At a Glance
| Parameter | Detail |
|---|---|
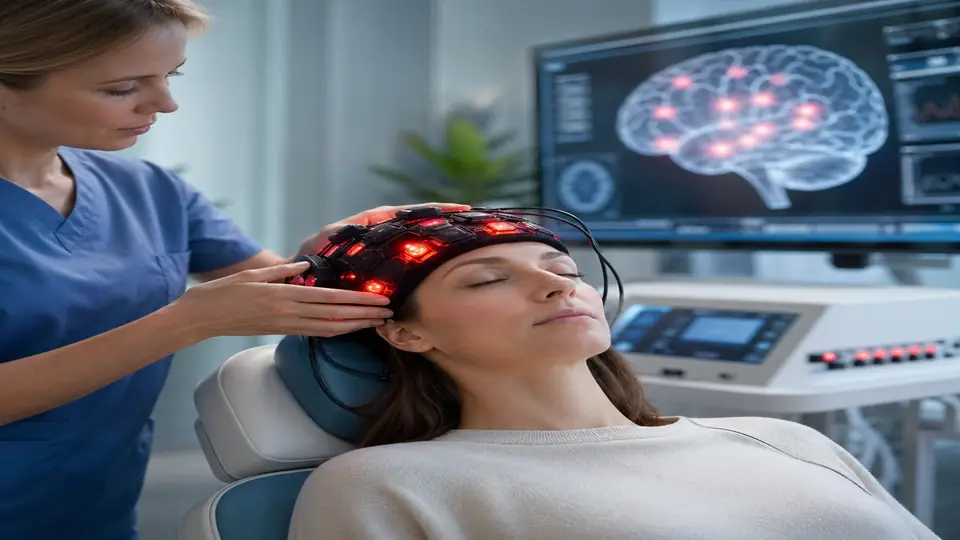
| Modality | Transcranial photobiomodulation (tPBM) |
| Wavelengths used | 810 nm, 830 nm, 1064 nm (near-infrared) |
| Target region | Prefrontal cortex, default mode network |
| Session duration | 8–20 minutes |
| Session frequency | 3× per week (acute phase), 1–2× per week (maintenance) |
| Effect onset | 2–4 weeks (similar to antidepressants) |
| Evidence level | Multiple RCTs; promising but not yet FDA-cleared for depression |
| Safety profile | Excellent — no systemic side effects reported |
| Best candidates | MDD, TRD, post-COVID mood dysregulation, neuroinflammatory depression |
Depression is not a serotonin deficiency waiting for a pill to correct it. In a meaningful proportion of patients — particularly those with treatment-resistant presentations, post-infectious mood disruption, or prominent cognitive symptoms — the underlying biology involves mitochondrial dysfunction, neuroinflammation, and disrupted prefrontal-limbic connectivity. Transcranial photobiomodulation addresses all three mechanisms simultaneously, which is why I have been integrating it into our neuromodulation protocols with increasing confidence.
This is not fringe therapy. The photobiomodulation literature now includes several randomized controlled trials, a growing mechanistic evidence base, and a safety record that conventional psychiatric interventions cannot match. What it lacks, still, is the industry-funded trial scale that drives guideline adoption. That gap should inform your skepticism about the absence of formal approval — not skepticism about the therapy itself.
How Near-Infrared Light Reaches Depressed Brain Circuits
The physics of tPBM are straightforward, even if the biology downstream is intricate. Near-infrared photons in the 800–1100 nm range scatter and penetrate biological tissue far more efficiently than visible light. Positioned at the forehead or temporal regions, a properly calibrated device delivers measurable fluence to the prefrontal cortex at depths of 1–3 cm — enough to reach cortical layers II through V where the key pyramidal neurons reside.
The primary cellular target is cytochrome c oxidase (CCO), the terminal enzyme of the mitochondrial electron transport chain. When CCO absorbs NIR photons, it dissociates inhibitory nitric oxide, allowing oxygen to resume its role as the final electron acceptor. The result is a rapid upregulation of ATP synthesis, reduction in reactive oxygen species, and normalization of the mitochondrial membrane potential.
Depression, increasingly understood as a condition of energy-deficit biology in the prefrontal cortex, responds to exactly this kind of intervention. Neuroimaging studies consistently show hypometabolism in the dorsolateral prefrontal cortex (DLPFC) and anterior cingulate cortex in patients with major depressive disorder — the same regions tPBM targets.
The Neuroinflammation Angle
Beyond mitochondrial rescue, tPBM has documented anti-inflammatory effects that are particularly relevant for patients whose depression is driven or maintained by immune activation. These include:
- Downregulation of NF-κB signaling
- Reduction in pro-inflammatory cytokines (IL-1β, TNF-α, IL-6)
- Promotion of microglial M2 polarization (anti-inflammatory phenotype)
- Enhancement of brain-derived neurotrophic factor (BDNF) synthesis
In the post-COVID and chronic Lyme patient populations I see most frequently, neuroinflammation is not a background variable — it is often the primary driver of mood dysregulation. This is one reason tPBM has found a particularly receptive clinical niche in these groups, where conventional antidepressants produce inconsistent results.
