At a Glance
| Property | Value |
|---|---|
| Procedure Type | Extracorporeal blood filtration (H.E.L.P. apheresis) |
| Duration | 2-3 hours per session |
| Access | Two peripheral IV lines (antecubital veins) |
| Pain Level | Mild — comparable to standard blood draw |
| Recovery | Most patients resume normal activity same day |
| Common Indications | Elevated inflammatory markers, chronic infection sequelae, environmental toxin burden, cardiovascular risk reduction |
| Evidence Level | Strong for lipid apheresis (cardiovascular); Moderate for H.E.L.P. in inflammatory and environmental applications |
You have been told you need apheresis, or you have researched it and think it might help your condition. Either way, the same question is running through your mind: what is this actually going to be like?
I perform H.E.L.P. apheresis procedures at our hospital regularly. It is one of my three signature treatments — alongside whole-body hyperthermia and IV laser therapy. And the single most common thing patients tell me after their first session is: “That was much less intimidating than I expected.”
This article is the walkthrough I wish every patient had before their first appointment. What happens before, during, and after — step by step, without medical jargon where it is not necessary and without minimizing the parts that patients actually want to know about.
What Is H.E.L.P. Apheresis?
H.E.L.P. stands for Heparin-induced Extracorporeal LDL Precipitation. It is a form of therapeutic apheresis — a category of procedures that filter blood outside the body and return it.
Standard apheresis has been used in medicine for decades, primarily for removing pathological antibodies (plasmapheresis), excess blood cells, or lipoproteins in patients with familial hypercholesterolemia. The evidence for lipid apheresis in cardiovascular disease is strong and well-established.
H.E.L.P. apheresis goes further. The system selectively removes:
- LDL cholesterol and Lp(a) — atherogenic lipoproteins
- Fibrinogen — a coagulation protein that, when elevated, contributes to blood viscosity and cardiovascular risk
- C-reactive protein (CRP) and other inflammatory mediators
- Environmental toxins — including heavy metals and lipophilic compounds bound to plasma proteins
- Oxidized lipids — products of oxidative stress that drive endothelial damage
What the system does not remove: red blood cells, white blood cells, platelets, albumin, immunoglobulins, and other essential blood components are returned to you. This selectivity is what makes H.E.L.P. different from a simple plasma exchange — it targets pathological molecules while preserving the components your body needs.
Before Your Session: Preparation
The Days Before
Preparation for apheresis is straightforward. There is no bowel prep, no fasting requirement, and no need to stop most medications. Here is what I tell patients:
Hydration is important. Drink at least 2-3 liters of water in the 24 hours before your session. The procedure involves processing a significant volume of your plasma, and good hydration makes the process smoother — veins are easier to access, blood flow is better, and you will feel better afterward. This is not optional advice. Patients who arrive dehydrated have a harder time.
Eat a light meal 2-3 hours before. Do not come fasting — your blood sugar should be stable. But do not eat a heavy meal immediately before either. A moderate breakfast or lunch with protein and complex carbohydrates is ideal.
Wear comfortable clothing with accessible arms. You will need IV access in both antecubital areas (the inside of your elbows). Short sleeves or sleeves that roll up easily are practical.
Medication review. Your physician will review your medications during the initial consultation. Most medications do not need to be adjusted, but blood thinners (anticoagulants) require specific timing considerations because heparin is used during the procedure. If you take warfarin, DOACs, or antiplatelet agents, discuss timing with your physician before the session.
Bring something to pass the time. The procedure takes 2-3 hours. You will be sitting in a comfortable chair, conscious and alert. Bring a book, your phone, headphones, or whatever keeps you comfortable. Some patients nap. Others watch movies on their tablets. One of my patients brings knitting.
The Morning Of
Arrive on time. The setup process takes 15-20 minutes, and running late compresses the session or delays other patients. I recommend arriving 10-15 minutes early for your first session to allow time for any last-minute questions.
