At a Glance
| Property | Value |
|---|---|
| Evidence Level | Moderate |
| Primary Use | Differential assessment during chronic infection treatment |
| Key Mechanism | Herx: cytokine cascade from pathogen die-off. Flare: immune activation or inflammatory response from non-treatment triggers |
The Question Every Lyme Patient Asks
You started antibiotics three days ago. Now you feel worse than before you began treatment. Your joints ache more. Your brain fog deepened. The fatigue is crushing. And you are asking yourself the question I hear in my clinic every single day: “Is this a Herxheimer reaction, or am I just getting sicker?”
This is not a trivial question. The answer determines whether you should continue treatment (Herx), modify treatment (Herx management), or investigate a different problem (disease flare). Getting it wrong in either direction has consequences — stopping effective therapy prematurely, or pushing through a genuine worsening that needs clinical attention.
Here is the framework I use to help patients and physicians distinguish between the two.
What Each One Actually Is
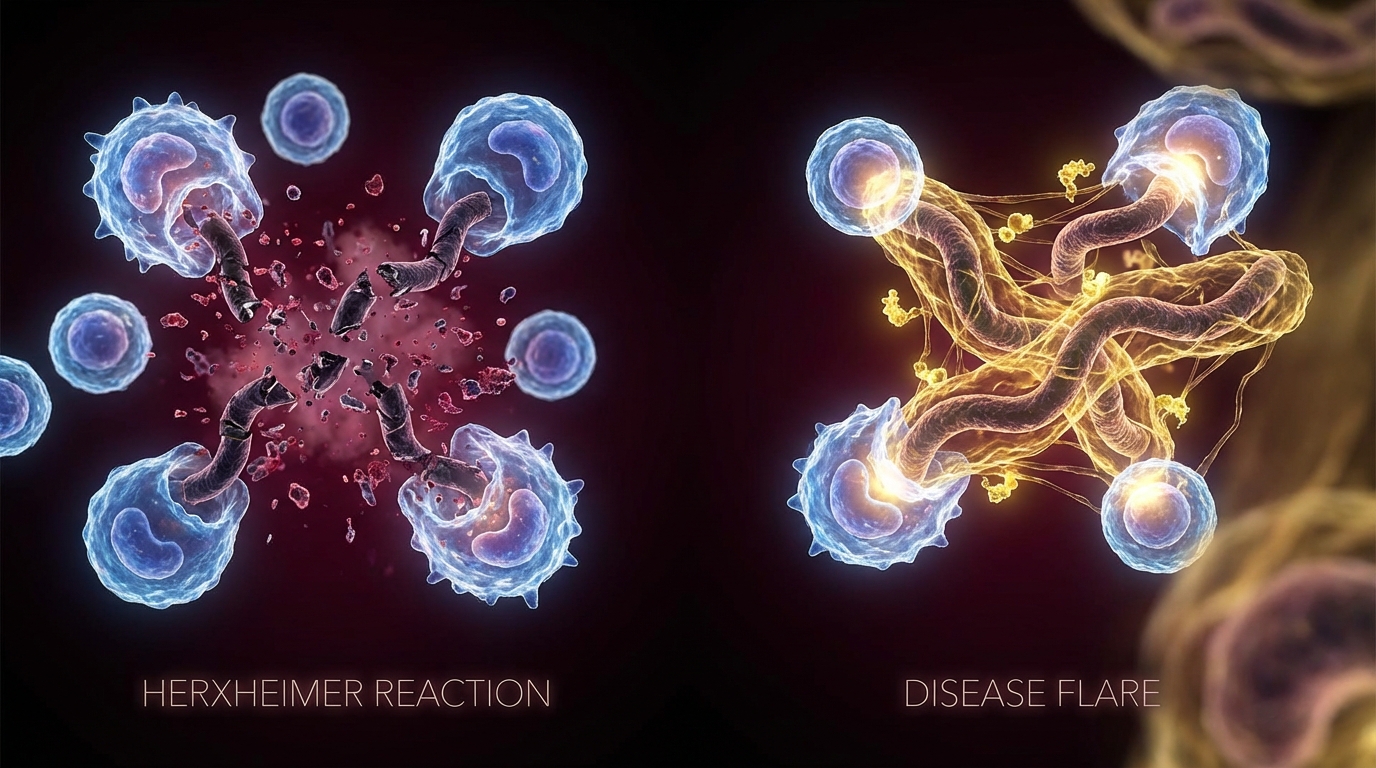
Herxheimer Reaction (Jarisch-Herxheimer Reaction)
A Herxheimer reaction is a transient, inflammatory response triggered by the rapid death of microorganisms during antimicrobial therapy. When pathogens are killed, they release endotoxins, lipoproteins, and other structural components that trigger a surge of pro-inflammatory cytokines — particularly TNF-alpha, IL-6, and IL-1beta [1].
