At a Glance
| Property | Value |
|---|---|
| Evidence Level | Moderate (strong for hyperlipidemia, moderate for post-COVID and chronic inflammation) |
| Primary Use | Removal of LDL, fibrinogen, CRP, microclots, and inflammatory mediators |
| Key Mechanism | Heparin-induced precipitation of lipoproteins and inflammatory proteins at low pH |
| Session Duration | 2-3 hours |
| Sessions Needed | 2-5 depending on indication |
| Apheresis Types at St. Georg | 7 (H.E.L.P., TPE, Double Cascade, Evaflux a3/a5, INUSpheresis, Immunoadsorption, Leukapheresis) |
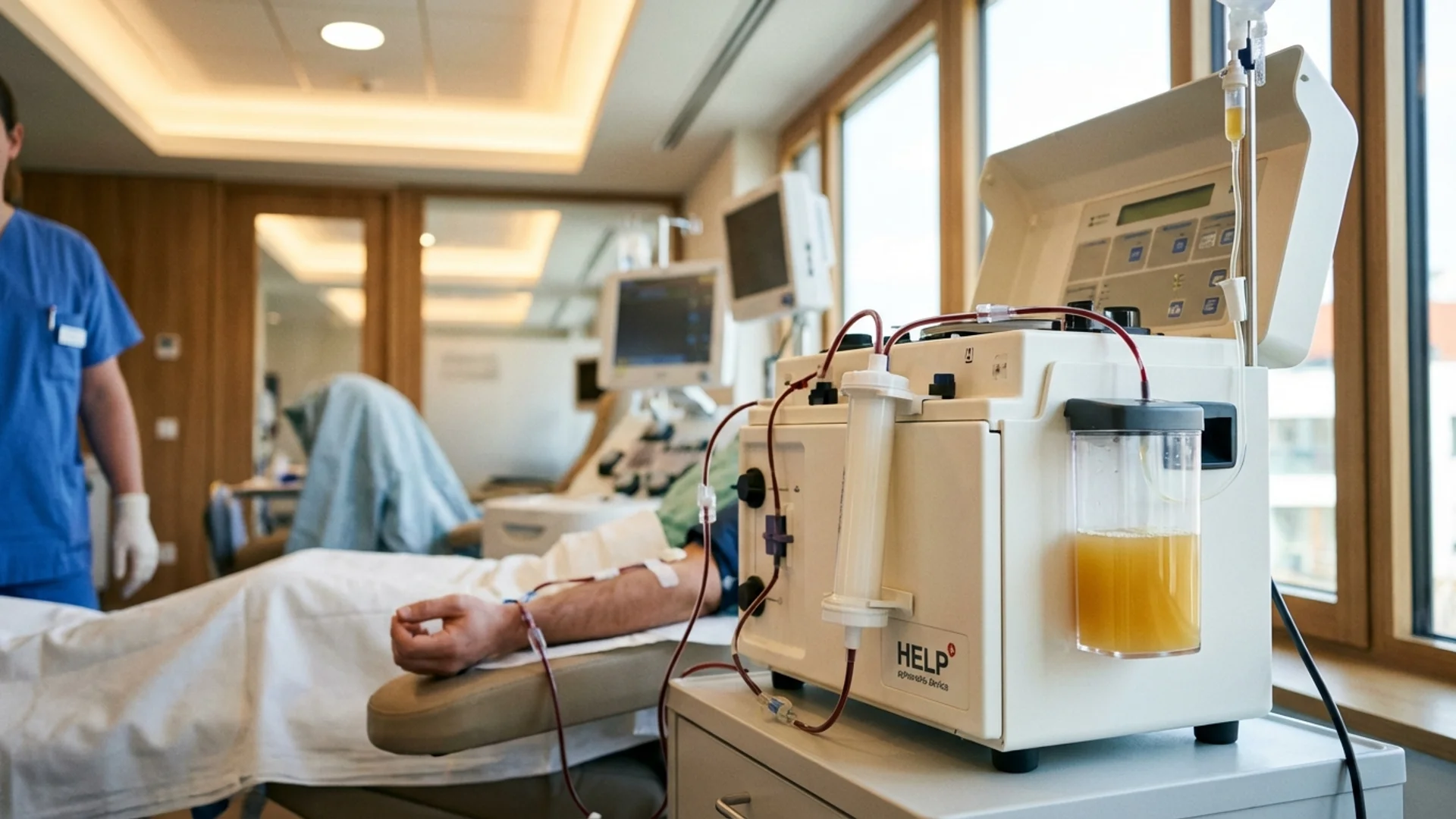
What H.E.L.P. Apheresis Actually Does
If you have been told you need apheresis, or you have been reading about it online for Long COVID or chronic Lyme disease, you probably have one question: what exactly does this machine remove from my blood, and how?
