Topic
Neuromodulation
Transcranial magnetic stimulation, vagus nerve stimulation, neurofeedback, and brain-targeted therapies. What the evidence shows and what I see in practice.
Explore by Topic
Transcranial Magnetic Stimulation (TMS)
FDA-cleared non-invasive brain stimulation for depression, OCD, and emerging indications.
Vagus Nerve Stimulation
Parasympathetic activation through invasive and non-invasive VNS approaches.
Neurofeedback
Real-time EEG training for self-regulation of brain activity patterns.
PEMF Therapy
Pulsed electromagnetic field therapy for pain, inflammation, and tissue repair.
Photobiomodulation
Low-level light therapy for brain health, mood, and cognitive performance.
Brain Fog Treatment
Neuromodulation approaches for cognitive dysfunction in chronic illness.
Free Guide
Brain Health and Neuromodulation Guide
Download the complete physician's guide. Evidence-based, no hype.
All Articles
25 articles
Chronic Fatigue Syndrome: A Physician's Complete Guide
A physician's complete guide to chronic fatigue syndrome. Mitochondrial dysfunction, immune dysregulation, diagnostic criteria, and the stepwise treatment approach we use at Klinik St. Georg.
Neuroborreliosis: When Lyme Crosses the Blood-Brain Barrier
How Borrelia invades the central nervous system, why neuroborreliosis is underdiagnosed, and how hyperthermia, TPS, and multimodal protocols treat what antibiotics alone cannot reach.

Brain Fog Treatment: A Physician's Complete Guide
Brain fog treatment options from neuroinflammation workup to neuromodulation. Causes include post-COVID, Lyme, MCAS, and mold. TPS, NAD+, and hyperbaric oxygen covered.
Clearing Brain Fog After Treatment: Recovery Timeline
What to expect during brain fog recovery after Lyme treatment — the multi-system recovery approach, realistic timelines, and evidence-based strategies.
Brain Fog and Neuroinflammation: The PET Scan Evidence
What causes brain fog in Lyme disease — Johns Hopkins PET scan findings showing glial activation, neuroinflammation mechanisms, and treatment implications.
Neurofeedback for ADHD: Does It Work?
Neurofeedback for ADHD reviewed honestly. EEG mechanism, theta/beta ratio, clinical trial evidence, limitations, session requirements, and realistic expectations from a physician.
Neurofeedback for Lyme Brain Fog
How neurofeedback retrains dysregulated brainwave patterns in Lyme disease patients. qEEG findings, clinical evidence, and what to expect from treatment.
Neurofeedback vs Biofeedback: Which Do You Need?
Clear comparison of neurofeedback and biofeedback. What each measures, how they work, conditions they treat, and how to choose the right one for your situation.

Neuropsychological Testing for Brain Fog: When and Why
When to get neuropsychological testing for brain fog. What the evaluation measures, how it differs from standard neurology exams, and what the results mean for treatment.
Photobiomodulation for Brain Fog: Mitochondrial Rescue
How photobiomodulation targets mitochondrial dysfunction to clear brain fog. Mechanism, clinical evidence, and practical application for chronic illness patients.
Transcranial Photobiomodulation: Light Through the Skull
Evidence-based review of transcranial photobiomodulation for brain health. Wavelengths, mechanisms, clinical trial data, and what I see in practice.
PBM vs Red Light Therapy: What's the Difference?
Photobiomodulation vs red light therapy explained. Terminology, wavelengths, clinical vs consumer devices, and why the distinction matters for brain health.
PEMF Therapy: Pulsed Electromagnetic Fields for Pain and Healing
Evidence-based review of PEMF therapy. Mechanisms, clinical evidence for pain, bone healing, inflammation, and tissue repair. What the research shows and what we observe in practice.

PEMF for Lyme Disease and Chronic Pain
How pulsed electromagnetic field therapy supports pain relief and inflammation reduction in Lyme disease — mechanism, clinical evidence, and practical considerations.