A nurse will check your vitals — blood pressure, heart rate, temperature. This is baseline data and a safety check. If your blood pressure is unusually low or you are showing signs of dehydration, we may want to give you IV fluids before starting.
You will also have a brief conversation with the treating physician (or the physician will have seen you in consultation beforehand) to confirm the indication, review your labs, and answer any remaining questions.
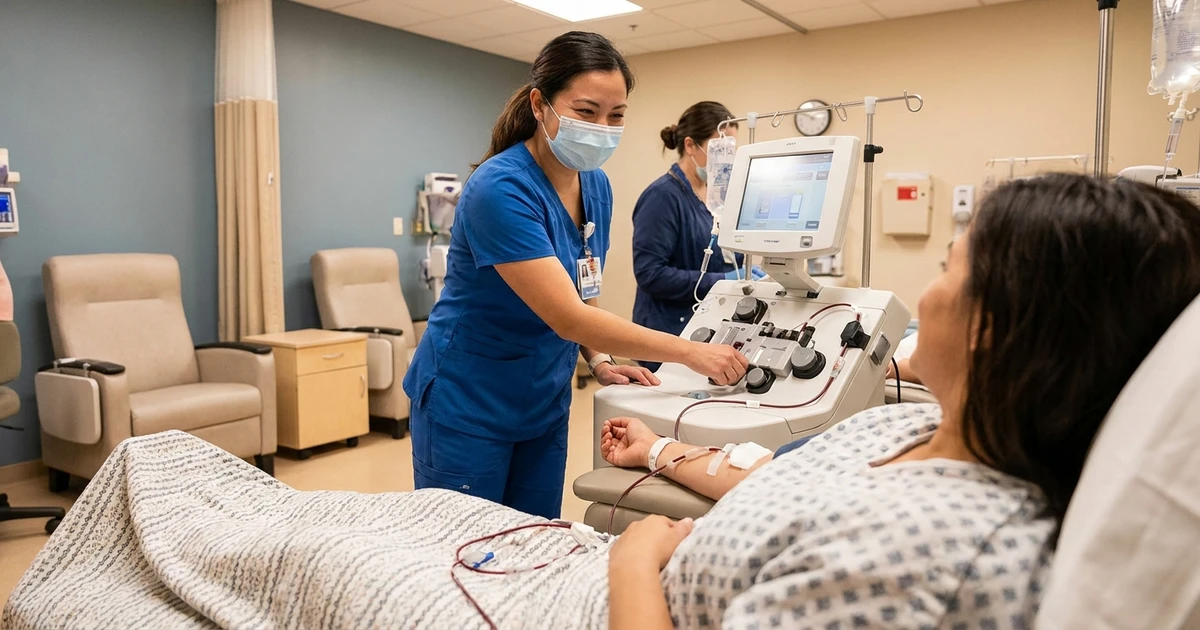
During the Procedure: Step by Step
Step 1: IV Access (5-10 minutes)
Two peripheral IV lines are placed — one in each arm, typically in the antecubital veins (the prominent veins at the inside of your elbow). One line draws blood out; the other returns filtered blood.
What it feels like: Like a standard blood draw — a brief pinch, then a pressure sensation as the line is secured. The needles used are similar in gauge to those used for blood donation. If you have difficult veins, let the nurse know — we have experienced staff and ultrasound guidance available if needed.
For patients anxious about needles: I understand. Many of my patients have had extensive medical experiences and developed legitimate needle anxiety. We can apply topical numbing cream (EMLA) 30-45 minutes before the procedure. Some patients find that listening to music or a guided meditation during access helps. The actual needle placement takes seconds — the anticipation is almost always worse than the reality.
Step 2: The Circuit Primes (5 minutes)
Before your blood enters the circuit, the system is primed with saline solution. You will see the lines fill with clear fluid. The machine runs through automated safety checks — pressure sensors, air detectors, and flow monitors are all verified. The nurse and/or technician will confirm that all parameters are normal before connecting the circuit to your IV lines.