Here is what the evidence shows.
H.E.L.P. stands for Heparin-induced Extracorporeal LDL Precipitation. The name tells you the mechanism. Heparin — a natural anticoagulant — is mixed with your separated plasma at a specific low pH (approximately 5.12), causing a cascade of precipitation reactions. At this pH, several pathological substances become insoluble and physically clump together. These clumps are then captured by a polycarbonate filter and removed from your blood entirely.
What precipitates out is not limited to LDL cholesterol. The process removes:
- LDL cholesterol — including Lp(a), the genetically determined cardiovascular risk factor that no drug effectively lowers
- Fibrinogen — the precursor protein to fibrin, and the building block of the pathological microclots described in post-COVID research
- C-reactive protein (CRP) — a systemic inflammation marker that is also biologically active in promoting further inflammation
- Inflammatory lipoproteins — including oxidized LDL, which drives endothelial damage
- Complement factors — components of the immune system’s inflammatory cascade
- Immune complexes — circulating antibody-antigen aggregates that can deposit in tissues
The elegance of the system is its selectivity. Unlike plasma exchange, which replaces your entire plasma volume (including beneficial albumin, immunoglobulins, and clotting factors), H.E.L.P. apheresis targets specific classes of molecules based on their precipitation characteristics. Your albumin, essential immunoglobulins, and other protective proteins are returned to your circulation.
The Mechanism in Detail
Let me walk through exactly what happens during a session, because understanding the process removes much of the anxiety patients feel.
Step 1: Blood Separation
Blood is drawn from one arm through a venous access line. A cell separator divides your whole blood into two components: the cellular fraction (red blood cells, white blood cells, platelets) and the plasma fraction (the liquid component containing proteins, lipids, and dissolved substances). Your blood cells are never exposed to the precipitation process — they are held aside and returned to you continuously.
Step 2: Heparin Precipitation
Your separated plasma is mixed with heparin and an acetate buffer at pH 5.12. At this precise acidity, the target molecules undergo a conformational change. LDL particles, fibrinogen, CRP, and other inflammatory mediators become insoluble and form visible precipitates — essentially, they clump out of solution.
Step 3: Filtration
The precipitate-laden plasma passes through a polycarbonate filter with a defined pore size. The precipitates are trapped. The filtered plasma — now depleted of its pathological cargo — passes through.
Step 4: pH Restoration and Heparin Removal
The cleaned plasma is dialyzed against a bicarbonate buffer to restore physiological pH (7.4) and remove the excess heparin. This step is critical — returning acidic, heparin-loaded plasma would cause immediate adverse effects.
Step 5: Reconstitution and Return
The pH-corrected plasma is recombined with your cellular blood components and returned to your other arm through a second venous line. The entire circuit is continuous — blood is being drawn, processed, and returned simultaneously.
The whole process takes 2-3 hours. Most patients read, work on their laptop, or sleep through it.

What the Filtrate Looks Like
I mention this because it matters to patients. When the precipitation filter is examined after a session, you can see the captured material — a yellowish-white mass of precipitated lipoproteins, fibrinogen, and inflammatory proteins. In patients with significant microclot burden (particularly post-COVID patients), the filtrate can appear noticeably more dense and discolored than what you see in a healthy control.
This is not theater. It is physical evidence of what was circulating in the patient’s blood. Many patients find it both disturbing (that was inside me?) and reassuring (it is no longer inside me). In my clinical experience, this tangible evidence also helps patients understand why they feel different after treatment — sometimes within hours.
The Evidence Base
Let me be direct about where the evidence stands for different indications.
Strong Evidence: Familial Hypercholesterolemia and Lp(a)
H.E.L.P. apheresis was originally developed and FDA-approved for treatment-resistant hyperlipidemia, particularly familial hypercholesterolemia and elevated Lp(a). Multiple randomized controlled trials and long-term outcome studies demonstrate that regular H.E.L.P. apheresis:
- Reduces LDL cholesterol by 55-70% per session [1]
- Reduces Lp(a) by 60-70% per session [2]
- Reduces fibrinogen by 50-60% per session
- Reduces cardiovascular event rates in patients who cannot achieve target lipid levels with medications alone [3]
This is Level 1 evidence. The procedure is covered by major insurance systems in Germany for these indications.