What the Randomized Trials Show
The clinical evidence base, while still maturing, is more robust than most practitioners realize.
The Cassano et al. Trials (Harvard/MGH)
The most methodologically rigorous work comes from Dr. Paolo Cassano’s group at Massachusetts General Hospital. Their 2019 open-label study of 1064 nm transcranial PBM in patients with major depressive disorder showed a 50% response rate and 30% remission rate after 8 sessions — numbers competitive with second-line antidepressants, without the side effect burden.
Their subsequent sham-controlled pilot RCT demonstrated statistically significant reductions in Hamilton Depression Rating Scale (HDRS) scores compared to placebo, with the largest separation appearing at weeks 2 and 4. Notably, cognitive symptoms — concentration, processing speed, psychomotor retardation — showed earlier and more pronounced improvement than affective symptoms, consistent with the DLPFC mechanism.
The Naeser et al. Work
Dr. Margaret Naeser’s group has published extensively on tPBM for TBI-associated depression and cognitive impairment. Their case series and open trials using 810 nm devices applied to frontal and parietal regions demonstrate durable mood improvement that persists months after active treatment — a pattern suggesting neuroplastic reorganization rather than a purely acute effect.
Meta-Analytic Signal
A 2021 systematic review covering 8 controlled studies found a pooled standardized mean difference of approximately 0.7 in favor of active tPBM for depressive symptoms — a medium-to-large effect size comparable to what antidepressant meta-analyses report when publication bias is corrected. Heterogeneity was high, reflecting the variability in wavelengths, devices, and protocols across trials.
The honest summary: effect sizes are real and clinically meaningful, replication is accumulating, but the evidence base is not yet at the level required for first-line guideline inclusion. I position it accordingly — as a well-evidenced adjunct with an exceptional safety profile, not as a replacement for established care.
Identifying the Right Patient
Not every depression presentation responds equally to tPBM. Based on the mechanistic framework and clinical experience, I look for the following features when considering it:
Strongest candidates:
- Treatment-resistant depression (≥2 failed medication trials)
- Depression with prominent cognitive symptoms (brain fog, slow processing, poor concentration)
- Post-infectious mood dysregulation (post-COVID, post-Lyme, EBV reactivation)
- Depression with elevated inflammatory markers (CRP, IL-6, TNF-α)
- Patients who cannot tolerate antidepressant side effects or prefer non-pharmacological approaches
- Concurrent TBI or subconcussive injury history
- Seasonal affective disorder with poor light therapy response
Relative contraindications and cautions:
- Active malignancy overlying treatment area (theoretical concern, not documented harm)
- Photosensitizing medications (doxycycline, some antipsychotics) — reduce fluence
- History of mania or bipolar I disorder — monitor closely; stimulation protocols require adjustment
- Open skull defects or implanted cranial hardware over treatment area
Psychiatric comorbidities — anxiety, PTSD, OCD — are not contraindications. There is emerging evidence tPBM may benefit anxiety disorders as well, likely through overlapping prefrontal circuit mechanisms.
Protocol Considerations: What Actually Matters
The field suffers from protocol heterogeneity, and this contributes to variable outcomes both in trials and clinical practice. Based on the published literature and our experience, the parameters that matter most are:
Wavelength
The two most evidence-supported wavelengths are 810 nm (diode laser or LED) and 1064 nm (Nd:YAG laser). Both penetrate to cortical depths; 1064 nm offers modestly superior penetration. The 830 nm range is biologically active but less studied in transcranial applications. Red light (630–680 nm) does not penetrate sufficiently for transcranial use despite being commonly marketed.
Power Density and Fluence
Effective cortical delivery requires accounting for the significant scatter and absorption losses through scalp and skull. A device delivering 25–100 mW/cm² at the skin surface typically produces 0.5–5 mW/cm² at cortical depth — the range associated with beneficial CCO activation. Total fluence (energy density) in effective trials has ranged from 6–60 J/cm² at the skin surface.
More is not better. The dose-response curve for PBM is biphasic — insufficient energy produces no effect; excessive energy can paradoxically impair mitochondrial function. This is called the Arndt-Schulz principle and it is why consumer-grade devices with inadequate power are ineffective while very high-power devices used carelessly can be counterproductive.