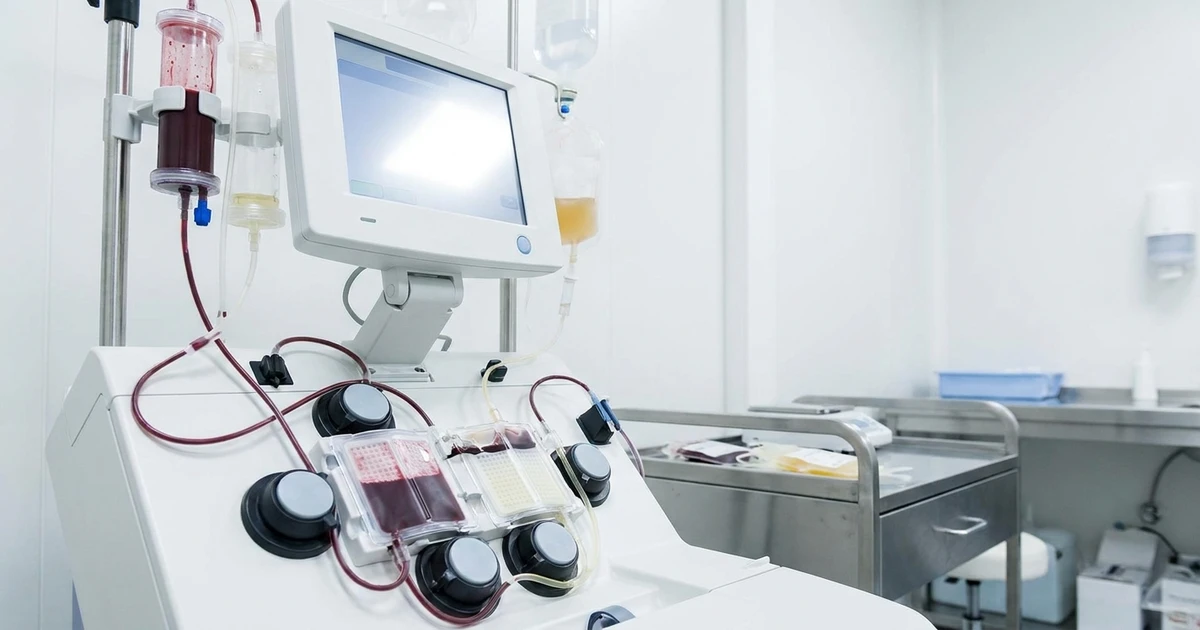
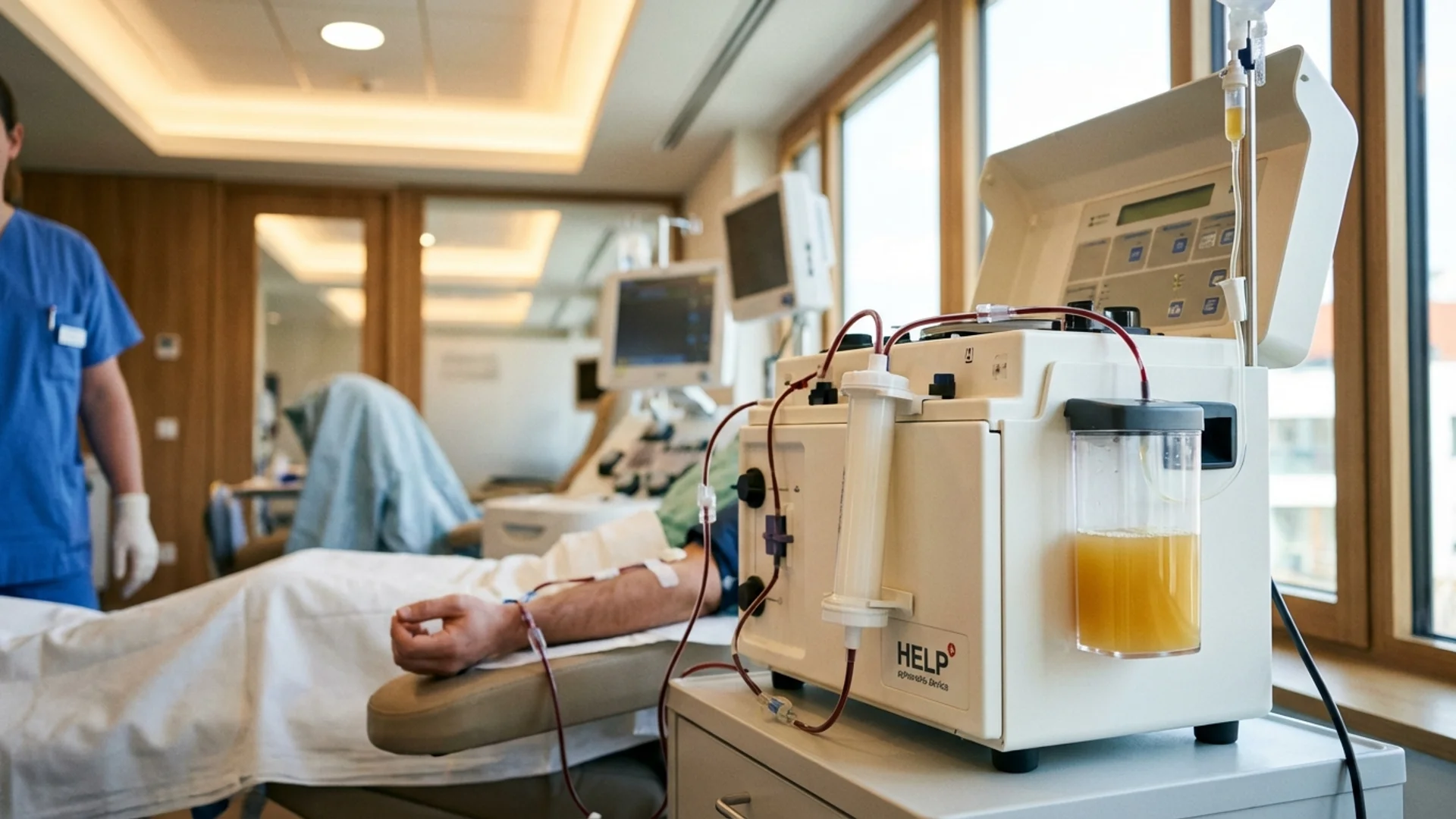
Step 3: Blood Processing Begins (2-2.5 hours)
Once the circuit is connected, blood flows from the draw line through the apheresis system and returns through the return line. Here is what happens inside the machine:
- Your blood is mixed with heparin (an anticoagulant) to prevent clotting in the circuit
- Plasma is separated from blood cells using a filter membrane
- The plasma passes through the precipitation step where heparin and a buffer solution cause the target proteins (LDL, fibrinogen, CRP, toxins) to precipitate out of solution
- The precipitate is removed by filtration
- The cleaned plasma is recombined with your blood cells
- Heparin is neutralized with a buffer before blood returns to you
- Filtered blood returns through the second IV line
What you feel during processing:
- First 15-20 minutes: Most patients feel nothing unusual. You may notice a slight coolness in the return arm as the filtered blood returns — this is normal and resolves as the system equilibrates.
- During the session: The most common sensation is a tingling or mild numbness around the lips or fingertips. This is caused by the citrate (calcium-binding) effect of the processing and is harmless. If it becomes uncomfortable, we slow the return rate or give a small calcium supplement. Let your nurse know immediately if you experience this.
- Blood pressure: Some patients experience a mild drop in blood pressure during the procedure. This is why we monitor vitals throughout. If you feel lightheaded or dizzy, speak up. This is manageable and not dangerous when caught early.
