At a Glance
| Property | H.E.L.P. Apheresis | INUSpheresis |
|---|---|---|
| Full Name | Heparin-induced Extracorporeal LDL Precipitation | INUS Apheresis (proprietary system) |
| Evidence Level | Strong (decades of published clinical data, registered medical device) | Limited (sparse peer-reviewed publications, predominantly marketing literature) |
| Mechanism | Heparin precipitation → LDL, Lp(a), fibrinogen, CRP removal | Proprietary adsorber filters → broad-spectrum binding |
| Published Clinical Studies | 100+ peer-reviewed publications | Minimal peer-reviewed publications |
| Regulatory Status | CE-marked medical device; established in cardiology guidelines | CE-marked; not referenced in major clinical guidelines |
| Primary Established Indication | Severe hypercholesterolemia, elevated Lp(a) | Marketed for environmental toxin and inflammatory mediator removal |
| Device Manufacturer | B. Braun (established medical device company) | INUS Medical Center (smaller, proprietary) |
| Cost per Session | 800-2,500 EUR | 1,500-5,000 EUR |
| Session Duration | 2-3 hours | 2-4 hours |
Patients who research blood filtration therapies — particularly those with chronic inflammatory conditions, Lyme disease, post-COVID, or environmental illness — inevitably encounter both H.E.L.P. Apheresis and INUSpheresis. Online, these procedures are sometimes presented as interchangeable or as competitors addressing the same need. They are not. The mechanisms, evidence bases, and clinical maturity of these two systems are substantially different, and patients deserve to understand those differences before committing to either.