Session Structure
Across effective trials, session parameters have generally included:
- Duration: 8–20 minutes per session
- Frequency: 3 sessions per week during the acute treatment phase (4–8 weeks)
- Target sites: F3 and F4 (DLPFC), Fz (medial prefrontal), occasionally Pz (posterior default mode network)
- Maintenance: 1–2 sessions per week after initial response
Device Selection
The device quality gap in this space is enormous. Research-grade devices (Photomedex, Vielight Neuro systems, TerraQuant cranial probes) deliver verified, consistent parameters. Consumer devices vary wildly in their claimed vs. actual output. I do not recommend patients self-treat with devices that cannot verify irradiance.
Integration with Conventional and Integrative Psychiatry
I use tPBM as a component of a broader treatment architecture, not as a stand-alone intervention. The combination strategies I find most effective are:
With pharmacotherapy: tPBM appears additive rather than interactive — it does not alter drug metabolism or receptor pharmacology in documented ways. Patients on SSRIs, SNRIs, or bupropion can typically continue without adjustment. The combination may accelerate response onset compared to medication alone.
With neurofeedback: Both modalities target prefrontal regulation. I typically sequence tPBM first (stimulatory/restorative phase) followed by neurofeedback training in the same session, allowing patients to practice self-regulation in an enhanced neurobiological state.
With NAD+ IV therapy: In patients with mitochondrial dysfunction as a significant contributor — particularly post-COVID and Lyme-associated depression — combining tPBM with NAD+ infusions creates parallel support for mitochondrial recovery. Clinical response in this combination appears more robust than either alone.
With vagus nerve stimulation: VNS (particularly non-invasive auricular or transcutaneous approaches) engages ascending anti-inflammatory and mood-relevant circuits that complement tPBM’s top-down prefrontal approach. The combination is particularly relevant for inflammatory depression phenotypes.
Lifestyle scaffolding: Any neuromodulation intervention works better on a brain that is sleeping adequately, exercising regularly, and not burdened by ongoing metabolic or inflammatory stress. I do not offer tPBM as a shortcut around these foundations.
What Patients Experience
Setting expectations accurately is part of the intervention. Most patients do not feel anything during treatment — the near-infrared light is invisible and generates minimal warmth. Some report a mild sense of mental clarity or subtle mood lift immediately post-session; others notice nothing acutely.
The therapeutic trajectory more closely resembles antidepressant treatment than ECT or ketamine — effects accumulate over 2–4 weeks rather than appearing dramatically after a single session. I ask patients to track symptoms weekly using a validated scale (PHQ-9, MADRS) and to monitor sleep quality, energy, and cognitive function as early signal variables.
By week 4 of a standard protocol, approximately 50–60% of appropriate candidates show meaningful improvement (≥50% symptom reduction). Non-responders at 8 weeks are unlikely to benefit from continued standard-protocol tPBM alone; I reassess the diagnostic formulation and consider intensification strategies.
Related Articles
- Photobiomodulation for Brain Fog: Mechanisms and Clinical Application
- TMS for Depression: A Physician’s Evidence Review
- Vagus Nerve Stimulation and Chronic Inflammation
- Post-COVID Brain Fog: What’s Actually Happening Neurologically
- NAD+ IV Therapy: What to Expect
References
-
Cassano P, Petrie SR, Hamblin MR, Henderson TA, Iosifescu DV. Review of transcranial photobiomodulation for major depressive disorder: targeting brain metabolism, inflammation, oxidative stress, and neuroplasticity. Neurophotonics. 2016;3(3):031404. PMID 27500188
-
Cassano P, Caldieraro MA, Norton R, et al. Reported side effects, weight and blood pressure, after repeated sessions of transcranial photobiomodulation. Photobiomodul Photomed Laser Surg. 2019;37(10):651-656. PMID 31557081
-
Naeser MA, Zafonte R, Krengel MH, et al. Significant improvements in cognitive performance post-transcranial, red/near-infrared light-emitting diode treatments in chronic, mild traumatic brain injury. J Neurotrauma. 2014;31(11):1008-1017. PMID 24568233
-
Hamblin MR. Mechanisms and applications of the anti-inflammatory effects of photobiomodulation. AIMS Biophys. 2017;4(3):337-361. PMID 28748217
-
Salehpour F, Mahmoudi J, Kamari F, Sadigh-Eteghad S, Rasta SH, Hamblin MR. Brain photobiomodulation therapy: a narrative review. Mol Neurobiol. 2018;55(8):6601-6636. PMID 29327206
-
Caldieraro MA, Cassano P. Transcranial and systemic photobiomodulation for major depressive disorder: a systematic review of efficacy, tolerability and biological mechanisms. J Affect Disord. 2019;243:262-273. PMID 30248630
-
Chao LL. Effects of home photobiomodulation treatments on cognitive and behavioral function, cerebral perfusion, and resting-state functional connectivity in patients with dementia: a pilot trial. Photobiomodul Photomed Laser Surg. 2019;37(3):133-141. PMID 31050942