- Temperature: You may feel slightly cool as blood circulates outside your body. We have blankets available.
What you should not feel:
- Significant pain (beyond the IV insertion site)
- Chest pain or difficulty breathing
- Severe dizziness or vision changes
If you experience any of these, tell the nurse immediately. Serious adverse events are rare, but our team is trained to manage them.
Step 4: Completion and Line Removal (10-15 minutes)
When the programmed volume has been processed, the machine begins the return phase — all blood in the circuit is returned to you. The IV lines are removed, and pressure is applied to the puncture sites for 3-5 minutes. Bandages are placed.
Your vitals are checked one final time. You will be asked to sit for 10-15 minutes before standing, and a nurse will ensure you are stable before you leave.
What Patients Commonly Experience After Apheresis
I am going to be specific here because vague reassurances are not helpful. Based on performing this procedure regularly and systematically documenting patient feedback, here is what most patients report:
The First Few Hours
Fatigue is the most common post-procedure experience. Roughly 60-70% of patients report feeling tired in the hours after apheresis. This is not the exhaustion of illness — patients describe it more as the pleasant tiredness after vigorous exercise. Your body has just had a significant volume of inflammatory mediators removed, and it is recalibrating.
Mild lightheadedness can occur, especially if you did not hydrate adequately before the session. This resolves with fluids and rest.
Hunger. Many patients are surprisingly hungry after the procedure. Eat a substantial meal. Your body is rebuilding plasma proteins, and it needs nutrients.
Bruising at IV sites. Some patients develop bruising at the puncture sites. This is cosmetic and resolves in 3-7 days. Applying pressure for a full 5 minutes after line removal minimizes this.
The Next 24-48 Hours
This is where the interesting part begins.
Mental clarity. The single most commonly reported benefit — and the one that surprises patients the most — is improved mental clarity within 24-48 hours. Patients describe it as “the fog lifting,” “thinking more sharply,” or “feeling like myself for the first time in months.” In my clinical experience, this is particularly pronounced in patients with chronic infection sequelae, post-COVID cognitive symptoms, or environmental toxin burden.
Improved energy. Related to clarity but distinct — patients often report better sustained energy rather than the crash-and-surge pattern common in inflammatory conditions.
Reduced pain. Patients with chronic pain related to inflammatory conditions often notice reduced pain intensity within 48-72 hours. This is consistent with the acute reduction in inflammatory mediators that the procedure achieves.
Sleep improvement. Many patients report sleeping more deeply the night after apheresis. Whether this is the fatigue effect or a direct consequence of reduced inflammatory load is unclear, but the pattern is consistent enough to mention.
What You Might Not Feel
I want to be honest about this too: not every patient experiences dramatic improvement after a single session. Some patients — particularly those with long-standing chronic conditions — notice subtle changes that accumulate over a series of sessions rather than a dramatic shift after the first one.
If your first session produces only mild fatigue and a vague sense of “something different” but no clear improvement, that does not mean the procedure did not work. Lab values (CRP, fibrinogen, LDL) will show objective changes even when subjective improvement is gradual. Trust the labs while waiting for the clinical response to build.
How Many Sessions Do You Need?
This depends entirely on the clinical indication and your response. General guidance from my practice:
| Indication | Typical Protocol | Frequency |
|---|---|---|
| Cardiovascular risk reduction (elevated Lp(a), LDL) | 6-10 sessions, then maintenance | Weekly initially, then every 2-4 weeks |
| Chronic infection sequelae (post-Lyme, post-COVID) | 3-6 sessions | Weekly or biweekly |
| Environmental toxin burden | 4-8 sessions | Weekly |
| Acute inflammatory crisis | 2-4 sessions | Every 2-3 days |
| Maintenance (ongoing) | Ongoing | Every 4-8 weeks |
I reassess after every 3 sessions. Lab markers (CRP, fibrinogen, LDL, toxin panels) guide the decision to continue, space out, or stop.
