Every patient I see with chronic inflammation, autonomic dysfunction, or treatment-resistant depression has one thing in common: their parasympathetic nervous system is underperforming. The vagus nerve is the master switch of that system — the longest cranial nerve in the body, running from the brainstem to the colon, touching nearly every organ along the way. Understanding how to measure its function and how to activate it is fundamental to managing chronic disease.
Here is what the research actually says, what works, and what is still speculative.
At a Glance
| Property | Detail |
|---|---|
| Evidence Level | Strong (implanted VNS for epilepsy, depression); Moderate (non-invasive VNS for inflammation, headache); Emerging (transcutaneous auricular VNS for broader applications) |
| Primary Use | Epilepsy, treatment-resistant depression, inflammation modulation, autonomic regulation |
| Key Mechanism | Afferent signaling to nucleus tractus solitarius, activating parasympathetic pathways and the cholinergic anti-inflammatory pathway |
| Biomarker | Heart rate variability (HRV), specifically the high-frequency component and RMSSD |
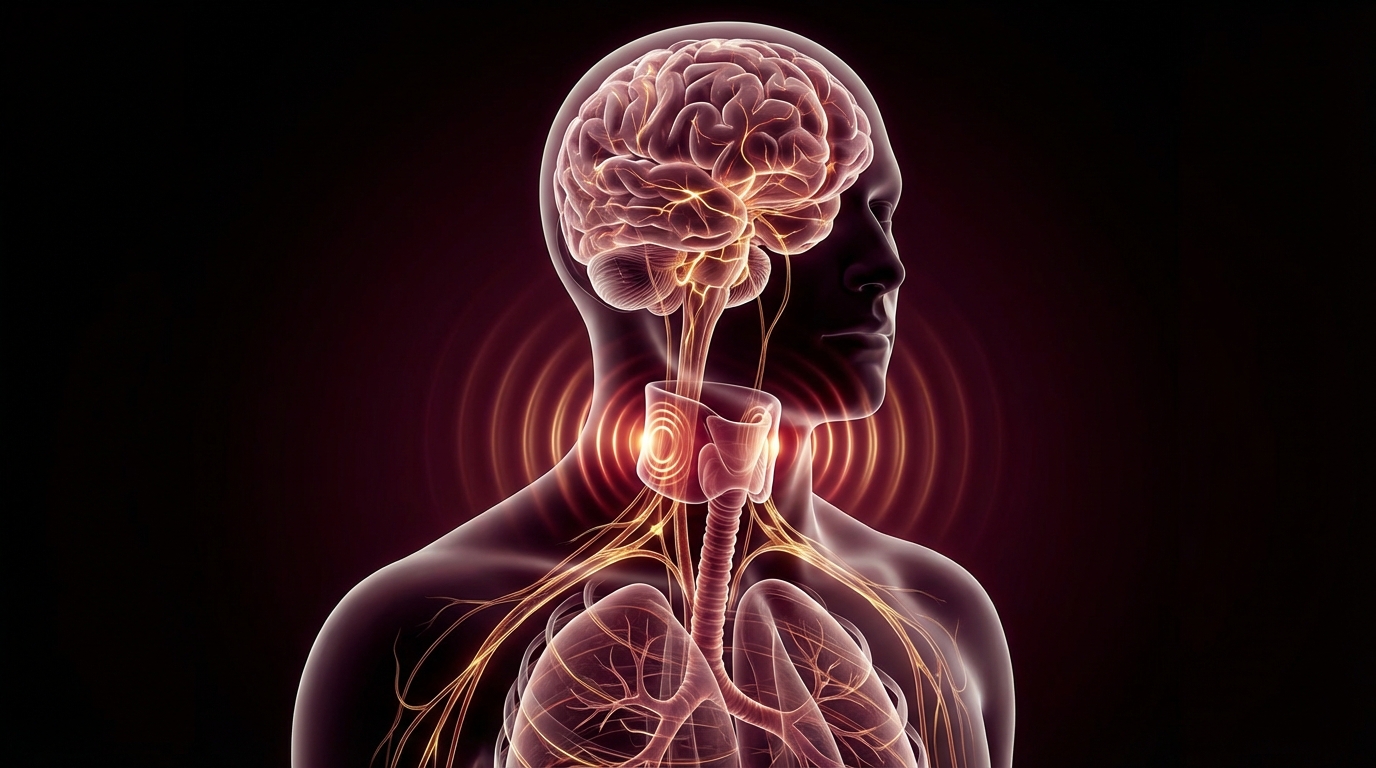
The Vagus Nerve: Anatomy That Matters
The vagus nerve — cranial nerve X — is not a single nerve. It is a complex, bilateral structure containing approximately 80% afferent (sensory) fibers carrying information from the body to the brain, and 20% efferent (motor) fibers carrying instructions from the brain to the body.
It originates in the medulla oblongata at the brainstem and descends through the neck, thorax, and abdomen, innervating:
- Heart: Slows heart rate via the sinoatrial node
- Lungs: Regulates bronchial tone and respiratory rate
- Gut: Controls motility, secretion, and the gut-brain axis from esophagus to transverse colon
- Liver, pancreas, spleen: Modulates metabolic and immune function
- Larynx and pharynx: Controls swallowing and voice
The term “vagal tone” refers to the baseline level of vagus nerve activity. High vagal tone is associated with lower resting heart rate, better emotional regulation, reduced inflammation, and improved digestive function. Low vagal tone is a consistent finding in chronic inflammatory conditions, depression, anxiety disorders, IBS, and post-COVID autonomic dysfunction.