PEMF Therapy Side Effects: What to Expect
What to expect during and after PEMF therapy — common responses, contraindications, how to titrate sessions, and when temporary symptom increases are normal.

PEMF vs TENS vs Red Light: Comparing Energy Therapies
Head-to-head comparison of PEMF, TENS, and red light therapy. Mechanisms, evidence, best use cases, and how to choose the right energy therapy for your condition.

Photobiomodulation: Red and Near-Infrared Light for the Brain
Evidence-based review of transcranial photobiomodulation. How red and near-infrared light affects brain metabolism, the evidence for TBI, dementia, depression, and cognitive enhancement.
qEEG Brain Mapping: What It Shows and Who Needs It
Complete guide to quantitative EEG brain mapping. What the test measures, how it identifies brain dysregulation, and why it matters for neurofeedback and brain fog treatment.

TMS for Depression: What 20 Years of Evidence Shows
TMS depression treatment reviewed by a physician. FDA clearance history, rTMS protocols, theta burst stimulation, response rates, and who responds best.
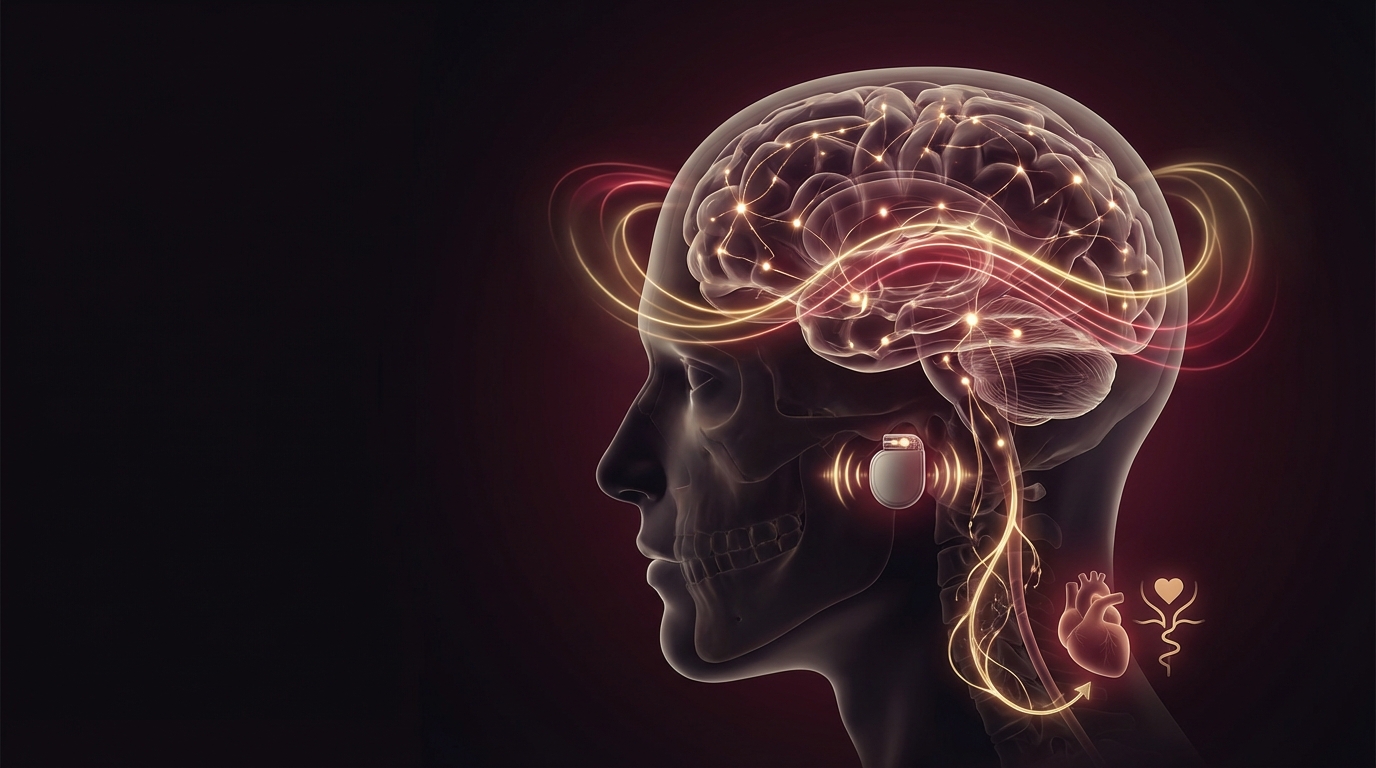
Vagus Nerve Stimulation for Chronic Fatigue and POTS
How vagus nerve stimulation restores autonomic balance in chronic fatigue and POTS — the cholinergic anti-inflammatory pathway, clinical evidence, and treatment options.
