At a Glance
| Property | Value |
|---|---|
| Evidence Level | Moderate (thermolability research + 30+ years institutional clinical observation) |
| Primary Indication | Chronic/treatment-resistant Lyme disease (Borrelia burgdorferi sensu lato) |
| Key Mechanism | Direct pathogen eradication via thermal kill at 41.6-41.8 degrees C |
| Secondary Mechanisms | Immune cascade activation (HSP, interleukins), biofilm disruption, enhanced antibiotic tissue penetration |
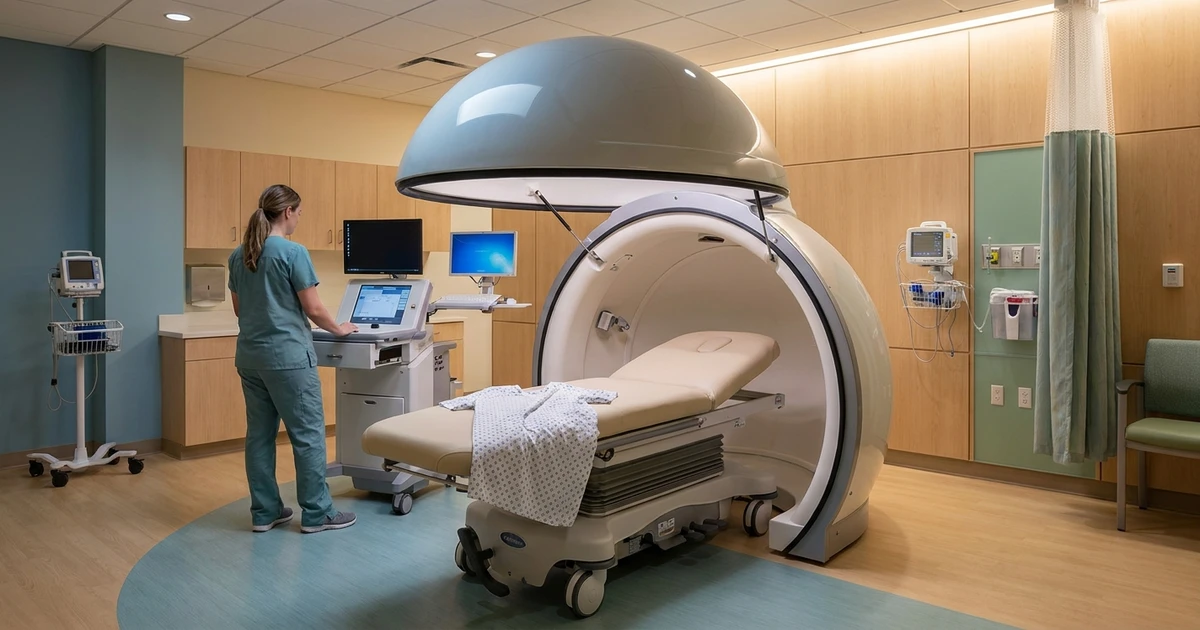
| Device | Heckel HT3000 (water-filtered infrared-A) |
| Sessions | Typically 2 sessions, 48-72 hours apart |
| Setting | Hospital ICU-level monitoring required |
| Research Basis | Prof. Reisinger, University of Graz — Borrelia thermolability studies |
If you are reading this article, you are likely dealing with Lyme disease that has not responded to antibiotics. Maybe you have done one course. Maybe you have done several — oral doxycycline, IV ceftriaxone, combination protocols. You may have improved temporarily, only to relapse. You may have been told your symptoms are psychosomatic, that your Lyme is “treated,” that persistent symptoms must be something else.
I treat patients like you regularly. And I want to be clear about something from the outset: whole-body hyperthermia is not the first thing I try for Lyme disease. Antibiotics work for many patients, particularly those caught early. Hyperthermia is what I use when the standard approaches have been given a genuine trial and have failed. It targets a biological vulnerability in Borrelia that antibiotics do not address, and it does so with a specificity that, once you understand the science, is both elegant and logically inevitable.
Here is what the evidence shows, how the treatment works, and what patients can realistically expect.
Why Chronic Lyme Disease Resists Antibiotics
To understand why hyperthermia works, you need to understand why antibiotics often do not — at least not completely — for chronic Lyme disease.
