These two organisms are grouped together not because they are closely related taxonomically, but because they share a common clinical pattern: both can establish chronic, intracellular infections that evade standard detection and treatment, producing symptoms that overlap with other chronic infections.
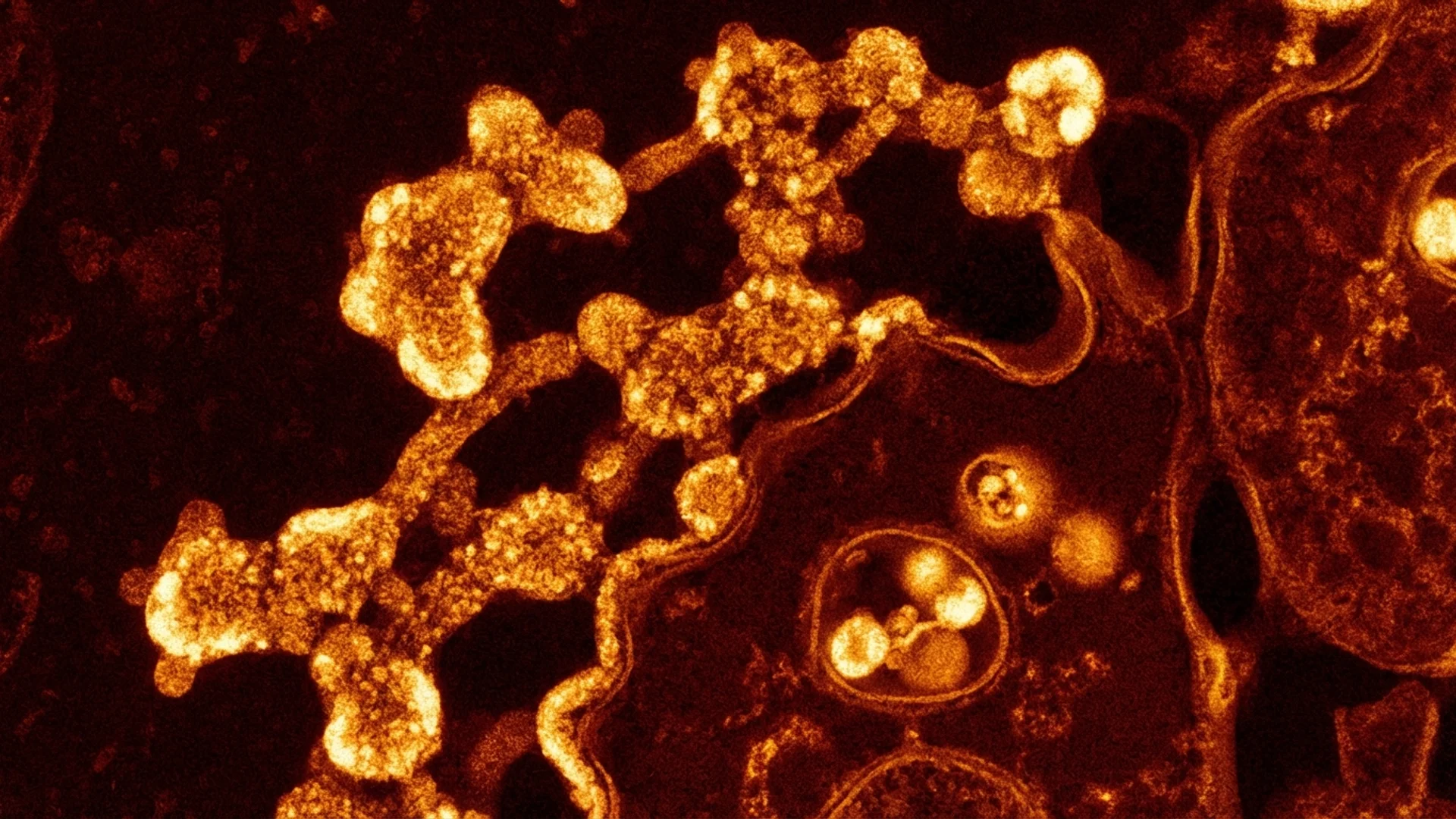
Mycoplasma
Mycoplasma species are the smallest free-living organisms — and uniquely among bacteria, they lack a cell wall. This is not an academic detail. It means that cell-wall-targeting antibiotics (penicillins, cephalosporins) are completely ineffective. A patient receiving amoxicillin for suspected Lyme disease will not treat concurrent Mycoplasma infection.