At-Home Vagus Nerve Exercises: Evidence-Based Techniques
Evidence-based vagus nerve exercises you can do at home — diaphragmatic breathing, cold exposure, humming, and why starting slow matters for dysautonomia patients.
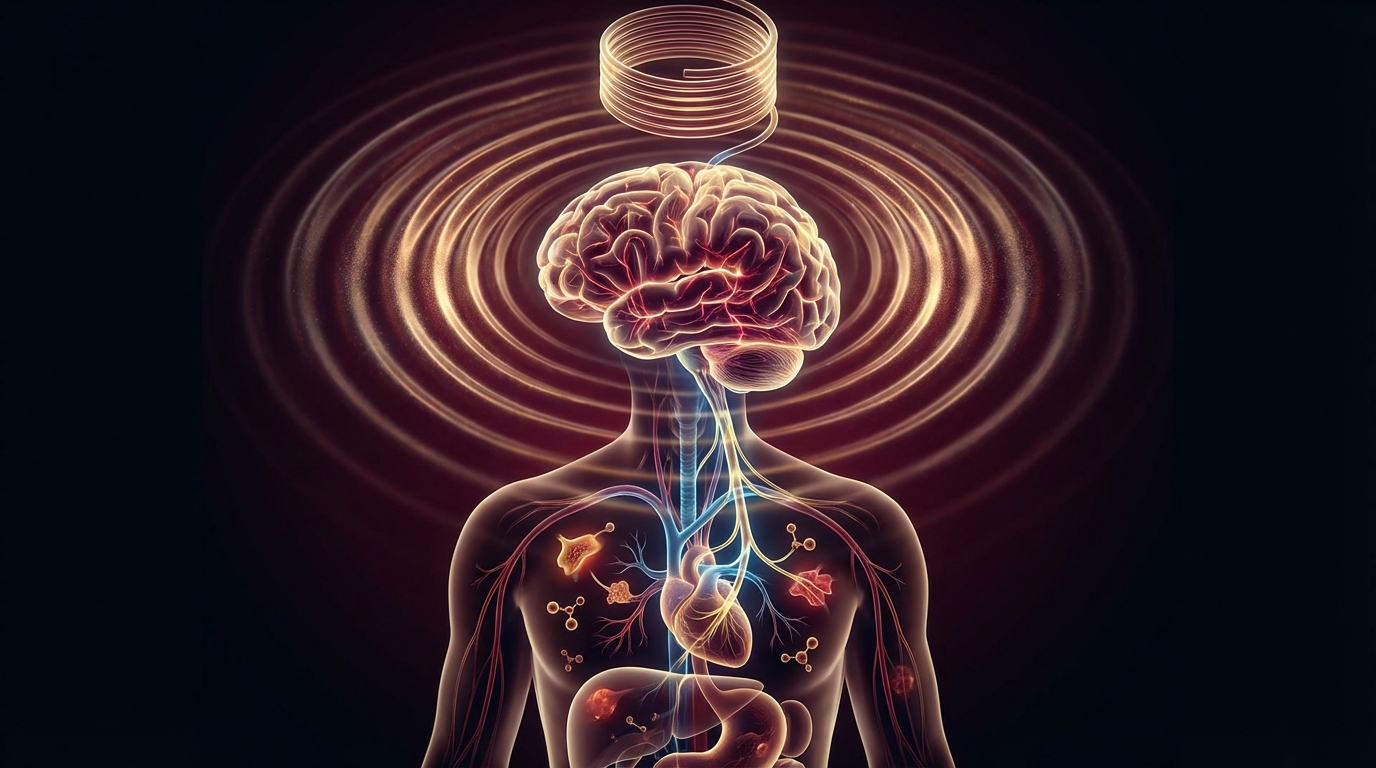
The Vagus Nerve and Inflammation: Cholinergic Anti-Inflammatory Pathway
How the vagus nerve controls inflammation through the cholinergic anti-inflammatory pathway. Mechanism, clinical significance, and implications for chronic illness.