I use H.E.L.P. Apheresis as one of our three signature treatments at Klinik St. Georg. I have chosen not to use INUSpheresis. Here is why, with full transparency about the reasoning.
H.E.L.P. Apheresis: The Evidence-Based System
What It Is
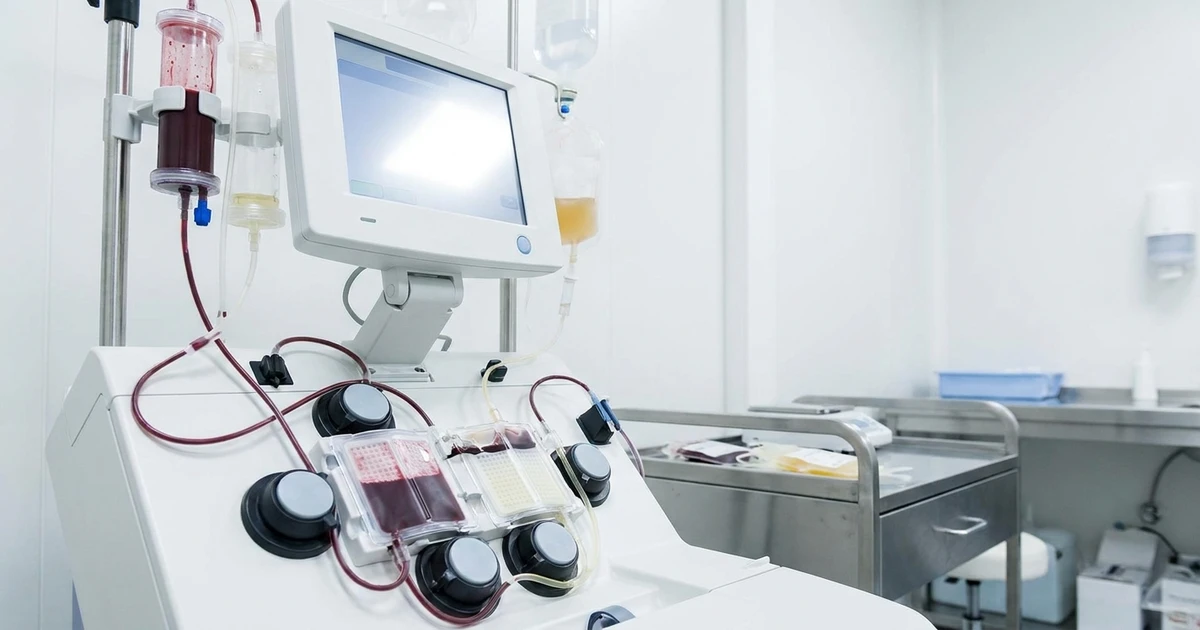
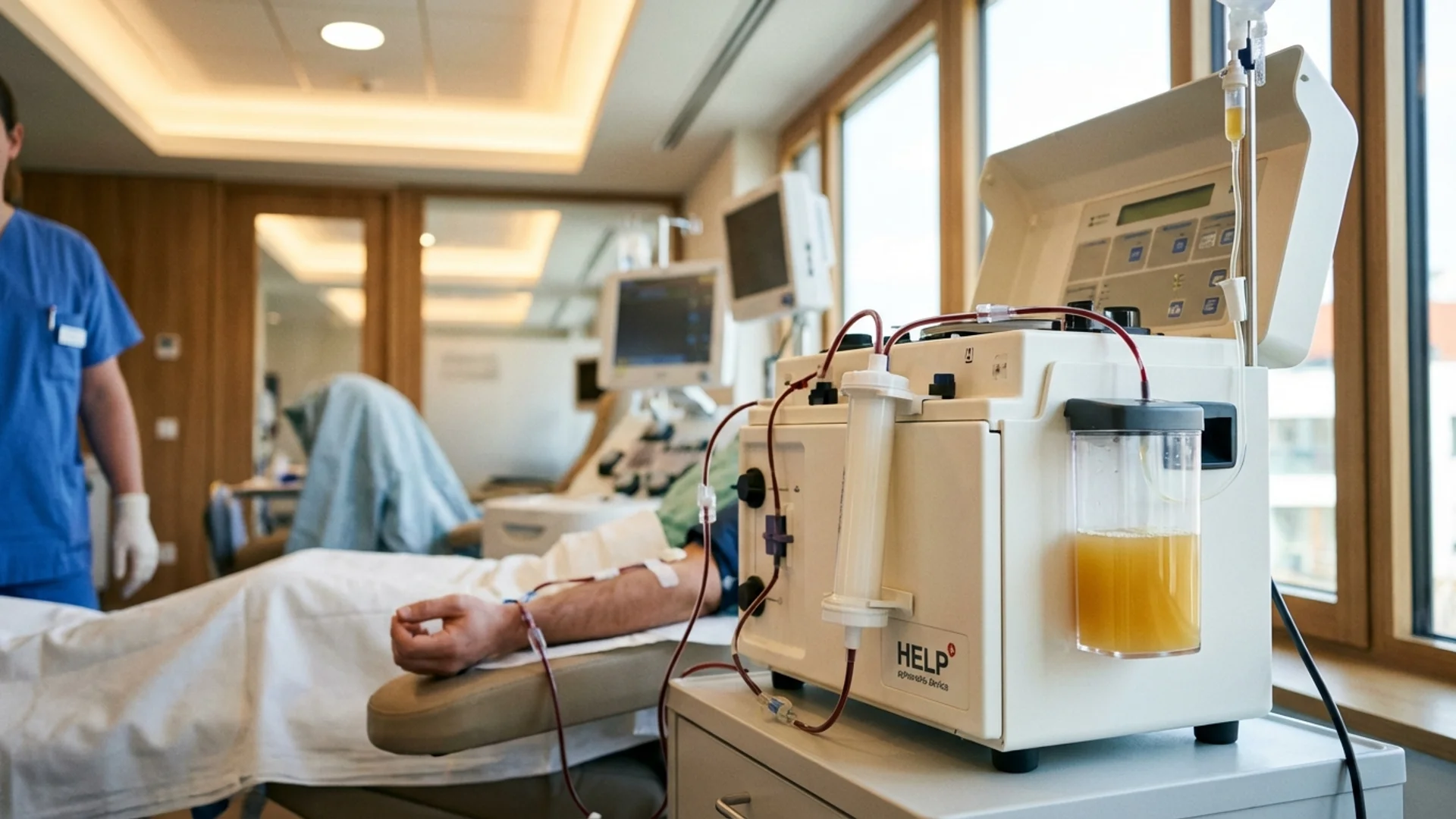
H.E.L.P. stands for Heparin-induced Extracorporeal LDL Precipitation. It is a therapeutic apheresis procedure developed in the 1980s and manufactured by B. Braun, one of the world’s largest medical device companies. The system selectively removes specific pathogenic molecules from the blood [1].
How It Works
The H.E.L.P. procedure follows a defined biochemical process:
-
Blood separation. Whole blood is drawn from one arm and separated into plasma and cellular components using a standard plasmapheresis membrane.
-
Heparin precipitation. The plasma is mixed with heparin at a low pH (approximately 5.12). At this pH, heparin selectively binds to and precipitates LDL cholesterol, lipoprotein(a) [Lp(a)], fibrinogen, and C-reactive protein (CRP). These molecules form insoluble complexes that fall out of solution.
-
Precipitation filtration. The precipitated complexes are removed by filtration through a polycarbonate filter.
