At a Glance
| Property | Value |
|---|---|
| Evidence Level | Emerging to Moderate (consistent mechanism, growing human data) |
| Primary Use | Cognitive dysfunction from mitochondrial impairment in chronic illness |
| Key Mechanism | Near-infrared light restores cytochrome c oxidase function, rescuing ATP production in neurons |
The Brain Fog-Mitochondria Connection
If you are reading this article, you probably already know what brain fog feels like. Slow processing speed. Words that disappear mid-sentence. The feeling of thinking through wet cement. What you may not know is that this subjective experience has a concrete biological basis — and that basis, in most chronic illness patients, traces back to the mitochondria.
Here is what the evidence shows: neurons are among the most metabolically demanding cells in the body. The brain represents approximately 2% of body weight but consumes 20% of total oxygen and glucose. When mitochondrial function declines — whether from infection-driven inflammation, oxidative stress, toxin exposure, or immune dysregulation — the brain is among the first organs to show functional impairment [1].
This is not abstract theory. PET scan studies in post-treatment Lyme disease patients show measurable reductions in cerebral metabolic rate. fMRI studies in post-COVID patients demonstrate altered functional connectivity patterns consistent with reduced neuronal energy availability. Organic acid testing in brain fog patients consistently shows elevated markers of mitochondrial dysfunction — elevated lactate-to-pyruvate ratios, reduced citric acid cycle intermediates, and abnormal fatty acid oxidation markers.
The question is not whether mitochondrial dysfunction drives brain fog. The question is what to do about it.
Why Photobiomodulation Makes Mechanistic Sense
Most treatments for mitochondrial dysfunction work indirectly. CoQ10 provides a cofactor. NAD+ precursors supply substrate. B vitamins support enzyme function. These are all valuable, but they all depend on the electron transport chain itself being functional enough to utilize them.
Photobiomodulation works differently. It acts directly on the rate-limiting step.
Cytochrome c oxidase (Complex IV) is the final enzyme in the mitochondrial electron transport chain. It transfers electrons to oxygen, generating the proton gradient that drives ATP synthase. In states of chronic inflammation, nitric oxide accumulates and competitively inhibits CCO by binding to the oxygen-binding site. This is one of the primary mechanisms by which neuroinflammation suppresses energy production [2].
Near-infrared light at 810nm is absorbed directly by cytochrome c oxidase. The photon energy dissociates nitric oxide from the enzyme’s binuclear center, immediately restoring catalytic activity. This is a direct, photochemical intervention at the exact point where the electron transport chain is bottlenecked.
In my clinical experience, this is what makes PBM qualitatively different from other mitochondrial support strategies. It does not supply a cofactor that the dysfunctional machinery cannot use. It removes the brake that is preventing the machinery from running.
The Evidence
What We Know (Human Data)
Cognitive performance in healthy adults: Blanco et al. (2017) demonstrated that a single session of transcranial PBM at 1064nm significantly improved working memory capacity and sustained attention in healthy young adults, as measured by the delayed match-to-sample task. Prefrontal oxygenation, measured by functional near-infrared spectroscopy, increased during the PBM session, suggesting enhanced mitochondrial oxygen metabolism [3].
Traumatic brain injury and cognitive fog: Naeser et al. (2014, 2019) published multiple studies showing that transcranial LED treatment at 810nm and 633nm improved cognitive function — specifically executive function, verbal memory, and processing speed — in patients with chronic TBI-related cognitive dysfunction. These are patients who had failed conventional rehabilitation.
Dementia: Chao (2019) reported that home-based transcranial PBM over 12 weeks improved executive function, clock drawing, and immediate recall in patients with mild-to-moderate dementia, compared to sham. These improvements correlated with increased cerebral perfusion on SPECT imaging — direct evidence that PBM was improving brain blood flow and metabolism.
Post-COVID brain fog: While large RCTs are still underway, preliminary data and case series from multiple centers suggest that transcranial PBM improves subjective cognitive function and objective neuropsychological test scores in long COVID patients with persistent brain fog. The biological plausibility is strong: SARS-CoV-2 is known to cause mitochondrial dysfunction through multiple mechanisms including spike protein-mediated Complex I inhibition.
What We See in the Lab (Preclinical)
Animal studies have provided the mechanistic foundation:
- Transcranial PBM reduces neuroinflammatory markers (TNF-alpha, IL-1beta, IL-6) in models of neurodegeneration
- PBM increases hippocampal BDNF expression, supporting neuroplasticity
- In ischemia-reperfusion models, PBM preserves mitochondrial membrane potential and reduces apoptosis
- PBM at 810nm increases brain ATP content by 30-70% in animal models, measured directly by phosphorus-31 magnetic resonance spectroscopy
What I See in Practice
In our clinical experience treating patients with chronic brain fog from Lyme disease, post-COVID syndrome, and mold illness, I observe that transcranial PBM produces measurable cognitive improvements in approximately 60-70% of patients when used as part of a comprehensive neuromodulation protocol.

The typical response pattern is:
- Weeks 1-2: Subtle improvements in verbal fluency and processing speed. Some patients report “clearer” thinking but cannot articulate exactly what changed.
- Weeks 3-4: More noticeable improvements. Patients report being able to read for longer periods, follow conversations more easily, and retrieve words more reliably.
- Weeks 5-8: Consolidated gains. Some patients describe this as “lifting of a veil” that had been present for months or years.
The patients who respond best share common characteristics: mitochondrial dysfunction markers on organic acid testing, brain fog as the dominant symptom (rather than pain), and adequate treatment of underlying infections before starting PBM. This last point is critical — PBM will not overcome ongoing active neuroinflammation from untreated Borrelia or persistent SARS-CoV-2 spike protein. Address the driver first, then optimize mitochondrial recovery.