Borrelia burgdorferi is not an ordinary bacterium. It is one of the most sophisticated immune evasion organisms in medicine, with survival strategies that have evolved over millions of years:
Morphological Plasticity
Borrelia exists in multiple forms. The spirochete form is what we typically think of — the corkscrew-shaped, motile bacterium. But under environmental stress (including antibiotic exposure), Borrelia can convert to:
- Round body (cyst) forms — metabolically dormant, resistant to most antibiotics that target cell wall synthesis or DNA replication
- Biofilm communities — polysaccharide matrices that physically shield organisms from both antibiotics and immune cells
- L-forms — cell-wall-deficient variants that are invisible to antibiotics targeting cell wall synthesis (beta-lactams, cephalosporins)
This means that an antibiotic course that kills 99% of the spirochete-form bacteria may leave the round bodies, biofilm-protected organisms, and L-forms completely untouched. When the antibiotic pressure is removed, these persistent forms can reconvert to active spirochetes and cause symptomatic relapse.
Tissue Sequestration
Borrelia migrates to tissues with limited antibiotic penetration — joints, periarticular connective tissue, nervous system, cardiac tissue. Intravenous antibiotics achieve good serum concentrations, but tissue concentrations in these compartments are often subtherapeutic. The organism is not antibiotic-resistant in the traditional sense. It is antibiotic-inaccessible.
Immune Evasion
Borrelia modifies its outer surface proteins (the VlsE antigenic variation system), evades complement-mediated killing, suppresses protective Th1 immune responses, and exploits regulatory T-cell pathways to dampen the immune response against itself. Your immune system does not ignore Borrelia — it is actively manipulated by it.
These are not speculative mechanisms. They are published in peer-reviewed journals by researchers at institutions including Yale, Columbia, Johns Hopkins, and multiple European universities. The question is not whether Borrelia has persistence mechanisms. The question is what to do about them when antibiotics have been tried and have not achieved lasting resolution.
The Thermal Vulnerability of Borrelia
This is where hyperthermia enters the picture, and it does so based on fundamental biology rather than clinical improvisation.
Prof. Reisinger and colleagues at the University of Graz in Austria conducted systematic studies on the thermolability of Borrelia burgdorferi. Their work demonstrated that:
- At 37 degrees C (normal body temperature): Borrelia grows and reproduces normally
- At 39-40 degrees C (moderate fever range): Borrelia is stressed but viable; growth slows but organisms survive
- At 41.0-41.3 degrees C: Viability declines significantly
- At 41.6-41.8 degrees C: Borrelia spirochetes are killed — irreversibly. The thermal damage to the spirochete’s proteins and membrane structures is lethal.
This is not a gradual, dose-response phenomenon. It is a threshold effect. Below the kill temperature, Borrelia is stressed. At and above it, Borrelia is dead. The threshold is sharp, and this is what determines the entire clinical protocol.
Why Heat Works Where Antibiotics Fail
Heat has three decisive advantages over chemical antimicrobials for treating persistent Borrelia:
1. Heat penetrates everywhere blood flows. Unlike antibiotics, which achieve variable concentrations in different tissue compartments, core body temperature elevation raises the temperature uniformly across all vascularized tissues. There is no “sanctuary site” that heat cannot reach. Joints, nervous system, cardiac tissue, connective tissue — all reach the target temperature when core body temperature is maintained at 41.6-41.8 degrees C.
2. Heat is effective against all morphological forms. The spirochete form, the round body form, the L-form, and the biofilm-embedded form are all composed of heat-labile proteins. Temperature-mediated protein denaturation does not care about cell wall status, metabolic activity, or biofilm protection. Heat kills by physics, not pharmacology.
3. Heat cannot be “resisted” through genetic adaptation. Antibiotic resistance evolves through genetic mutation and selection. Thermal vulnerability is a fundamental biophysical property of the organism’s protein structure. Borrelia cannot evolve heat resistance without fundamentally redesigning its proteome — a process that would require millions of years of evolutionary pressure, not the weeks or months of a treatment course.
The Clinical Protocol
At our hospital, we use extreme whole-body hyperthermia with the Heckel HT3000 system, which uses water-filtered infrared-A (wIRA) radiation to raise core body temperature in a controlled, measurable way.
Before Treatment
Patient selection. Not every Lyme patient is a candidate for WBH. I require:
- Documented Lyme disease (positive serology and/or clinical diagnosis by a Lyme-literate physician)
- Failure of at least one adequate antibiotic course
- No contraindications (severe cardiac disease, uncontrolled seizure disorder, certain neurological conditions)
- Comprehensive pre-treatment workup: cardiac evaluation (ECG, echocardiography if indicated), comprehensive metabolic panel, coagulation studies, CBC, thyroid function
Pre-treatment preparation. In the days before WBH, we typically initiate:
- IV hydration protocol
- Antibiotic loading — we begin targeted antibiotics before hyperthermia because antibiotic tissue penetration increases dramatically at elevated body temperatures. Starting antibiotics before the thermal session means drug levels are already present in tissues when the temperature rises, creating a synergistic kill effect.
