At a Glance
| Property | Value |
|---|---|
| Condition | Post-COVID Brain Fog |
| Evidence Level | Moderate (clinical studies available) |
| Causative Agent | SARS-CoV-2 |
| Treatment Approach | Low-dose naltrexone (LDN): 1-4.5 mg at bedtime, Omega-3 fatty acids: High-dose EPA/DHA (3-4 g…, Curcumin: Bioavailable formulations for… |
| Key Takeaway | Post-COVID brain fog involves measurable cognitive impairment driven by neuroinflammation, microclot-impaired cerebral microcirculation, autoantibodies… |
Of all the symptoms that post-COVID patients report, cognitive dysfunction — commonly called “brain fog” — may be the most distressing. Patients describe difficulty concentrating, impaired short-term memory, slowed processing speed, word-finding difficulties, and a pervasive sense that their mental clarity has been replaced by a cognitive haze.
For many of these patients, standard neurological workups are normal. MRI is unremarkable. Routine cognitive testing may be within normal limits — though often in the lower range of where the patient would have scored previously. The result is a familiar and frustrating pattern: real cognitive impairment without a diagnosis that conventional neurology readily accepts.
The cognitive dysfunction is real, it is measurable with appropriate tools, and it has identifiable mechanisms.
The Mechanisms
Post-COVID brain fog is not a single pathology. Multiple mechanisms contribute, and their relative importance varies between patients:

Neuroinflammation
SARS-CoV-2 infection triggers neuroinflammation through several pathways:
- Direct viral entry: While the extent of direct neuronal infection is debated, the virus can enter the central nervous system via the olfactory nerve, the blood-brain barrier, or through immune cell trafficking [1].
- Cytokine-mediated inflammation: Systemic inflammatory cytokines (IL-6, TNF-alpha, IL-1beta) cross the blood-brain barrier and activate microglia — the brain’s resident immune cells. Activated microglia produce their own inflammatory mediators, creating a self-sustaining neuroinflammatory cycle.
- Blood-brain barrier disruption: COVID-19 can increase blood-brain barrier permeability, allowing inflammatory molecules, immune cells, and potentially viral components to enter the brain parenchyma.
Neuroimaging studies in post-COVID patients have identified microglial activation using PET tracers, supporting the neuroinflammatory hypothesis [2].
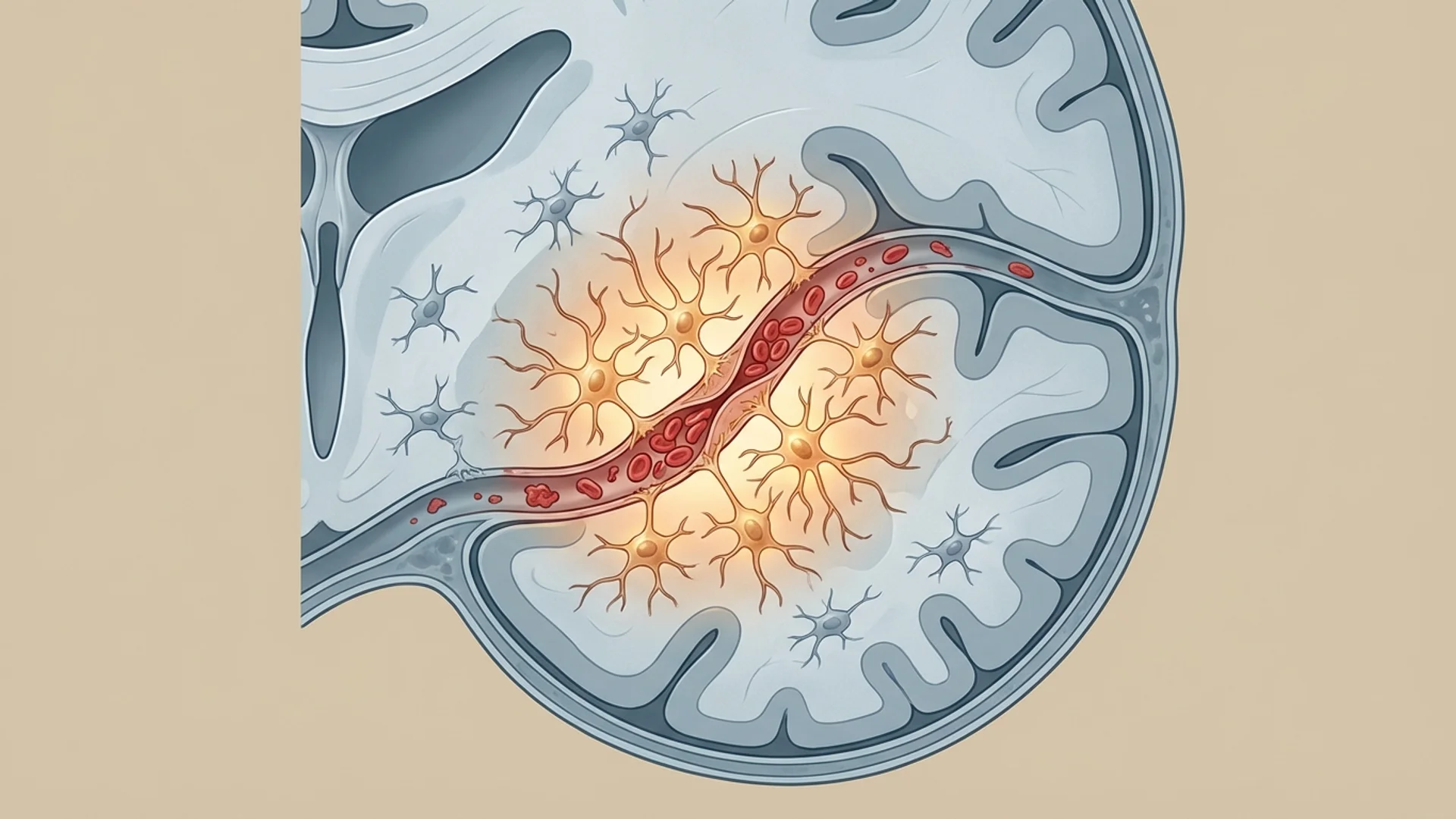
Microcirculatory Impairment
As I discussed in my microclot article, fibrin amyloid microclots and endothelial dysfunction can impair capillary blood flow throughout the body. The brain, which consumes approximately 20% of the body’s oxygen despite representing only 2% of body mass, is particularly vulnerable to even modest reductions in microcirculatory perfusion.
