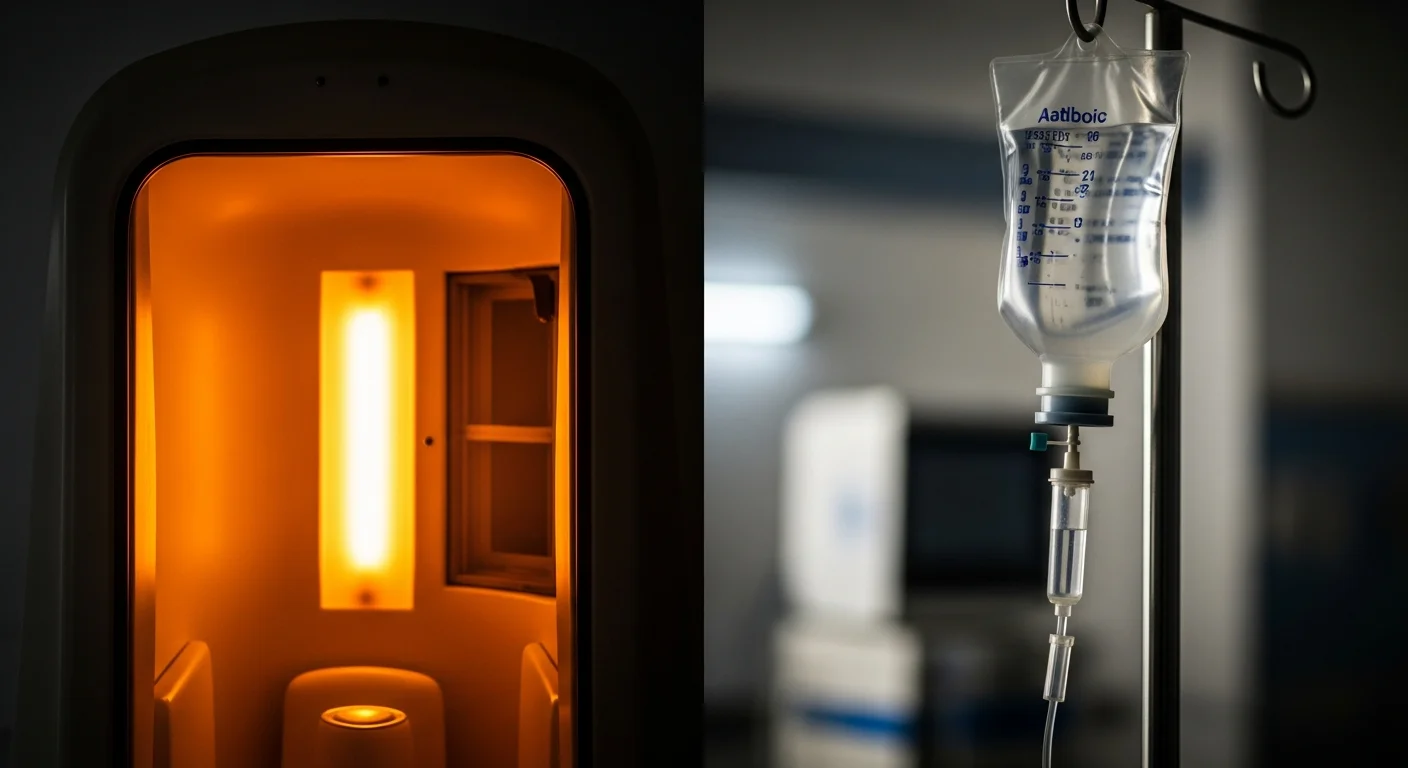
If you have been diagnosed with Lyme disease — or suspect persistent Borrelia infection despite prior antibiotic treatment — you are facing a decision that most physicians in the United States will not even present to you. The standard approach is IV antibiotics. The alternative, available primarily at specialized clinics in Germany and parts of Europe, is whole-body hyperthermia. These are not equivalent treatments for the same situation. They work through entirely different mechanisms, carry different evidence profiles, and suit different clinical stages.
Here is what the evidence shows, and how I think about choosing between them — drawing on Klinik St. Georg’s experience treating Lyme patients since the mid-1990s.