Originally described in syphilis treatment (by Drs. Jarisch and Herxheimer in the 1890s), the reaction has been documented in the treatment of Lyme disease, relapsing fever, leptospirosis, and other spirochetal infections.
The trigger is always medication. Specifically, the initiation of antimicrobial therapy, an increase in dose, a change to a more effective agent, or the addition of a biofilm disruption protocol that exposes previously protected organisms.
Disease Flare
A disease flare is a worsening of symptoms caused by factors other than antimicrobial-induced pathogen die-off. Flares can result from:
- Physical or emotional stress
- Overexertion
- Sleep deprivation
- Dietary triggers (alcohol, sugar, inflammatory foods)
- Hormonal fluctuations (menstrual cycle)
- Weather or barometric pressure changes
- Concurrent viral illness
- Immune system fluctuations
- Environmental toxin exposure (mold, chemicals)
The trigger is not medication. Flares occur independently of antimicrobial therapy, though they can occur during treatment — which is exactly why they are confused with Herxheimer reactions.
The Diagnostic Framework
Timing
| Feature | Herxheimer Reaction | Disease Flare |
|---|---|---|
| Onset trigger | Within hours to 3 days of starting/changing antimicrobials | No clear temporal relationship to medication changes |
| Duration | Self-limiting: 3-7 days (sometimes up to 2 weeks) | Persists until the trigger is identified and addressed |
| Resolution | Resolves spontaneously with continued treatment | Does not resolve with continued treatment alone |
| Pattern | May recur with each dose increase or medication change | Tends to follow identifiable non-medication triggers |
The 72-hour rule: If symptoms worsen within 72 hours of starting or changing antimicrobial therapy, Herxheimer reaction is the most likely explanation. If symptoms worsen without any recent medication change, a disease flare is more likely.
Symptom Quality
| Feature | Herxheimer Reaction | Disease Flare |
|---|---|---|
| Symptom type | Intensification of existing symptoms (familiar symptoms, louder volume) | May include existing symptoms AND new symptom patterns |
| Systemic symptoms | Often includes flu-like features: fever, chills, malaise, sweating | Less likely to include true fever |
| Cognitive | Worsened brain fog, headache — same quality as baseline | May involve new cognitive patterns or different quality |
| Emotional | Irritability, mood lability (especially with Bartonella die-off) | Anxiety or depression may relate to identifiable stressor |
| Pain pattern | Migratory joint/muscle pain, often shifting locations | Tends to be fixed location, related to area of overuse or injury |
Clinical Context
| Feature | Herxheimer Reaction | Disease Flare |
|---|---|---|
| Treatment status | Currently receiving antimicrobial therapy | May or may not be on treatment |
| Recent changes | New medication, dose increase, added biofilm disruption | No recent treatment change |
| Preceding events | None beyond medication change | Identifiable stressor (overexertion, poor sleep, infection, mold exposure) |
| Response to dose reduction | Improves when antimicrobial dose is temporarily reduced | Does not improve with dose reduction |

The Evidence
What We Know (Human Data)
The Jarisch-Herxheimer reaction is a well-characterized phenomenon in spirochetal infections. A systematic review of Herxheimer reactions in Lyme disease documented the following characteristics [1]:
- Onset within 24 hours of antimicrobial initiation in most cases
- Duration typically 1-3 days, occasionally longer
- Fever is common but not universal (more common in early Lyme than in chronic)
- Cytokine profiling shows TNF-alpha elevation as the primary mediator
The distinction between Herx and flare has not been the subject of controlled trials — it is primarily a clinical framework developed through expert consensus and clinical observation. This does not make it invalid; it makes it the kind of practical knowledge that comes from years of treating these patients.
Disease flare patterns in chronic Lyme have been described in observational studies. Post-treatment Lyme disease syndrome (PTLDS) patients report symptom fluctuations triggered by exertion, stress, and environmental factors — patterns that are distinct from treatment-associated reactions [2].