Cerebral microclots can produce the kind of diffuse, fluctuating cognitive impairment that characterizes brain fog — not a focal neurological deficit (like a stroke would cause) but a generalized reduction in cognitive efficiency.
Autoimmunity
Post-COVID autoantibodies targeting neural tissue have been identified in some patients. These include antibodies against:
- Neuronal surface antigens
- Autonomic ganglia (contributing to dysautonomia)
- Various intracellular neural proteins
Whether these autoantibodies are directly causing cognitive dysfunction or are markers of a broader autoimmune process is an active area of investigation.
Reactivated Viruses
EBV, CMV, and HHV-6 — viruses with known neurotropism — frequently reactivate following COVID-19. HHV-6 in particular can infect glial cells and neurons, and its reactivation has been associated with cognitive dysfunction independently of COVID-19.
Mitochondrial and Metabolic Dysfunction
The brain’s enormous energy demands make it vulnerable to mitochondrial dysfunction and cellular energy. Post-COVID metabolic changes — including reduced NAD+ levels, impaired oxidative phosphorylation, and altered glucose metabolism — can produce cognitive symptoms even in the absence of structural brain damage.
Assessment
When I evaluate a post-COVID patient with cognitive complaints, my assessment goes beyond standard neurological examination:
- Neurocognitive testing: Formal assessment of attention, processing speed, working memory, executive function, and verbal fluency. Even “normal range” scores may represent significant decline from the patient’s baseline.
- Inflammatory markers: hsCRP, IL-6, and — where available — markers of neuroinflammation
- Coagulation assessment: D-dimer, fibrinogen, von Willebrand factor
- Reactivated virus panel: EBV, CMV, HHV-6 serology including reactivation markers
- Autoantibody screening: Antineuronal antibodies where clinically indicated
- Mitochondrial markers: Organic acid testing, lactate/pyruvate ratios
- Autonomic assessment: POTS and other dysautonomia can present primarily as cognitive symptoms due to reduced cerebral perfusion in upright posture
- Brain MRI: To exclude structural pathology, though findings are usually normal or show only nonspecific changes
Treatment Approach
Treatment targets the identified mechanisms:
Anti-Neuroinflammatory Strategies
- Low-dose naltrexone (LDN): 1-4.5 mg at bedtime. LDN modulates microglial activation and has shown preliminary benefit in post-COVID neuroinflammation; its dual mechanism — transient opioid receptor blockade plus TLR4 inhibition — makes it particularly relevant for the neuroinflammatory component of brain fog (see LDN: clinical evidence and dosing protocol). The evidence is from case series and small studies, not large RCTs, but the safety profile is favorable.
- Omega-3 fatty acids: High-dose EPA/DHA (3-4 g daily) for anti-inflammatory effects, including neuroinflammatory modulation
- Curcumin: Bioavailable formulations for systemic and neuroinflammatory support
Microcirculatory Support
- Anticoagulation and apheresis as described in my microclot article
- Ginkgo biloba (standardized extract, 120-240 mg daily) for cerebral microcirculatory support — modest evidence from controlled trials in cognitive impairment of other etiologies
Mitochondrial Support
- IV NAD+ and oral NMN for NAD+ repletion
- CoQ10 for electron transport chain support
- IHHT for mitochondrial biogenesis
- B vitamins, magnesium, alpha-lipoic acid
Addressing Reactivated Viruses
- Antiviral therapy when reactivation is confirmed (valacyclovir, valganciclovir depending on the virus)
- Immune support to restore viral control
Neurocognitive Rehabilitation
- Graduated cognitive challenge — just as physical rehabilitation requires graded exercise, cognitive rehabilitation requires graded mental activity
- Sleep optimization — the brain’s waste clearance system (glymphatic system) operates during deep sleep, and impaired sleep directly worsens cognitive function
- Stress reduction — chronic stress hormones impair hippocampal function and exacerbate neuroinflammation
Clinical Observations
The trajectory of recovery for post-COVID brain fog varies considerably. Some patients improve substantially within weeks of targeted treatment. Others require months of sustained intervention. A minority have slow or incomplete recovery.
In my experience, the patients who recover most completely are those in whom a specific, treatable mechanism is identified and addressed — reactivated EBV, significant microclot burden, severe mitochondrial dysfunction. Patients with multiple contributing mechanisms require more comprehensive and prolonged treatment.
What I tell patients: brain fog is not permanent. The brain has remarkable capacity for recovery when the underlying drivers are identified and addressed. But recovery is usually gradual, and patience is required.

References
- Fernandez-Castaneda A, et al. Mild respiratory COVID can cause multi-lineage neural cell and myelin dysregulation. Cell. 2022;185(14):2452-2468.
- Visser D, et al. Long COVID treatment is associated with extensive in-vivo neuroinflammation on [18F]DPA-714 PET. Brain. 2022;145(11):4067-4078.
This content is educational and does not constitute medical advice. Post-COVID cognitive dysfunction should be evaluated and treated by a qualified physician.