At a Glance
| Feature | IV Antibiotics | Whole-Body Hyperthermia |
|---|---|---|
| Mechanism | Bactericidal or bacteriostatic disruption of Borrelia metabolism | Direct thermal killing of Borrelia (heat-sensitive above 41 degrees C) |
| Standard protocol | Ceftriaxone 2g/day IV for 14-28 days | 2 sessions at 41.6-42 degrees C, 6-8 hours each, 48 hours apart |
| Evidence level | Strong (multiple RCTs for early Lyme) | Emerging (clinical series, mechanistic evidence, no RCTs) |
| Best for | Early-stage Lyme, acute disseminated Lyme | Persistent/chronic Lyme, antibiotic-refractory cases |
| Treatment duration | 2-4 weeks (may extend) | 2 sessions over 3-4 days |
| Availability | Worldwide | Primarily Germany and select European clinics |
| Approximate cost | $2,000-8,000 (US, with insurance variable) | $15,000-25,000 (including clinic stay in Germany) |
| Recurrence concern | 10-20% post-treatment Lyme disease syndrome | Limited long-term data; clinical series suggest low recurrence |
How IV Antibiotics Work Against Borrelia
Intravenous antibiotics have been the cornerstone of Lyme disease treatment since the 1980s. The rationale is straightforward: deliver bactericidal concentrations of antibiotic directly to the bloodstream to reach disseminated spirochetes.
The standard regimens:
- Ceftriaxone (Rocephin): 2 grams IV daily for 14-28 days. This is the first-line IV choice with the most clinical data. Ceftriaxone achieves good CNS penetration, which matters because Borrelia can cross the blood-brain barrier.
- Cefotaxime: An alternative third-generation cephalosporin, sometimes preferred for patients with biliary complications from ceftriaxone.
- Penicillin G: IV penicillin was the original treatment but has largely been superseded by ceftriaxone due to convenience and tissue penetration.
How they kill Borrelia: Beta-lactam antibiotics (ceftriaxone, cefotaxime) inhibit bacterial cell wall synthesis by binding penicillin-binding proteins. Borrelia burgdorferi has a relatively slow replication cycle (12-24 hours, compared to minutes for many bacteria), which means antibiotic exposure must be sustained over weeks to catch spirochetes during active division.
What the evidence supports: The IDSA (Infectious Diseases Society of America) guidelines, based on multiple randomized controlled trials, support 14-28 days of IV ceftriaxone for Lyme neuroborreliosis, Lyme carditis, and antibiotic-refractory Lyme arthritis (Wormser et al., 2006). For early localized Lyme, oral doxycycline is typically sufficient.
The problem: For a subset of patients, standard antibiotic courses do not resolve symptoms. Post-treatment Lyme disease syndrome (PTLDS) affects an estimated 10-20% of treated patients. Whether this represents persistent infection, post-infectious immune dysregulation, or residual tissue damage remains one of the most contentious debates in infectious disease medicine.
How Whole-Body Hyperthermia Works Against Borrelia
Whole-body hyperthermia (WBH) takes a fundamentally different approach: instead of chemically disrupting Borrelia’s metabolism, it exploits the spirochete’s vulnerability to heat.
The thermal biology of Borrelia:
Borrelia burgdorferi is a mesophilic organism that thrives at temperatures between 33 and 37 degrees C — the normal temperature range of the human body and the tick vector. Crucially, laboratory studies have demonstrated that Borrelia becomes metabolically impaired above 39 degrees C and loses viability above 41 degrees C (Reisinger et al., 2006). At 41.6-42 degrees C, maintained for several hours, spirochete death occurs through protein denaturation and membrane destabilization.
The treatment protocol:
In my clinical experience, the hyperthermia protocol for Lyme typically involves:
- Pre-treatment preparation: 2-3 days of antibiotic loading (usually doxycycline and azithromycin) to weaken spirochete defenses and address co-infections that may be less heat-sensitive.
- Session 1: Core body temperature raised to 41.6-42 degrees C under general anesthesia, maintained for 6-8 hours using infrared water-filtered-A radiation. Continuous ICU-level monitoring of cardiac function, oxygenation, electrolytes, and organ function.
- 48-hour recovery period: During which the immune system mounts a vigorous response to the heat-damaged spirochetes.
- Session 2: Repeat hyperthermia session. The second session targets spirochetes that may have been in biofilm-protected niches or tissue compartments that were less uniformly heated during session 1.
- Post-treatment support: Continued antibiotics for 7-14 days, detoxification support, immune modulation.
