The observation that people living at high altitude tend to live longer and have lower rates of cardiovascular disease has intrigued researchers for decades. While altitude exposure involves many variables, the intermittent exposure to lower oxygen levels — hypoxia — appears to be one of the key mechanisms driving adaptation.
IHHT (Intermittent Hypoxia-Hyperoxia Training) takes this principle and applies it in a controlled clinical setting. The patient breathes alternating periods of low-oxygen air (hypoxia, typically 9-13% O2) and high-oxygen air (hyperoxia, 35-40% O2) through a mask while resting comfortably. Each session lasts 30 to 45 minutes.
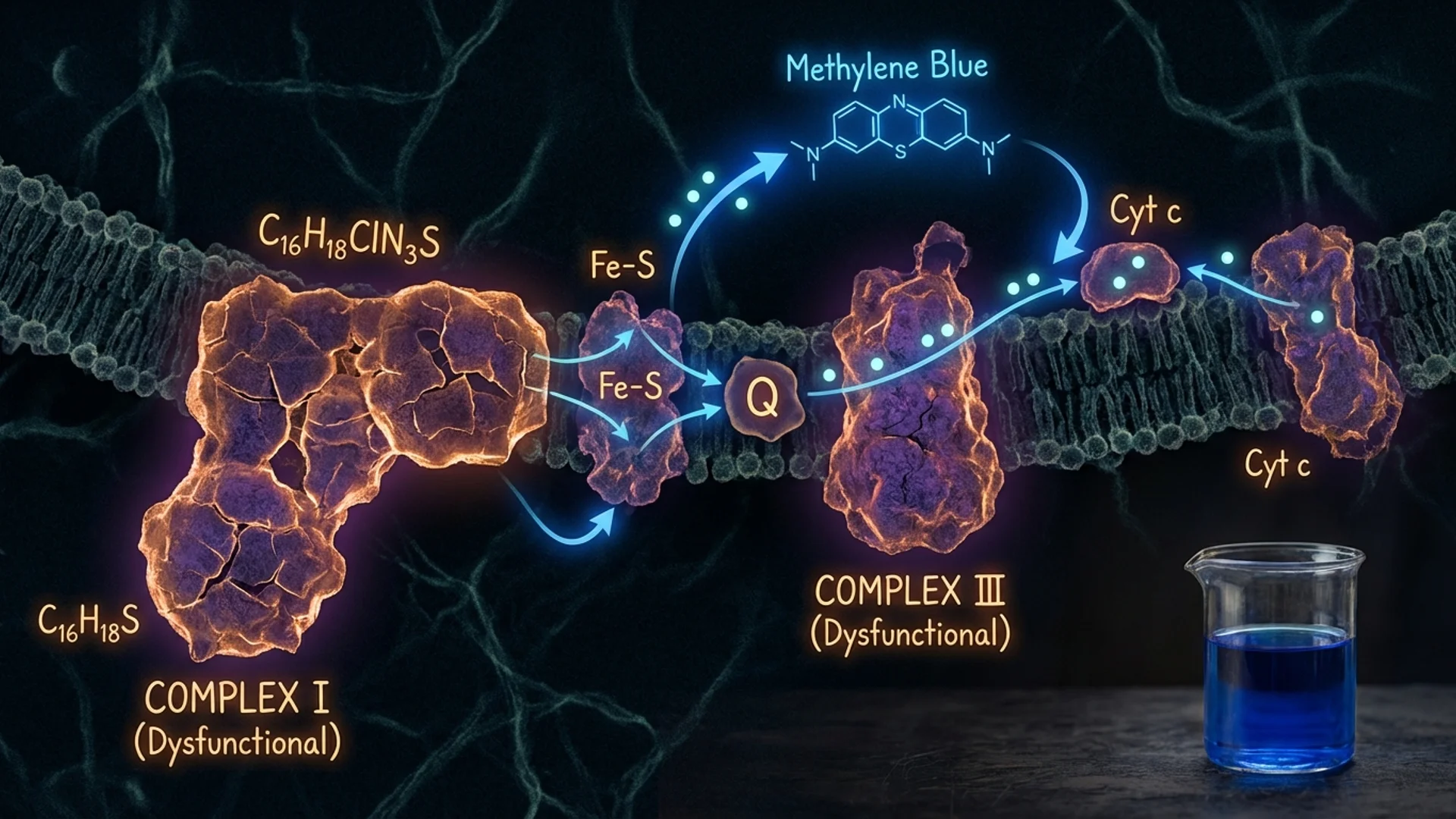
The mechanism of interest is mitochondrial quality control. Hypoxic stress damages weak, dysfunctional mitochondria while triggering the cell to produce new, healthy ones — a process called mitochondrial biogenesis. The hyperoxic intervals provide recovery and enhance oxygen delivery. Over a series of sessions, the net effect is a shift toward a healthier mitochondrial population.