Risks and Contraindications
Every medical procedure carries risks. Apheresis is well tolerated, but I believe in full transparency.
Common (occur in >5% of patients):
- Mild hypotension during procedure
- Citrate-related tingling (perioral, fingertips)
- Fatigue post-procedure
- Bruising at IV sites
Uncommon (1-5%):
- Nausea during procedure
- Vasovagal response (feeling faint)
- Hematoma at puncture site
Rare (<1%):
- Allergic reaction to heparin or circuit materials
- Significant hypotension requiring intervention
- Air embolism (prevented by automated air detection systems)
- Infection at IV site
Contraindications:
- Active bleeding or severe coagulation disorders
- Heparin-induced thrombocytopenia (HIT) — an allergy-like reaction to heparin
- Severe hemodynamic instability
- Severe anemia (hemoglobin below 8 g/dL)
- Active sepsis
If you have a history of heparin sensitivity or HIT, alternative anticoagulation protocols exist. Discuss this with your physician before scheduling.
What to Do After Your Session
Day of the procedure:
- Hydrate aggressively — 2-3 liters of water or electrolyte solution
- Eat a protein-rich meal within 2 hours
- Avoid strenuous exercise
- Do not drive if you feel lightheaded (arrange transport if needed)
- Keep bandages on for 4-6 hours
The following days:
- Resume normal activity as tolerated
- Continue adequate hydration for 48 hours
- Monitor IV sites for signs of infection (increasing redness, warmth, swelling, or discharge)
- Take any prescribed supplements (your physician may recommend specific electrolytes or nutrients)
What to report to your physician:
- Persistent bleeding from puncture sites
- Signs of infection
- Unusual fatigue lasting more than 48 hours
- Any new or unusual symptoms
How Apheresis Fits Into a Treatment Protocol
At our hospital, apheresis is rarely a standalone treatment. It is part of an integrated protocol that may include:
- Whole-body hyperthermia for chronic infections
- IV laser therapy (photobiomodulation) for immune modulation and circulation
- Targeted antimicrobial therapy for active infections
- IV micronutrient support for replenishment
- Detoxification support protocols
The sequencing matters. In our standard protocol for chronic Lyme disease, for example, apheresis is typically performed before hyperthermia. The rationale: reducing the inflammatory and toxin burden first means the body handles the stress of hyperthermia more effectively, and the immune activation triggered by hyperthermia is more productive when the systemic inflammatory noise has been reduced.
This is not a procedure you should evaluate in isolation. Ask your physician how apheresis fits into your overall treatment plan, what it is expected to accomplish that other interventions cannot, and what the criteria are for continuing or discontinuing the series.
References
- Jaeger BR, Richter Y, Nagel D, et al. Longitudinal cohort study on the effectiveness of lipid apheresis treatment to reduce high lipoprotein(a) levels and prevent major adverse coronary events. Nat Clin Pract Cardiovasc Med. 2009;6(3):229-239.
- Moriarty PM, Hemphill LC, Toth PP, et al. Lipoprotein apheresis for lipoprotein(a) and cardiovascular disease. J Clin Lipidol. 2019;13(6):894-900.
- Straube R, Kingreen H, Rostin M. Therapeutic apheresis in clinical practice: a review. Transfus Med Hemother. 2012;39(2):80-86.
- Pokrovsky SN, Ezhov MV, Il’ina LN, et al. Association of lipoprotein(a) excess with early vein graft occlusions in middle-aged men undergoing coronary artery bypass surgery. J Thorac Cardiovasc Surg. 2003;126(4):1071-1075.
- Julius U, Fischer S, Schatz U, et al. Why an apheresis center should offer more than one apheresis method. Ther Apher Dial. 2013;17(2):179-184.
- Schwartz J, Padmanabhan A, Aqui N, et al. Guidelines on the use of therapeutic apheresis in clinical practice — evidence-based approach. J Clin Apher. 2016;31(3):149-338.