Moderate Evidence: Post-COVID Syndrome
The application of H.E.L.P. apheresis to post-COVID syndrome is based on sound mechanistic reasoning and growing clinical data. The logic follows directly from the microclot hypothesis advanced by Pretorius, Kell, and others: if fibrin amyloid microclots are driving symptoms, then removing fibrinogen (the precursor) and the microclots themselves should provide relief.
Published observational studies and case series report:
- Significant reduction in fatigue scores following 2-4 sessions [4]
- Improvement in cognitive function measures
- Reduction in inflammatory markers (CRP, fibrinogen, IL-6)
- Subjective improvement in exercise tolerance
A 2023 study published in Molecular Psychiatry provided important mechanistic support, demonstrating that post-COVID patients have measurably impaired microcirculation and that interventions targeting microclots improve perfusion parameters [5].
I want to be calibrated here. We do not yet have large, randomized, placebo-controlled trials for apheresis in post-COVID. The evidence is moderate — consistent observational data with strong mechanistic plausibility. What I see in practice aligns with the published data: most patients experience meaningful improvement. Not all, and not always permanent after a single course, but meaningful.
Clinical Observation: Chronic Lyme and Tick-Borne Disease
In chronic tick-borne disease, I use H.E.L.P. apheresis as an adjunct to antimicrobial treatment and hyperthermia. The rationale is reduction of inflammatory burden and immune complexes that accumulate during chronic infection and intensify during treatment-induced Herxheimer reactions.
This is primarily based on clinical observation and mechanistic reasoning. In our experience treating over 12,000 Lyme patients since 1994, the addition of apheresis between hyperthermia sessions reduces the severity of Herxheimer reactions and accelerates recovery. I classify this as clinical observation, not established evidence.

How Many Sessions Are Needed
This depends entirely on the indication and the individual patient’s response.
Post-COVID syndrome: I typically recommend 2-4 H.E.L.P. apheresis sessions, interleaved with moderate whole-body hyperthermia (~40 degrees C). The combination addresses both the microclot/inflammatory component (apheresis) and the immune dysregulation/viral persistence component (hyperthermia). Some patients respond well to 2 sessions; others need 4 or more.
Chronic Lyme treatment protocol: Apheresis sessions are integrated into the broader treatment program, typically 1-2 sessions between hyperthermia treatments. The number depends on the intensity of the patient’s inflammatory response.
Cardiovascular prevention (Lp(a), familial hypercholesterolemia): This is ongoing, typically every 1-2 weeks, because the underlying genetic condition continuously regenerates the pathological lipoproteins.
What I tell my patients: Apheresis is not a one-time cure. It is a mechanical reduction of pathological substances. If the underlying condition continues to produce those substances (as in genetic hyperlipidemia or ongoing chronic infection), the treatment may need to be repeated. The goal is to reduce the burden enough that your body’s own systems can manage the remainder.
The Seven Apheresis Modalities at Klinik St. Georg
One of the things that distinguishes our hospital is that we do not rely on a single apheresis technique. We operate seven distinct modalities, each with specific strengths:
-
H.E.L.P. Apheresis — Selective precipitation of LDL, Lp(a), fibrinogen, CRP. Primary choice for post-COVID and cardiovascular prevention.
-
Therapeutic Plasma Exchange (TPE) — Full plasma replacement. Reserved for severe autoimmune presentations or acute crises where broad removal is needed.
-
Double Cascade Filtration — Two-stage membrane filtration that separates plasma components by molecular weight. More selective than TPE, removing large molecules (autoantibodies, immune complexes) while retaining albumin.
-
Evaflux a3/a5 — Column-based immunoadsorption using tryptophan-linked polyvinyl alcohol. Selectively removes immunoglobulins. Particularly useful when autoantibodies are the primary target.
-
INUSpheresis — A membrane-based apheresis system that targets environmental toxins, heavy metals, and inflammatory mediators alongside lipoproteins. Used in patients with combined toxic and inflammatory burdens.
-
Immunoadsorption — Protein A or anti-IgG column-based removal of specific immunoglobulin classes. Precise targeting of autoantibodies without plasma loss.
-
Leukapheresis — Selective removal of white blood cells. Used when pathological leukocyte populations (e.g., activated autoreactive lymphocytes) are contributing to disease.