Why two sessions? Borrelia is known to exist in multiple morphological forms — the classic spirochete, round bodies (cysts), and biofilm-associated persister forms. A single hyperthermia session may not penetrate all tissue compartments uniformly. The second session, performed 48 hours later, catches organisms that may have been in protected niches during the first.
Safety: This is not a mild fever therapy. Maintaining a core temperature of 42 degrees C for 6-8 hours is a serious medical procedure requiring general anesthesia, mechanical ventilation, and continuous ICU-level monitoring. It is performed by teams with specific training in hyperthermia medicine. The procedure should only be undertaken at facilities with deep experience in this modality.
Head-to-Head Comparison
| Parameter | IV Antibiotics | Whole-Body Hyperthermia |
|---|---|---|
| Mechanism of Borrelia killing | Cell wall disruption (requires active replication) | Thermal denaturation (kills regardless of replication state) |
| Effect on persister forms | Limited (persisters are metabolically dormant) | Strong (heat kills regardless of metabolic state) |
| Effect on biofilms | Poor penetration into biofilm matrix | Heat penetrates biofilms; may disrupt matrix |
| CNS penetration | Ceftriaxone: moderate; some drugs: poor | Core temperature elevation is systemic, including CNS |
| Treatment of co-infections | Must add specific agents for each co-infection | Heat affects multiple pathogens simultaneously; some co-infections less heat-sensitive |
| Duration of treatment | 14-28 days minimum | 3-4 days (2 sessions + recovery) |
| Herxheimer reaction | Common, manageable | Can be intense; managed under anesthesia/monitoring |
| Published RCTs | Multiple (for early/disseminated Lyme) | None (clinical series and case reports) |
| Side effects | GI disruption, C. difficile risk, PICC complications, allergic reactions | Procedure-related (anesthesia risks, electrolyte shifts, transient organ stress) |
| Insurance coverage | Partial to full (US/EU) | Generally not covered; out-of-pocket |
| Recurrence rate | 10-20% PTLDS rate | Insufficient long-term data; clinical observation suggests lower |
When I Recommend IV Antibiotics
IV antibiotics remain the appropriate first-line treatment in these situations:
- Early disseminated Lyme disease — new diagnosis with neurological involvement (facial palsy, meningitis), cardiac involvement (heart block), or severe arthritis. The evidence base here is solid, and response rates are high.
- First-line treatment for any confirmed Lyme diagnosis — before considering hyperthermia, a standard antibiotic course should be attempted. Many patients respond well and do not need more intensive intervention.
- When hyperthermia is contraindicated — significant cardiac disease, pregnancy, uncontrolled epilepsy, or other conditions that preclude general anesthesia at extreme core temperatures.
- Pediatric Lyme — hyperthermia protocols are primarily studied and performed in adults.
What I tell my patients: if you have a new Lyme diagnosis, start with antibiotics. They work for the majority of patients, and the evidence supporting them is the most robust of any Lyme treatment. Hyperthermia is not a first-line therapy — it is a tool for situations where first-line treatment has failed.
When I Recommend Whole-Body Hyperthermia
In my clinical experience, hyperthermia becomes the stronger option when:
- Standard antibiotic courses have failed — the patient has completed one or more rounds of IV antibiotics but continues to have objective signs of active infection (positive PCR, inflammatory markers, or clinical syndrome consistent with ongoing Borrelia activity).
- Persistent neurological Lyme symptoms — cognitive impairment, neuropathy, or neuropsychiatric symptoms that have not responded to IV ceftriaxone. The systemic heat penetration may reach CNS compartments more effectively than some antibiotics.
- Late-stage or chronic Lyme — patients diagnosed years after initial infection, where Borrelia has likely established biofilm communities and persister populations that are inherently antibiotic-resistant.
- Multiple co-infections — patients with concurrent Babesia, Bartonella, or other tick-borne co-infections. Hyperthermia provides a broad-spectrum thermal effect that can address multiple pathogens simultaneously, though some co-infections (particularly Babesia) may require additional targeted therapy.
- Patients seeking a defined treatment endpoint — the 2-session hyperthermia protocol offers a concentrated intervention, compared to months of rotating antibiotics.
Here is what the evidence shows: the mechanistic rationale for hyperthermia is sound — Borrelia’s thermal vulnerability is well-documented in vitro. The clinical data consists of case series and observational reports from German hyperthermia centers, not randomized trials. This is an important distinction. The outcomes I have observed are often dramatic, particularly in patients who had failed multiple antibiotic protocols, but I cannot point to a level-1 evidence base.