-
Heparin adsorption. Excess heparin is removed from the plasma by passage through a DEAE-cellulose adsorber, restoring normal heparin levels.
-
Bicarbonate dialysis. The plasma is dialyzed against a bicarbonate buffer to restore physiological pH.
-
Reconstitution. The cleaned plasma is recombined with the cellular components and returned to the patient through a vein in the other arm.
The entire process takes 2 to 3 hours and is performed in a clinical setting with nurse monitoring.
What H.E.L.P. Removes (and How Much)
The selectivity of H.E.L.P. is one of its key advantages. It does not indiscriminately remove all plasma proteins. It targets specific pathogenic molecules:
| Substance | Single-Session Reduction | Clinical Significance |
|---|---|---|
| LDL cholesterol | 55-70% | Primary cardiovascular risk factor |
| Lipoprotein(a) | 55-70% | Independent cardiovascular risk factor with no pharmaceutical treatment |
| Fibrinogen | 50-60% | Elevated in inflammation; increases blood viscosity and thrombosis risk |
| C-reactive protein | 50-60% | Acute-phase inflammatory marker |
| Immunoglobulins | 10-15% (non-targeted) | Minimal impact on immune function |
| Albumin | <5% loss | Clinically insignificant |
The selectivity is important. Albumin, immunoglobulins, and other essential plasma proteins are largely preserved. This is not a blunt filtering tool — it is a biochemically targeted precipitation system [2].
The Evidence Base
H.E.L.P. Apheresis has one of the most robust evidence bases of any apheresis procedure:
Cardiovascular applications (strongest evidence):
- Multiple prospective studies demonstrating reduction in cardiovascular events in patients with severe hypercholesterolemia refractory to statin therapy
- The H.E.L.P. LDL-Apheresis Registry has tracked outcomes in thousands of patients
- Recognized in European and German cardiology guidelines for treatment of severe familial hypercholesterolemia and elevated Lp(a)
- Published evidence of improved coronary blood flow, reduced carotid intima-media thickness, and decreased cardiovascular event rates [3]
Inflammatory conditions (moderate evidence):
- Published studies in sudden sensorineural hearing loss demonstrating improved outcomes compared to standard treatment alone
- Clinical data in peripheral arterial disease showing improved limb perfusion
- Observational data in chronic inflammatory conditions showing symptom improvement correlated with fibrinogen and CRP reduction
Chronic infection and post-infectious conditions (emerging evidence):
- Clinical observation at Klinik St. Georg and comparable centers in chronic Lyme disease, post-COVID syndrome, and chronic inflammatory conditions
- The mechanism is plausible: removing inflammatory mediators (fibrinogen, CRP) reduces the systemic inflammatory burden that persists after infection treatment
- Not yet validated in randomized controlled trials for these indications
Why We Use It
At Klinik St. Georg, H.E.L.P. Apheresis serves several clinical roles:
In chronic Lyme disease: After whole-body hyperthermia targets the infection itself, H.E.L.P. addresses the inflammatory aftermath. Chronic Lyme patients often have elevated fibrinogen, CRP, and inflammatory mediators that persist even after successful pathogen eradication. H.E.L.P. physically removes these molecules, providing immediate reduction in inflammatory burden.
In post-COVID syndrome: Many post-COVID patients present with elevated inflammatory markers, microclotting (associated with elevated fibrinogen), and persistent systemic inflammation. H.E.L.P.’s ability to reduce fibrinogen by 50 to 60 percent per session addresses the microclotting hypothesis directly.
In cardiovascular risk reduction: Patients with elevated Lp(a) — for which no approved pharmaceutical treatment exists — benefit from H.E.L.P.’s demonstrated 55 to 70 percent reduction per session. This is a recognized guideline-based indication.
INUSpheresis: What We Know
What It Is
INUSpheresis is a therapeutic apheresis procedure developed by the INUS Medical Center, a private clinic in Cham, Germany. It uses proprietary adsorber filters to bind and remove substances from the plasma.
How It Works (As Described by the Manufacturer)
The procedure, as described in INUS marketing and informational materials:
- Blood separation. Similar to H.E.L.P., blood is separated into plasma and cellular components.
- Adsorber filtration. Plasma passes through proprietary adsorber columns containing binding agents (the specific composition is proprietary and not fully disclosed in peer-reviewed literature).
- Return. Filtered plasma is recombined with cellular components and returned to the patient.