The choice of modality depends on the specific pathology we are targeting. A post-COVID patient with significant microclot burden gets H.E.L.P. apheresis. A patient with autoantibody-driven neurological symptoms might receive immunoadsorption. A patient with combined environmental toxin exposure and chronic inflammation might benefit from INUSpheresis. This is individualized medicine — not one-size-fits-all.
Safety Profile
H.E.L.P. apheresis has a well-established safety record over decades of clinical use. Common but manageable effects include:
- Transient hypotension — Blood volume shifts during the extracorporeal circuit can cause temporary drops in blood pressure. This is managed with fluid replacement and is rarely significant.
- Venous access site discomfort — Some bruising or soreness at the needle insertion sites. Standard venipuncture complications.
- Transient fatigue — Some patients feel mildly tired on the day of treatment, followed by improved energy the next day.
- Allergic reactions — Rare, but possible with any extracorporeal blood contact procedure.
Serious adverse events are uncommon. The procedure has been performed millions of times globally for lipid indications with an excellent safety record.
Contraindications include severe coagulation disorders, active bleeding, heparin-induced thrombocytopenia (HIT), and hemodynamic instability. Patients on ACE inhibitors require specific management due to potential bradykinin-related reactions during extracorporeal procedures.
What Patients Should Know Before Treatment
If you are considering H.E.L.P. apheresis, here is what I want you to understand:
It is not a detox trend. This is a medical procedure with decades of clinical data, originally developed for a serious cardiovascular condition. Its application to post-COVID and chronic infections is an evidence-based extension of that technology, not a wellness fad.
Results are not always immediate. Some patients feel noticeably better within 24-48 hours. Others improve gradually over days to weeks as the reduced inflammatory burden allows tissue repair. A minority do not respond meaningfully, which may indicate that their symptoms are driven by mechanisms other than the ones apheresis targets.
It works best as part of a comprehensive protocol. In my clinical experience, apheresis alone rarely resolves complex conditions like post-COVID or chronic Lyme disease. It is most effective when combined with targeted antimicrobial treatment, hyperthermia, immune modulation, and other therapies selected for the individual patient.
The procedure itself is well-tolerated. Most patients are surprised by how undramatic it is. You sit in a comfortable chair. Two IV lines are placed. The machine runs. You read or rest. After 2-3 hours, the lines are removed and you walk out.
The Bottom Line
H.E.L.P. apheresis is a selective extracorporeal blood filtration technique that removes LDL, fibrinogen, CRP, and inflammatory mediators through heparin-induced precipitation at controlled pH. It has strong evidence for cardiovascular indications and moderate but growing evidence for post-COVID syndrome and chronic inflammatory conditions. At Klinik St. Georg, it is one of seven apheresis modalities we deploy based on the individual patient’s pathology — because no single filtration technique addresses every clinical scenario.
The nuance matters. Apheresis is a powerful tool, but it is a tool — not a cure in isolation. It removes what should not be there. The rest of the treatment program addresses why it was there in the first place.
References
- Jaeger BR, Richter Y, Nagel D, et al. Longitudinal cohort study on the effectiveness of lipid apheresis treatment to reduce high lipoprotein(a) levels and prevent major adverse coronary events. Nat Clin Pract Cardiovasc Med. 2009;6(3):229-239.
- Leebmann J, Roeseler E, Julius U, et al. Lipoprotein apheresis in patients with maximally tolerated lipid-lowering therapy, lipoprotein(a)-hyperlipoproteinemia, and progressive cardiovascular disease. Circulation. 2013;128(24):2567-2576.
- Heigl F, Hettich R, Lotz N, et al. Efficacy, safety, and tolerability of long-term lipoprotein apheresis in patients with LDL- or Lp(a)-hyperlipoproteinemia. Atheroscler Suppl. 2015;18:154-162.
- Bornstein SR, Voit-Bak K, Donate T, et al. Chronic post-COVID-19 syndrome and chronic fatigue syndrome: Is there a role for extracorporeal apheresis? Mol Psychiatry. 2022;27(1):34-37.
- Pretorius E, Vlok M, Venter C, et al. Persistent clotting protein pathology in Long COVID/Post-Acute Sequelae of COVID-19 (PASC) is accompanied by increased levels of antiplasmin. Cardiovasc Diabetol. 2021;20(1):172.
- Kell DB, Laubscher GJ, Pretorius E. A central role for amyloid fibrin microclots in long COVID/PASC: origins and therapeutic implications. Biochem J. 2022;479(4):537-559.