Can You Combine Them?
Yes — and in practice, they are almost always combined. The standard approach at experienced hyperthermia centers is to use antibiotics before, during, and after hyperthermia sessions. The rationale is synergistic:
Pre-hyperthermia antibiotics (loading phase):
- Doxycycline and/or azithromycin for 2-3 days before the first session
- Weakens spirochete cell walls, making them more vulnerable to thermal stress
- Addresses intracellular Borrelia that macrolides (azithromycin) target specifically
Concurrent approach:
- Antibiotics circulating during hyperthermia sessions benefit from enhanced tissue perfusion and increased metabolic activity at elevated temperatures
- Some antibiotics (tetracyclines, macrolides) have temperature-dependent activity curves that improve at higher temperatures
Post-hyperthermia antibiotics (consolidation):
- 7-14 days of oral antibiotics to address any surviving organisms in a weakened state
- Targets the immune cascade that hyperthermia triggers — massive release of Borrelia antigens stimulates both innate and adaptive immunity
In my clinical experience, the combination approach yields the best outcomes. Hyperthermia alone may leave some co-infections insufficiently treated. Antibiotics alone may not reach persister forms. Together, they address multiple pathogenic mechanisms simultaneously.
Clinical Perspective — Julian Douwes M.D.
My father, Friedrich Douwes, discovered the potential of hyperthermia for Lyme almost by accident. In 1994, he was treating a cancer patient with whole-body hyperthermia — a treatment he pioneered in oncology — and the patient happened to also have chronic Lyme disease. After the hyperthermia sessions, the Lyme symptoms improved dramatically. That serendipitous discovery launched what would become three decades of refining this approach at Klinik St. Georg. For early-stage Lyme, antibiotics work well and should remain first-line. But for the patient who has done two or three rounds of IV ceftriaxone and still cannot think clearly, still has joint pain, still has the fatigue that defines their daily life — that patient deserves to know that whole-body hyperthermia exists. It is not experimental in the sense of being untested — German clinics have performed thousands of procedures with documented outcomes. It is experimental in the sense of lacking randomized controlled trials, and I believe that distinction matters. What I can say is that the patients we have treated with hyperthermia after they failed standard antibiotics have shown improvement rates that antibiotics alone could not replicate. That is a clinical observation, not a clinical trial — but it is what drives our practice.
Key Takeaways
- IV antibiotics (primarily ceftriaxone) remain the evidence-based first-line treatment for Lyme disease with multiple supporting RCTs.
- Whole-body hyperthermia exploits Borrelia’s thermal vulnerability above 41 degrees C and is particularly suited to persistent or antibiotic-refractory Lyme.
- Hyperthermia has mechanistic support and clinical series data but lacks published randomized controlled trials.
- The two approaches are complementary — standard practice at hyperthermia centers includes antibiotic loading before and after hyperthermia sessions.
- Hyperthermia requires ICU-level monitoring under general anesthesia and should only be performed at experienced, specialized centers.
- For patients who have failed standard antibiotic treatment, hyperthermia offers a fundamentally different mechanism that addresses persister forms, biofilms, and heat-sensitive spirochetes in ways that antibiotics cannot.
- Cost and accessibility remain significant barriers — hyperthermia is primarily available in Germany and is generally not covered by insurance.
References
- Wormser, G.P., et al. “The clinical assessment, treatment, and prevention of Lyme disease, human granulocytic anaplasmosis, and babesiosis: clinical practice guidelines by the Infectious Diseases Society of America.” Clinical Infectious Diseases, 43(9), 2006, pp. 1089-1134.
- Reisinger, E.C., et al. “In vitro activity of thermotherapy against Borrelia burgdorferi.” International Journal of Hyperthermia, 12(1), 1996, pp. 133-137.
- Klempner, M.S., et al. “Two controlled trials of antibiotic treatment in patients with persistent symptoms and a history of Lyme disease.” New England Journal of Medicine, 345(2), 2001, pp. 85-92.
- Aucott, J.N., et al. “Post-treatment Lyme disease syndrome symptomatology and the impact on life functioning.” PeerJ, 1, 2013, e322.
- Donta, S.T. “Issues in the diagnosis and treatment of Lyme disease.” Open Neurology Journal, 6, 2012, pp. 140-145.