Dihexa Dosage: Nootropic Protocol and Safety
Dihexa dosing guide by Dr. Julian Douwes. Oral and subcutaneous protocols, the c-Met safety question, and why caution is warranted with this potent nootropic peptide.
Post-COVID Brain Fog: Mechanisms and Treatment
Why COVID-19 causes persistent cognitive dysfunction and what can be done about it. Mechanisms, assessment, and treatment strategies.
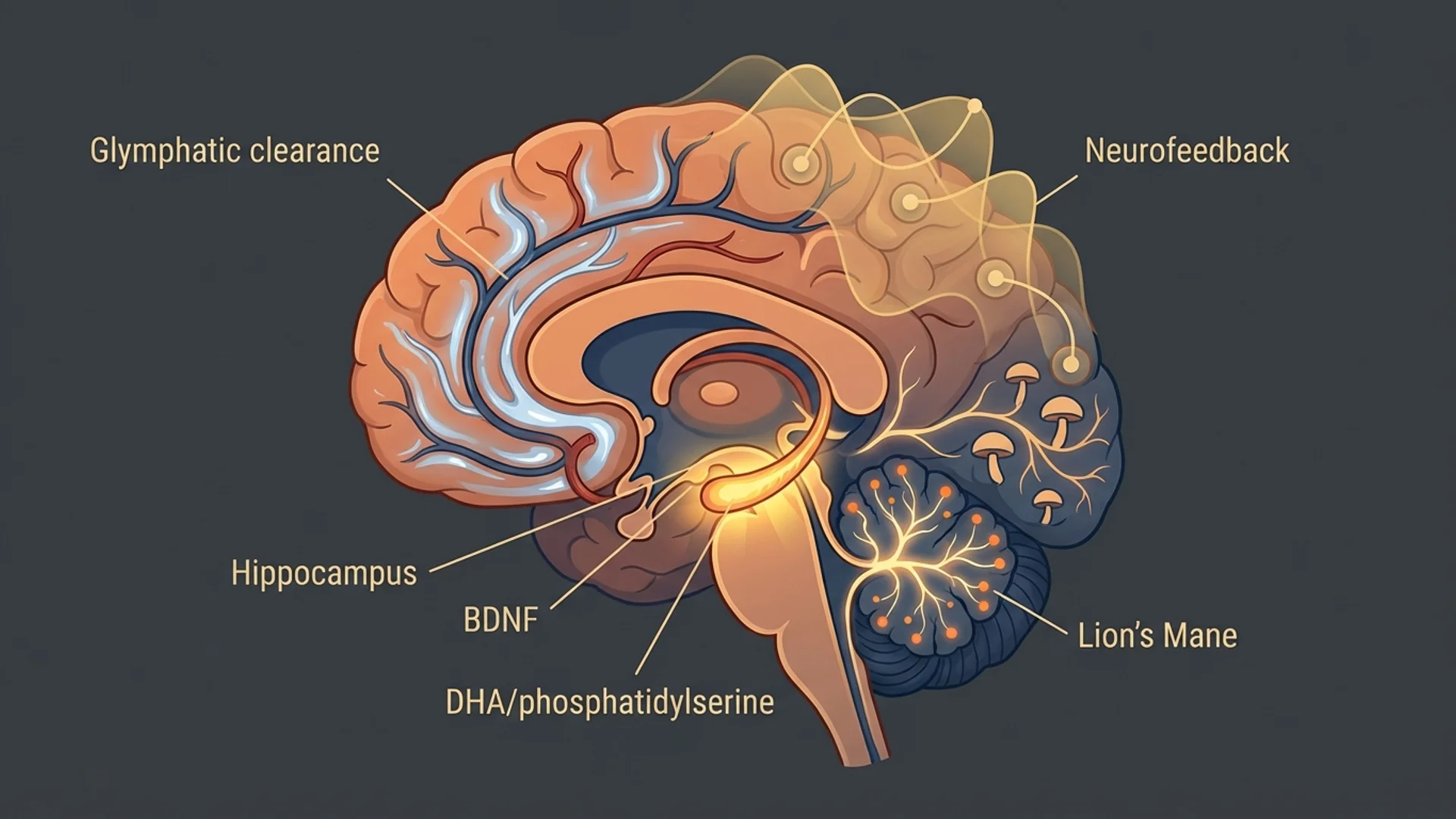
Cognitive Performance Protocol
Evidence-based protocol for mental clarity, focus, and memory from a physician who treats cognitive dysfunction daily.
Complete Guide
The Physician's Guide to Neuromodulation
In-depth reference by Dr. Julian Douwes
What Is Neuromodulation?
Neuromodulation uses electrical, magnetic, acoustic, or light energy to alter brain and nerve function. Unlike medication — which changes chemistry globally — neuromodulation targets specific circuits with precision. Unlike surgery — which is irreversible — most neuromodulation is non-invasive and adjustable.
At St. George Hospital, we integrate neuromodulation into treatment programs for chronic pain, post-COVID brain fog, Lyme neuroborreliosis, depression, and cognitive decline. It complements our existing therapies — hyperthermia, apheresis, peptides, IV protocols — rather than replacing them.
The Therapies
Transcranial Magnetic Stimulation (TMS)
A coil placed against the scalp generates magnetic pulses that induce electrical currents in targeted brain regions. Repetitive TMS (rTMS) is FDA-cleared for treatment-resistant depression, OCD, and smoking cessation. The Stanford SAINT protocol achieved 79% remission in treatment-resistant depression — a remarkable result.