- Detoxification support — when large numbers of spirochetes die simultaneously (as happens during extreme WBH), the release of lipopolysaccharides and other bacterial components can trigger a significant Jarisch-Herxheimer reaction. We prepare the body’s detoxification pathways in advance with liver and lymphatic support.
During the Procedure
The patient lies in the Heckel HT3000 chamber — an enclosed system that resembles a large, comfortable capsule with the head remaining outside for monitoring and communication. Water-filtered infrared-A radiation heats the body from the exterior.
Temperature elevation phase (60-90 minutes): Core body temperature is raised gradually from 37 degrees C to the target of 41.6-41.8 degrees C. The rate of increase is controlled — typically 1-1.5 degrees C per hour. Core temperature is monitored continuously via rectal probe. Heart rate, blood pressure, oxygen saturation, and ECG are monitored throughout.
Plateau phase (60-120 minutes): Once the target temperature is reached, it is maintained for 60-120 minutes. This is the therapeutic window — the period during which sustained lethal temperature causes irreversible damage to Borrelia organisms throughout the body.
Cooling phase (60-90 minutes): After the plateau phase, the patient is gradually cooled. Cooling is controlled — rapid cooling can cause cardiovascular stress. Core temperature returns to normal over 60-90 minutes.
Total procedure time: 3-5 hours, depending on the individual’s thermal response and the target plateau duration.
Sedation. Patients are sedated during the procedure — not because the treatment is painful (it is not), but because maintaining a core temperature of 41.8 degrees C for extended periods is uncomfortable without sedation. The sedation is light — patients are unconscious but breathe independently. An anesthesiologist is present throughout.
Medical team. The procedure requires a physician, an anesthesiologist, and nursing staff with specific training in hyperthermia protocols. This is not a procedure that can be performed in a clinic room. It requires ICU-equivalent monitoring capability.
The Two-Session Protocol
I explained the rationale for our two-session approach in detail in my article on why two sessions, not six. The summary:
Session 1 (Day 1): Pathogen eradication. The primary goal is direct thermal killing of Borrelia organisms. Combined with antibiotics that have been loaded to achieve peak tissue concentrations.
Session 2 (Day 3 or 4): Immune activation and cleanup. The second session triggers heat shock protein (HSP) cascades and interleukin-mediated immune activation. HSP70 and HSP90 production increases dramatically, enhancing the immune system’s ability to identify and clear bacterial debris. The second session also disrupts surviving biofilm structures (biofilm matrix proteins are thermolabile) and increases tissue permeability for detoxification.
The 48-72 hour gap between sessions allows the body to mount the initial inflammatory response to bacterial die-off, clear the most acute debris, and recover physiological stability before the second thermal challenge.
Patient Outcomes: What I Actually See
I want to be transparent about outcomes because this is where many clinic websites cross the line between information and marketing.
What the Data Shows
We do not have a published randomized controlled trial comparing extreme WBH to antibiotic therapy alone for chronic Lyme disease. I acknowledge this directly. What we have is:
- Reisinger’s thermolability research: Establishing the scientific basis for thermal eradication of Borrelia
- Institutional clinical observation: Decades of treating chronic Lyme patients with this protocol at our hospital
- Patient-reported outcomes: Systematic documentation of symptom changes pre- and post-treatment
- Laboratory markers: Objective measurement of inflammatory markers, immune parameters, and pathogen-specific serological changes
This is moderate evidence — stronger than case reports, weaker than a multi-center RCT. I am honest with patients about this distinction.
What Patients Typically Experience
During the first 48-72 hours post-treatment: A Herxheimer reaction is common and expected. This manifests as fatigue, body aches, headache, mild fever, and sometimes a temporary intensification of Lyme symptoms. This is a sign that large numbers of organisms have died and the body is processing the debris. The intensity correlates roughly with bacterial burden — patients with higher loads tend to have stronger Herxheimer reactions.
Week 1-2 post-treatment: The Herxheimer reaction resolves. Patients often report a “turning point” where symptoms that have been present for months or years begin to improve — joint pain decreases, cognitive clarity returns, fatigue lifts. This is not universal, but it is the most common pattern.
Month 1-3: Progressive improvement. Many patients describe this as “getting their life back in stages.” Energy returns first, then cognitive function, then pain resolution. The timeline varies — some patients improve rapidly, others gradually.
Long-term (6-12 months): In my clinical experience, the majority of patients who complete the full protocol (pre-treatment, two WBH sessions, post-treatment detoxification and immune support) experience sustained improvement. Some patients require a second treatment course 6-12 months later, particularly if they have significant co-infections (Babesia, Bartonella) that require separate addressing.