What INUSpheresis Claims to Remove
Marketing materials for INUSpheresis list a broader range of target substances than H.E.L.P.:
- Environmental toxins (heavy metals, pesticides, microplastics, solvents)
- Inflammatory mediators
- Oxidized lipids
- Biotoxins (mold toxins, bacterial toxins)
- Spike protein (post-COVID)
- Various metabolic waste products
The Evidence Problem
Here is where I must be direct, and this is the primary reason I do not use INUSpheresis in my practice.
Peer-reviewed publications. The published, peer-reviewed clinical evidence for INUSpheresis is sparse. A systematic search of PubMed and comparable databases yields minimal results compared to the hundreds of publications supporting H.E.L.P. Apheresis.
Proprietary filter composition. The exact composition and binding characteristics of the INUSpheresis adsorber filters are not fully disclosed in peer-reviewed literature. For H.E.L.P., the mechanism is completely transparent — the biochemistry of heparin precipitation at pH 5.12 is well-characterized. For INUSpheresis, we are asked to trust proprietary claims without the same level of independent verification.
Removal verification. H.E.L.P. has published data showing precisely what is removed and in what quantities, with pre- and post-treatment laboratory measurements documented across thousands of patients. INUSpheresis removal claims, particularly for environmental toxins, heavy metals, and spike protein, lack comparable independent verification in peer-reviewed publications.
No guideline recognition. H.E.L.P. is referenced in cardiovascular guidelines for specific indications. INUSpheresis is not referenced in any major clinical guidelines that I am aware of.
Cost premium. INUSpheresis sessions typically cost 1,500 to 5,000 EUR — often more than H.E.L.P. — which raises the question of whether the higher cost reflects greater therapeutic value or higher marketing margins.
What INUSpheresis May Do Well
I want to be fair. The absence of strong published evidence does not prove that INUSpheresis is ineffective. It is possible that:
- The adsorber technology does remove some of the substances claimed
- Patients genuinely improve after treatment (clinical observation from INUSpheresis practitioners exists)
- The broader removal spectrum, if real, could offer advantages for specific patient populations (particularly environmental toxin burden)
The issue is not that INUSpheresis is necessarily ineffective. The issue is that the evidence supporting its claims has not been subjected to the same level of independent scrutiny as H.E.L.P. And in medicine, unverified claims — even plausible ones — do not meet the threshold I hold myself to when recommending treatment to patients.
Head-to-Head Comparison
Evidence Quality
| Category | H.E.L.P. Apheresis | INUSpheresis |
|---|---|---|
| Peer-reviewed publications | 100+ | Minimal |
| Registered clinical trials | Multiple | Not identified |
| Guideline recognition | Yes (European cardiovascular) | No |
| Independent verification of removal | Extensively documented | Limited |
| Manufacturer transparency | Full mechanism disclosure | Proprietary filter composition |
| Long-term safety data | Decades of published data | Limited published safety data |
Mechanism Comparison
| Feature | H.E.L.P. | INUSpheresis |
|---|---|---|
| Mechanism | Biochemically defined (heparin precipitation at pH 5.12) | Adsorber-based binding (proprietary composition) |
| Selectivity | High — targets specific molecules | Claimed broad-spectrum |
| Predictability | Removal rates well-characterized | Removal rates less well-characterized |
| Reproducibility | Consistent across published studies | Less independently verified |
Clinical Application
| Indication | H.E.L.P. Evidence | INUSpheresis Evidence |
|---|---|---|
| Severe hypercholesterolemia | Strong (guideline-based) | Not established |
| Elevated Lp(a) | Strong (guideline-based) | Not established |
| Chronic inflammation | Moderate (clinical data) | Anecdotal/marketing |
| Post-COVID | Emerging (plausible mechanism + observation) | Emerging (claims, limited publication) |
| Environmental toxin removal | Not the primary purpose | Central marketing claim, limited verification |
| Chronic infection (Lyme) | Moderate (institutional experience) | Anecdotal |
Cost Comparison
| Factor | H.E.L.P. | INUSpheresis |
|---|---|---|
| Per session | 800-2,500 EUR | 1,500-5,000 EUR |
| Typical course (3-5 sessions) | 2,400-12,500 EUR | 4,500-25,000 EUR |
| Insurance coverage (Germany) | Yes, for approved indications | Limited |
| Insurance coverage (international) | Variable, better documentation for claims | Variable, less documentation support |
What I Tell Patients Who Ask
Patients frequently ask me about INUSpheresis — often because they have seen marketing materials online or have been recommended it by other practitioners. Here is what I tell them:
I cannot recommend a treatment whose evidence base I have not been able to independently verify. The claims made for INUSpheresis may be accurate, but until they are supported by independent, peer-reviewed publications with the same rigor that supports H.E.L.P., I cannot in good conscience prescribe it.