What I See in Practice
In our clinical experience, the distinction between Herx and flare is usually clear when you have the full clinical picture. The cases that create confusion are:
1. Herx reactions that last longer than expected. Some patients, particularly those with high pathogen burden or impaired detoxification, experience prolonged Herx reactions lasting 2-3 weeks. These can look like a sustained worsening, which causes anxiety that treatment is making things worse.
2. Flares that coincide with treatment. A patient starts a new antibiotic on the same week they have a stressful event, poor sleep, or mold exposure. The symptom worsening is attributed to Herx when it is actually a flare triggered by the concurrent stressor.
3. Mixed presentation. In patients on active treatment, a genuine Herx reaction may be prolonged or intensified by concurrent flare triggers. The solution is to address both: manage the Herx reaction and eliminate the flare trigger.
What I tell my patients: keep a symptom diary. Document your medications (including dose changes and timing), your activity level, sleep quality, stress events, and symptom severity daily. Patterns that are invisible in the moment become clear over weeks of documentation. This is the single most valuable tool for distinguishing Herx from flare.
Practical Application
The Decision Framework
Step 1: Did you recently start, change, or increase antimicrobial therapy?
- YES + symptoms worsened within 72 hours = Likely Herx
- NO = Likely flare
Step 2: Are the symptoms familiar?
- Same symptoms you had before treatment, just louder = Supports Herx
- New or qualitatively different symptoms = Consider flare, adverse drug reaction, or new diagnosis
Step 3: Is there an identifiable non-medication trigger?
- Stress, overexertion, poor sleep, mold exposure = Supports flare
- No identifiable trigger beyond medication change = Supports Herx
Step 4: What happens when you reduce the antimicrobial dose?
- Symptoms improve within 24-48 hours = Confirms Herx (you reduced the kill rate and the die-off decreased)
- No improvement = Not Herx — investigate other causes
Managing Each Scenario
If Herx:
- Do NOT stop the antimicrobial (this means it is working)
- Reduce dose temporarily if the reaction is severe
- Implement Herx management strategies
- Inform your treating physician
- Expect improvement within 3-7 days
If Flare:
- Identify and address the trigger
- Do NOT attribute worsening to treatment and stop effective therapy
- Rest, anti-inflammatory support, hydration
- Reevaluate if the flare does not resolve within 1-2 weeks
- Consider whether the trigger reveals an untreated concurrent issue (mold, co-infection, autoimmunity)
If Uncertain:
- Document everything
- Temporarily reduce antimicrobial dose as a diagnostic maneuver
- If symptoms improve with dose reduction = Herx
- If no change = likely not Herx
- Contact your treating physician for guidance

Safety and Considerations
- Severe Herx reactions (high fever, hypotension, severe tachycardia) require urgent medical evaluation. These can occur in patients with high pathogen burden and may need IV support.
- Not all symptom worsening during treatment is Herx or flare. Adverse drug reactions (allergic reactions, organ toxicity) and new medical conditions must always be considered.
- Patients who interpret Herx as a sign that treatment is working should not seek to maximize their Herx reactions. Controlled die-off is the goal, not maximum suffering.
- Disease flares can reveal previously unrecognized triggers that deserve their own investigation and treatment.
The Bottom Line
The distinction between a Herxheimer reaction and a disease flare is one of the most important clinical judgments in chronic infection treatment. Herx reactions are treatment-triggered, self-limiting, and a sign that antimicrobials are reaching their targets. Flares are triggered by external stressors, persist until the trigger is addressed, and have no temporal relationship to medication changes. The nuance matters: getting this distinction right keeps patients on effective therapy when it is working, and prevents them from enduring unnecessary suffering when a different problem needs attention.
References
- Butler T. The Jarisch-Herxheimer reaction after antibiotic treatment of spirochetal infections: a review of recent cases and our understanding of pathogenesis. Am J Trop Med Hyg. 2017;96(1):46-52. PMID: 28077740
- Rebman AW, Bechtold KT, Yang T, et al. The clinical, symptom, and quality-of-life characterization of a well-defined group of patients with posttreatment Lyme disease syndrome. Front Med. 2017;4:224. PMID: 29312942
- Pound MW, May DB. Proposed mechanisms and preventative options of Jarisch-Herxheimer reactions. J Clin Pharm Ther. 2005;30(3):291-295. PMID: 15896244