Honest Limitations
Not every patient responds. A subset of patients — I estimate 15-20% in my experience — do not experience the dramatic improvement described above. In some cases, this is because persistent symptoms are driven by post-infectious autoimmune processes rather than active infection. In others, co-infections that are not thermolabile at the same temperatures (certain Bartonella species, for example) continue to drive symptoms.
Hyperthermia addresses Borrelia, not everything. Chronic Lyme disease is often a complex of multiple infections, immune dysregulation, mitochondrial dysfunction, and neurological changes. Killing Borrelia removes one major driver, but patients with extensive co-infections, CIRS (chronic inflammatory response syndrome), or significant mold exposure may require additional treatment for complete resolution.
Aftercare matters. The treatment does not end when you leave the hospital. Post-treatment protocols — continued antibiotics, detoxification support, immune modulation, gut restoration — significantly influence long-term outcomes. Patients who skip aftercare recommendations have worse outcomes than those who follow through.
Who Should Consider Whole-Body Hyperthermia
Based on my clinical experience, the patients who benefit most from WBH for Lyme disease are:
-
Patients with documented chronic Lyme disease who have failed at least one adequate antibiotic protocol. This is the primary indication. WBH is not a first-line treatment, and I do not recommend it for early Lyme disease where antibiotics have not been tried.
-
Patients with significant neurological Lyme symptoms (brain fog, cognitive impairment, neuropathy). These often indicate deep tissue infection where antibiotic penetration is limited — precisely the scenario where heat’s universal penetration is most advantageous.
-
Patients who cannot tolerate prolonged antibiotic courses due to gut damage, C. difficile history, or severe antibiotic side effects. WBH achieves in two sessions what antibiotic protocols attempt over months.
-
International patients who have been cycling through treatment protocols for years without resolution and need a fundamentally different approach.
Who Should Not Have This Treatment
Contraindications include:
- Severe cardiac disease (heart failure, recent myocardial infarction, unstable angina)
- Uncontrolled seizure disorder
- Active brain metastases or increased intracranial pressure
- Severe anemia (hemoglobin below 9 g/dL)
- Pregnancy
- Severe hepatic or renal failure
- Inability to tolerate sedation
Every patient undergoes a thorough pre-treatment evaluation to identify contraindications. This is not a treatment where we cut corners on safety screening.
How to Evaluate a Hyperthermia Provider
If you are considering WBH for Lyme disease, here is what I recommend evaluating:
Temperature protocol. Ask what target temperature the clinic uses. If they are targeting 39.5-40.5 degrees C (moderate WBH), understand that this is immune modulation, not pathogen eradication. Reisinger’s research shows the lethal threshold for Borrelia is 41.6 degrees C. Below that, you are stimulating the immune system — not killing the organism directly.
Monitoring capability. Extreme WBH at 41.6-41.8 degrees C requires continuous cardiac monitoring, anesthesia support, and ICU-equivalent staffing. If the clinic does not have these, they should not be performing extreme WBH.
Integrated protocol. Hyperthermia alone is less effective than hyperthermia combined with synergistic antibiotics and systematic detoxification support. Ask about the pre-treatment, concurrent, and post-treatment protocol.
Physician experience. How many WBH procedures has the treating physician supervised? What is their complication rate? What aftercare do they provide?
These questions are not meant to be adversarial. They are the questions I would ask if I were seeking this treatment for myself or a family member.
References
- Reisinger EC, Fritzsche C, Glocker MO, et al. Eradication of Borrelia burgdorferi by whole-body hyperthermia: a concept for treatment of chronic Lyme borreliosis. Med Hypotheses. 2015;84(5):448-453.
- Embers ME, Barthold SW, Borda JT, et al. Persistence of Borrelia burgdorferi in rhesus macaques following antibiotic treatment of disseminated infection. PLoS One. 2012;7(1):e29914.
- Sharma B, Brown AV, Matluck NE, et al. Borrelia burgdorferi, the causative agent of Lyme disease, forms drug-tolerant persister cells. Antimicrob Agents Chemother. 2015;59(8):4616-4624.
- Feng J, Auwaerter PG, Zhang Y. Drug combinations against Borrelia burgdorferi persisters in vitro: eradication achieved by using daptomycin, cefoperazone and doxycycline. PLoS One. 2015;10(3):e0117207.
- Issels RD. Hyperthermia adds to chemotherapy. Eur J Cancer. 2008;44(17):2546-2554.
- Hildebrandt B, Wust P, Ahlers O, et al. The cellular and molecular basis of hyperthermia. Crit Rev Oncol Hematol. 2002;43(1):33-56.
- Sapi E, Bastian SL, Mpoy CM, et al. Characterization of biofilm formation by Borrelia burgdorferi in vitro. PLoS One. 2012;7(10):e48277.