Evidence level: Strong. Multiple large RCTs and meta-analyses.
Conditions: Depression, OCD, chronic pain, migraine, PTSD, post-COVID cognitive symptoms.
Transcranial Direct Current Stimulation (tDCS)
Low-intensity direct current (1-2 mA) through scalp electrodes modulates cortical excitability. Anodal stimulation increases activity; cathodal decreases it. The Flow FL-100 became the first FDA-approved home tDCS device for depression in late 2025.
Evidence level: Moderate-strong. Hundreds of RCTs. Best evidence for depression and cognitive enhancement in aging.
Conditions: Depression, chronic pain, cognitive decline, post-stroke rehabilitation.
Vagus Nerve Stimulation (VNS)
The vagus nerve connects to the brainstem, limbic system, and cortex. Stimulating it activates the cholinergic anti-inflammatory pathway — reducing TNF-alpha, IL-1beta, and IL-6. Non-invasive transcutaneous auricular VNS (taVNS) stimulates the vagus through the ear, requiring no surgery.
Evidence level: Strong for epilepsy and depression (invasive). Moderate-emerging for taVNS across multiple conditions.
Conditions: Epilepsy, depression, inflammatory bowel disease, rheumatoid arthritis, chronic pain, PTSD, dysautonomia, post-COVID.
This is where I see enormous potential for Lyme disease. Columbia University is currently recruiting for a VNS trial for post-treatment Lyme disease. The anti-inflammatory mechanism directly addresses persistent neuroinflammation.
Neurofeedback
Real-time EEG monitoring provides feedback to train patients to self-regulate brainwave patterns. Quantitative EEG (qEEG) brain mapping identifies aberrant patterns that guide protocol selection.