What I tell my patients: PBM is a mitochondrial rescue tool. It works best when the acute assault on the mitochondria has been controlled and you are now supporting recovery of damaged but salvageable neurons. Beyond cognitive recovery, the same mitochondrial and neuroinflammatory mechanisms that clear brain fog appear to operate in mood circuitry — our companion review on photobiomodulation for depression covers the RCT data and protocol specifics for that application.
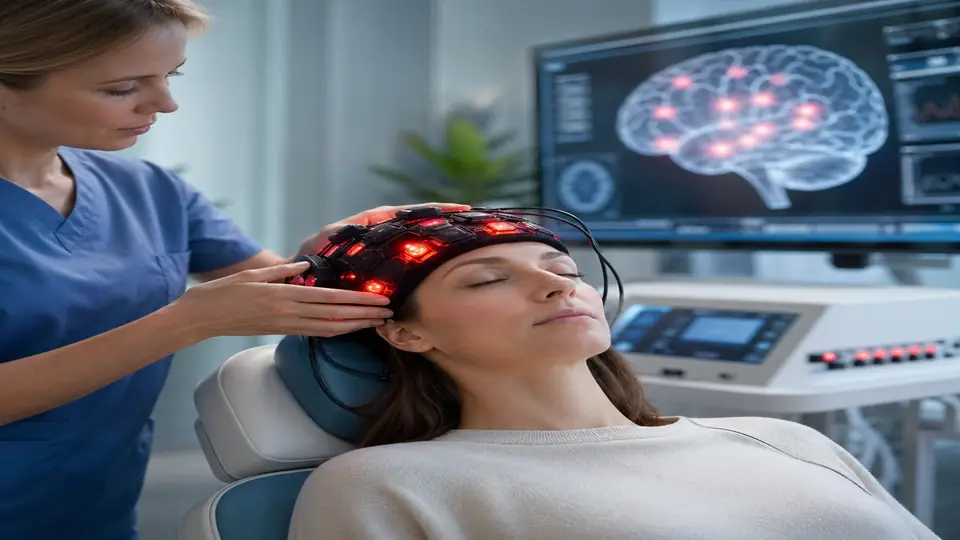
Practical Application
Protocol for Brain Fog
Based on the published literature and my clinical observation:
- Wavelength: 810nm near-infrared (this is critical — consumer red light panels at 660nm are insufficient for transcranial application)
- Target sites: Bilateral frontal (F3, F4), temporal (T3, T4), and midline parietal (Pz) — these target the default mode network and prefrontal cortex
- Power density: 50-250 mW/cm2 at the scalp
- Energy dose: 20-60 J/cm2 per site
- Session duration: 20-30 minutes total
- Frequency: 3 sessions per week for 8-12 weeks initially
- Pulsing: 40 Hz pulsed mode is increasingly preferred for cognitive applications, based on gamma entrainment data
Combining PBM with Other Approaches
PBM for brain fog works best in combination:
- Address the root cause: Treat the infection, remove the toxin, calm the immune dysregulation
- Support mitochondrial substrates: CoQ10 (200-400mg ubiquinol), NAD+ precursors, B vitamins, magnesium
- Reduce ongoing neuroinflammation: Omega-3 fatty acids (2-4g EPA+DHA), curcumin, specialized pro-resolving mediators
- Add PBM to directly restore electron transport chain function
- Consider complementary neuromodulation: Neurofeedback for brainwave pattern normalization, vagus nerve stimulation for autonomic rebalancing

When to Consider Formal Cognitive Testing
If brain fog has persisted for more than 6 months despite treatment, I recommend neuropsychological testing to establish a formal cognitive baseline. This provides objective data for tracking treatment response and can identify specific cognitive domains that need targeted rehabilitation.
Safety and Considerations
Transcranial PBM for brain fog is well-tolerated. The most common side effect is transient headache in the first 1-3 sessions, which typically resolves as treatment continues. Rare reports of temporary sleep disruption exist, likely related to the energizing effect of improved mitochondrial function — similar to how some patients feel energized after an NAD+ infusion.
The important caveat: PBM is not a substitute for diagnosing and treating the underlying cause of brain fog. If your cognitive dysfunction is driven by active neuroborreliosis, untreated mold exposure, or autoimmune encephalitis, PBM alone will provide temporary and incomplete relief at best. The foundation of treatment must address the driver.
The Bottom Line
Brain fog in chronic illness is not “just fatigue” and it is not psychosomatic. It reflects measurable mitochondrial dysfunction in neurons. Photobiomodulation at near-infrared wavelengths directly addresses this dysfunction by restoring cytochrome c oxidase activity — the molecular bottleneck in energy production. The evidence is growing, the safety profile is excellent, and the mechanism is well-characterized. For patients with persistent cognitive dysfunction after controlling the underlying disease, transcranial PBM represents a rational, evidence-informed addition to the recovery plan.
References
- Myhill S, Booth NE, McLaren-Howard J. Chronic fatigue syndrome and mitochondrial dysfunction. International Journal of Clinical and Experimental Medicine. 2009;2(1):1-16. PMC2680051.
- Hamblin MR. Mechanisms and applications of the anti-inflammatory effects of photobiomodulation. AIMS Biophysics. 2017;4(3):337-361. PMC5523874.
- Blanco NJ, Maddox WT, Gonzalez-Lima F. Improving executive function using transcranial infrared laser stimulation. Journal of Neuropsychology. 2017;11(1):14-25. PMID: 26017772.
- Chao LL. Effects of Home Photobiomodulation Treatments on Cognitive and Behavioral Function, Cerebral Perfusion, and Resting-State Functional Connectivity in Patients with Dementia. Photobiomodulation, Photomedicine, and Laser Surgery. 2019;37(3):133-141. PMID: 31050928.