Mycoplasma pneumoniae is the species most commonly associated with chronic disease. While it is known primarily as a cause of “walking pneumonia” in younger patients, it can establish persistent infection associated with:
- Chronic fatigue
- Respiratory symptoms (chronic cough, mild dyspnea)
- Joint pain and arthritis
- Neurological symptoms (peripheral neuropathy, cognitive dysfunction)
- Skin manifestations (erythema multiforme, Stevens-Johnson syndrome in acute cases)
- Autoimmune phenomena
Other Mycoplasma species (M. fermentans, M. penetrans, M. genitalium) have been associated with chronic illness, though the evidence base is smaller.
Diagnosis
Mycoplasma pneumoniae IgG serology is commonly positive in the general population due to the frequency of prior exposure. Distinguishing past infection from active chronic infection is the diagnostic challenge. Elevated IgM suggests recent or active infection but has limited sensitivity in chronic disease. PCR from respiratory samples or blood can provide direct evidence but sensitivity varies.
In my practice, I consider the clinical context: persistent symptoms consistent with Mycoplasma, elevated IgG titers (particularly rising titers on serial testing), positive IgM, or PCR positivity — combined with clinical response to appropriate antibiotics — inform the diagnosis.
Treatment
Because Mycoplasma lacks a cell wall:
- Macrolides (azithromycin, clarithromycin) are first-line
- Tetracyclines (doxycycline, minocycline) are effective alternatives
- Fluoroquinolones (moxifloxacin) are reserved for resistant or severe cases
Treatment for chronic Mycoplasma is typically prolonged (weeks to months) and may require cycling between antibiotic classes to address intracellular persistence.
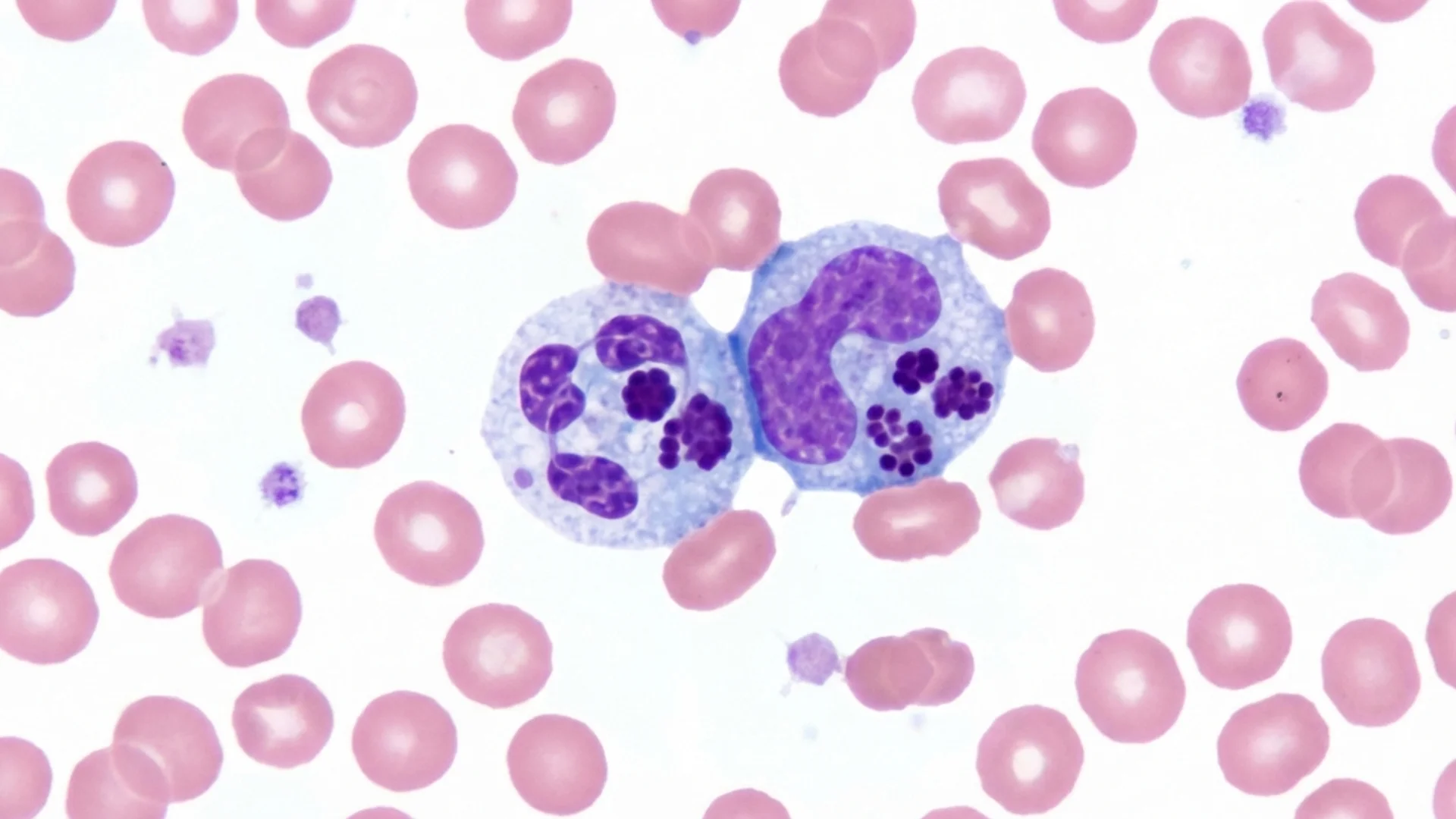
Chlamydia Pneumoniae
Chlamydia pneumoniae (Chlamydophila pneumoniae) is an obligate intracellular bacterium with a complex lifecycle that includes a metabolically inactive form (elementary body) that is resistant to antibiotics and a metabolically active form (reticulate body) that is susceptible.
This lifecycle creates a therapeutic challenge: the organism can persist in its inactive form within cells, reactivating periodically. Standard short-course antibiotic therapy may suppress active replication without eliminating the latent reservoir.
Clinical Associations