Evidence level: Moderate. Over 3,000 peer-reviewed studies. Level 1 evidence for ADHD.
Conditions: ADHD, anxiety, depression, PTSD, insomnia, chronic pain, cognitive decline.
In Lyme patients, abnormal qEEG patterns are found in approximately 75% of active cases. Published case reports show significant cognitive improvement after neurofeedback training.
PEMF (Pulsed Electromagnetic Field Therapy)
Pulsed electromagnetic fields at specific frequencies influence DNA synthesis, gene expression, and mitochondrial function. FDA-cleared for bone healing since 1979.
Evidence level: Mixed. Strong for bone healing and spinal pain. A 2025 meta-analysis found highly fragmented evidence for neuropathic pain.
Conditions: Bone fracture non-union, osteoarthritis, chronic pain (especially spinal/radicular), wound healing.
Transcranial Photobiomodulation
Near-infrared light (810nm or 1064nm) absorbed by cytochrome c oxidase in mitochondria enhances ATP production, reduces neuroinflammation, improves cerebral blood flow, and promotes neurogenesis.
Evidence level: Emerging. Compelling preclinical data. Clinical validation in early phases.
Conditions: Alzheimer’s, Parkinson’s, traumatic brain injury, depression, cognitive enhancement.
Transcranial Pulse Stimulation (TPS)
Focused ultrasound pulses reach deep brain structures non-invasively. A February 2025 RCT published in JAMA Network Open showed significant cognitive improvement in Alzheimer’s patients aged 70 or under. Approved in Europe for clinical treatment of Alzheimer’s disease.
Evidence level: Moderate-strong for Alzheimer’s.
Cranial Electrotherapy Stimulation (CES)
Low-level alternating microcurrent via ear-clip electrodes. FDA-cleared for anxiety, depression, and insomnia. A 2025 real-world study found 48% achieved insomnia remission by day 21.
Evidence level: Moderate. High certainty for anxiety. Large effect size for insomnia.
How We Choose the Right Therapy
Every neuromodulation program begins with assessment:
- qEEG brain mapping — identifies specific brainwave pattern abnormalities
- Autonomic testing — HRV analysis, tilt-table if dysautonomia suspected
- Neurocognitive assessment — baseline cognitive function measurement
- Clinical history — the underlying condition determines which modalities apply
We do not apply neuromodulation blindly. The diagnostic workup determines which circuits need modulation and in which direction.
Integration with Other Therapies
Neuromodulation is most powerful when combined with other treatment modalities:
- Post-COVID: taVNS for autonomic regulation + apheresis for microclot removal + NAD+ IV for mitochondrial support + neurofeedback for cognitive rehabilitation
- Lyme neuroborreliosis: Antimicrobial therapy + neurofeedback for cognitive recovery + taVNS for neuroinflammation + TMS for depression
- Cancer pain: TMS for pain modulation + PEMF for musculoskeletal symptoms + CES for anxiety and sleep
- Longevity: TPS for cognitive preservation + neurofeedback for brain performance + photobiomodulation for neuroprotection
Safety
Non-invasive neuromodulation has an excellent safety profile. Common side effects are mild and transient — scalp discomfort with TMS, mild headache with tDCS, skin irritation with electrode placement.
Contraindications vary by modality but generally include: metal implants near the stimulation site (TMS), active seizure disorder (some modalities), and pregnancy (precautionary).
The Evidence Honest Assessment
I want to be transparent about where the evidence stands:
- Strong: TMS for depression, VNS for epilepsy, CES for anxiety, TPS for Alzheimer’s
- Moderate: tDCS for depression and pain, neurofeedback for ADHD, PEMF for bone healing
- Emerging: VNS for Lyme disease, photobiomodulation for neurodegeneration, tDCS for post-COVID
- Preliminary: Binaural beats for cognitive enhancement, LIFU for mood disorders
We use modalities across this spectrum, but we are always honest with patients about evidence levels. A therapy with emerging evidence may still be worth trying when conventional options have been exhausted — but the patient deserves to know where we stand scientifically.