The Evidence
Controlled Human Studies
IHHT has been studied in several controlled human trials, primarily in European clinical settings:

A randomized controlled trial in elderly patients with mild cognitive impairment showed that IHHT improved cognitive function, exercise tolerance, and quality of life scores compared to sham treatment over a 5-week protocol [1].
Studies in patients with metabolic syndrome have demonstrated improvements in blood pressure, lipid profiles, and markers of oxidative stress after IHHT protocols [2].
In patients with chronic fatigue — a population I see frequently in my practice — controlled studies have shown improvements in exercise capacity and subjective energy levels.
Mechanistic Studies
The mechanistic rationale is well-supported. Intermittent hypoxia activates HIF-1alpha (hypoxia-inducible factor), which triggers a cascade of adaptive responses including:
- Upregulation of mitochondrial biogenesis via PGC-1alpha
- Enhanced antioxidant enzyme production
- Improved cellular oxygen utilization efficiency
- Activation of stem cell mobilization pathways
These are the same pathways activated by high-altitude acclimatization, compressed into a clinical protocol.
Important Distinction
I want to be clear about an important distinction. IHHT uses brief, controlled, intermittent hypoxia with recovery intervals. This is fundamentally different from chronic hypoxia (such as untreated sleep apnea), which is harmful. The dose and timing matter enormously. Chronic, uncontrolled hypoxia causes oxidative damage. Brief, intermittent, controlled hypoxia with adequate recovery triggers adaptation.
How I Use IHHT in Practice
IHHT is one of the therapies I use most frequently in my longevity and chronic fatigue programs. The treatment is non-invasive, well-tolerated, and requires no physical exertion from the patient — which makes it accessible even to patients who are too fatigued or deconditioned for exercise-based interventions.
A typical protocol in my practice:
- Initial assessment: Baseline pulse oximetry response to hypoxia (a brief test to determine individual tolerance)
- Protocol: 10-15 sessions over three to five weeks
- Session structure: Alternating periods of hypoxic air (3-5 minutes at 9-13% O2) and hyperoxic air (1-3 minutes at 35-40% O2), repeated six to eight cycles per session
- Monitoring: Continuous pulse oximetry throughout the session; the system automatically adjusts oxygen levels based on the patient’s response
- Progression: Hypoxic intensity is gradually increased across sessions as tolerance improves
Clinical Observations
In my clinical experience, IHHT has been particularly valuable for:
- Chronic fatigue patients who lack the energy for conventional exercise programs
- Post-COVID patients with persistent fatigue and reduced exercise tolerance
- Longevity patients seeking to optimize mitochondrial function as part of a comprehensive program
- Pre-surgical preparation to improve physiological resilience
What I have observed consistently is improved exercise tolerance, better subjective energy levels, and in patients undergoing mitochondrial function testing, measurable improvements in organic acid profiles suggesting enhanced mitochondrial efficiency.
The effects are not instantaneous. Most patients notice meaningful improvement after six to eight sessions. The benefits appear to persist for several weeks to months after completing a course, depending on the patient’s underlying condition and lifestyle factors.
Limitations and Safety
IHHT is generally safe when administered with proper equipment and monitoring. Contraindications include:
- Acute febrile illness
- Severe, uncontrolled hypertension
- Severe COPD with resting hypoxemia
- Acute cardiac events (within the preceding three months)
- Pregnancy
Side effects are uncommon but can include mild headache, lightheadedness, or fatigue immediately after the first few sessions. These typically resolve as the body adapts.
The honest limitation is that while the controlled trial data is positive, much of it comes from relatively small studies, often with surrogate endpoints rather than hard clinical outcomes. Larger, longer-term trials would strengthen the evidence base considerably.
The Bottom Line
IHHT is a well-tolerated, non-invasive intervention with a sound mechanistic rationale and supportive clinical trial data. It is not a replacement for exercise, sleep, and nutrition — the foundations of any longevity program. But as a complementary therapy, particularly for patients with mitochondrial dysfunction or those unable to exercise conventionally, it occupies a useful position in the clinical toolkit.

References
- Serebrovska TV, et al. Intermittent Hypoxia-Hyperoxia Training Improves Cognitive Function and Decreases Circulating Biomarkers of Alzheimer’s Disease in Patients with Mild Cognitive Impairment. International Journal of Molecular Sciences. 2019;20(21):5405.
- Glazachev O, et al. Adaptations following an intermittent hypoxia-hyperoxia training in coronary artery disease patients. Clinical Cardiology. 2017;40(6):370-376.
This content is educational and does not constitute medical advice. IHHT should be administered by trained medical professionals with appropriate monitoring equipment.