H.E.L.P. does what we need it to do. For the indications we treat at Klinik St. Georg — inflammatory burden reduction in chronic Lyme, post-COVID, and cardiovascular risk — H.E.L.P. Apheresis has published, verified efficacy. It removes the specific molecules that are pathogenic in these conditions, and it does so predictably and reproducibly.
Broader removal is not automatically better. The INUSpheresis marketing emphasizes removing a wider range of substances than H.E.L.P. But in medicine, specificity is often more valuable than breadth. Removing everything indiscriminately risks removing beneficial molecules along with pathogenic ones. H.E.L.P.’s selectivity — removing LDL, Lp(a), fibrinogen, and CRP while preserving albumin and most immunoglobulins — is a feature, not a limitation.
Follow the evidence. This is the principle that guides all of my clinical decisions. When INUSpheresis has a published evidence base comparable to H.E.L.P.’s, I will reevaluate. Until then, I prescribe the system whose claims I can verify.
Patient Selection for Apheresis
Regardless of which system is used, apheresis is not appropriate for every patient. At our clinic, the indications for H.E.L.P. Apheresis include:
Strong indications:
- Severe hypercholesterolemia refractory to maximal statin therapy
- Elevated Lp(a) above 60 mg/dL (no pharmaceutical alternative exists)
- Adjunctive treatment during chronic Lyme protocols (post-hyperthermia inflammatory burden reduction)
Moderate indications:
- Post-COVID syndrome with elevated inflammatory markers and suspected microclotting
- Chronic inflammatory conditions with elevated fibrinogen and CRP
Patients whose inflammatory burden is primarily antibody-driven — rheumatoid arthritis, lupus nephritis, myasthenia gravis — may achieve more targeted load reduction through immunoadsorption protocols that selectively deplete the IgG fraction rather than the broader lipid-fibrinogen profile H.E.L.P. targets. We detail the evidence and clinical selection criteria for this patient group in our apheresis for autoimmune disease guide.
- Sudden sensorineural hearing loss (time-sensitive — best within 10 days of onset)
Contraindications:
- Severe bleeding disorders
- Heparin-induced thrombocytopenia (HIT) — absolute contraindication for H.E.L.P.
- Severe anemia (hemoglobin below 8 g/dL)
- Hemodynamic instability
- Active sepsis
The Bottom Line
H.E.L.P. Apheresis and INUSpheresis are fundamentally different systems with vastly different evidence bases. H.E.L.P. has decades of peer-reviewed publications, guideline recognition, transparent mechanism disclosure, and verified removal data. INUSpheresis makes broader claims but with significantly less independent verification.
This does not mean INUSpheresis is worthless. It means the evidence does not yet support the claims. In medicine, “promising but unproven” and “proven” are different categories, and patients should understand which category each treatment falls into.
At Klinik St. Georg, we use H.E.L.P. Apheresis because we can verify what it does, predict what it will remove, and cite published evidence for its clinical effects. That is the standard our patients deserve.
References
- Seidel D, et al. The H.E.L.P.-apheresis system. Artificial Organs. 1996;20(4):335-339.
- Bosch T, et al. Heparin-induced extracorporeal LDL/fibrinogen precipitation — HELP — is an effective apheresis procedure for lowering cardiovascular risk. Atherosclerosis Supplements. 2009;10(5):95-99.
- Jaeger BR, et al. Longitudinal cohort study on the effectiveness of lipid apheresis treatment to reduce high lipoprotein(a) levels and prevent major adverse coronary events. Nature Clinical Practice Cardiovascular Medicine. 2009;6(3):229-239. doi:10.1038/ncpcardio1456.
- Thompson GR, et al. LDL apheresis. Atherosclerosis. 2003;167(1):1-13.
- Stefanutti C, et al. Lipoprotein apheresis and cardiovascular disease: a comprehensive review. Transfusion and Apheresis Science. 2021;60(4):103162. doi:10.1016/j.transci.2021.103162.
- Moriarty PM, et al. Lipoprotein(a) and its potential association with thrombosis and inflammation in COVID-19: a testable hypothesis. Current Atherosclerosis Reports. 2020;22(9):48. doi:10.1007/s11883-020-00867-3.
This content is educational and does not constitute medical advice. Apheresis procedures should only be performed in licensed clinical settings with proper medical oversight. Treatment decisions should be based on individual assessment by a qualified physician.