C. pneumoniae has been associated with:
- Chronic respiratory symptoms — cough, sinusitis, pharyngitis
- Atherosclerosis — C. pneumoniae DNA has been detected in atherosclerotic plaques, and its role in cardiovascular disease has been debated for decades. While large-scale antibiotic trials targeting C. pneumoniae in cardiovascular patients have been disappointing, the organism’s presence in vascular tissue suggests it may contribute to inflammation and plaque instability in some individuals.
- Chronic fatigue and cognitive dysfunction
- Asthma exacerbations
- Multiple sclerosis — epidemiological associations exist, though causation has not been established
Diagnosis
IgG serology for C. pneumoniae is positive in 60-80% of adults by age 65, reflecting the ubiquity of exposure. As with Mycoplasma, the challenge is distinguishing past exposure from clinically relevant chronic infection.
Elevated IgA antibodies are sometimes used as a marker of chronic or persistent infection, though this interpretation is debated. PCR from respiratory samples, when positive, provides stronger evidence.
Treatment
- Macrolides or tetracyclines for the active (reticulate body) form
- Extended pulsed protocols are sometimes used to target organisms as they cycle between dormant and active phases
- Rifampin may be added for intracellular penetration
The Broader Context
Both Mycoplasma and C. pneumoniae are common enough that their presence does not automatically explain a patient’s symptoms. The clinical question is whether these organisms are contributing to disease in a given patient.
In my practice, I consider these infections most seriously when:
- Symptoms are consistent with the known clinical associations
- Standard treatments have failed
- There is evidence of other chronic infections (suggesting immune compromise that allows reactivation)
- Laboratory markers support active infection (not merely past exposure)
- Clinical response to targeted antibiotics provides therapeutic confirmation
These organisms are part of the broader pattern I see in complex chronic infection: multiple pathogens, each individually manageable but collectively overwhelming when the immune system is compromised.
This content is educational and does not constitute medical advice. Diagnosis and treatment of chronic intracellular infections should be managed by a qualified physician.