The Cholinergic Anti-Inflammatory Pathway
This is the mechanism that makes vagal stimulation clinically relevant beyond neurology. In 2000, Kevin Tracey and colleagues at the Feinstein Institutes identified what they termed the “inflammatory reflex” — a neural circuit through which the vagus nerve detects and suppresses systemic inflammation.
The pathway works as follows:
- Afferent vagal fibers detect inflammatory signals (cytokines, pathogen-associated molecular patterns) in the periphery
- This information is relayed to the brainstem
- Efferent vagal fibers signal to the spleen via the splenic nerve
- Acetylcholine released by T-cells in the spleen binds to alpha-7 nicotinic receptors on macrophages
- This suppresses the production of TNF-alpha, IL-1, IL-6, and other pro-inflammatory cytokines
This is not speculative. Tracey’s group demonstrated in animal models that direct electrical stimulation of the vagus nerve could suppress lethal doses of endotoxin. Subsequent human studies with implanted VNS devices have shown measurable reductions in inflammatory markers in rheumatoid arthritis patients.
In my clinical experience, this mechanism is directly relevant to every chronic inflammatory condition I treat — from Lyme disease to post-COVID to autoimmune disorders. The vagus nerve is not just about calming the mind. It is a hard-wired inflammation control system.
Vagus Nerve Stimulation: The Methods
Implanted VNS (Invasive)
Implanted VNS involves surgically placing a small pulse generator (similar to a cardiac pacemaker) under the skin of the chest, with an electrode wrapped around the left cervical vagus nerve. The device delivers regular electrical pulses to the nerve.
Epilepsy. Implanted VNS was FDA-approved for drug-resistant epilepsy in 1997. Multiple RCTs and long-term follow-up studies demonstrate seizure reduction of 50% or more in approximately 50% of patients. The evidence is strong. A Cochrane review by Panebianco et al. (2015) confirmed efficacy, noting that benefits tend to increase over time — patients often show continued improvement at 2-3 years compared to initial activation.
Treatment-Resistant Depression. VNS received FDA approval for treatment-resistant depression in 2005 based on long-term open-label data showing sustained response rates. The evidence is more nuanced here — the pivotal randomized trial did not meet its primary endpoint at 10 weeks, but long-term data at 1-2 years showed significant benefit compared to treatment as usual. This suggests VNS for depression works through gradual neuroplastic changes rather than acute effects.
Non-Invasive VNS (nVNS)
Non-invasive approaches stimulate branches of the vagus nerve through the skin, avoiding surgery entirely.
gammaCore (Cervical nVNS). This handheld device stimulates the cervical vagus nerve through the skin of the neck. It is FDA-cleared for cluster headache and migraine. The evidence for headache is moderate — RCTs show benefit, though effect sizes are smaller than for invasive VNS in epilepsy.
Transcutaneous Auricular VNS (taVNS). The ear contains a branch of the vagus nerve — the auricular branch (Arnold’s nerve) — that can be stimulated with a small clip electrode on the tragus or cymba conchae. This is the most accessible form of VNS and the subject of rapidly growing research.
Studies by Stavrakis et al. (2020) have demonstrated that taVNS can reduce atrial fibrillation burden, suppress inflammatory cytokines, and improve autonomic balance in human subjects. The evidence is moderate and growing. Multiple RCTs are underway for depression, inflammation, and post-COVID autonomic dysfunction.
NEMOS (Cerbomed). A CE-marked taVNS device approved in Europe for epilepsy and depression. The device stimulates the auricular branch of the vagus nerve via an ear electrode.
Physiological Vagal Activation
Not all vagal stimulation requires a device. Several physiological interventions reliably activate the vagus nerve:
Cold exposure. Immersing the face in cold water triggers the mammalian dive reflex — a powerful vagal response that slows heart rate and redirects blood flow to vital organs. Cold showers, ice baths, and cold-water face immersion all activate this pathway. The evidence for acute parasympathetic activation from cold exposure is well-established in physiology literature. What remains less clear is whether chronic cold exposure training produces lasting improvements in vagal tone.
In my clinical practice, I recommend cold exposure as an adjunct — not as a standalone treatment for serious conditions, but as a daily practice that supports autonomic regulation. Starting with 30 seconds of cold water at the end of a shower and gradually building tolerance is a reasonable approach for most patients.
Breathwork. Slow, deep breathing with an extended exhale (e.g., 4-count inhale, 7-count exhale) stimulates the vagus nerve through baroreceptor activation and respiratory sinus arrhythmia. This is the physiological basis for why deep breathing reduces heart rate and promotes calm — it is vagal activation, not placebo.
Gargling and singing. The vagus nerve innervates the muscles of the pharynx and larynx. Vigorous gargling and sustained vocalization (humming, singing, chanting) activate these muscles and, by extension, the vagus nerve. The evidence here is mechanistic and clinical observation rather than RCT-level.
Measuring Vagal Tone: Heart Rate Variability
Heart rate variability (HRV) is the most accessible and well-validated biomarker for vagal tone. It measures the variation in time intervals between consecutive heartbeats. A healthy heart does not beat like a metronome — it varies beat to beat in response to autonomic input.
High HRV indicates strong parasympathetic (vagal) input and is associated with better cardiovascular health, emotional regulation, stress resilience, and lower inflammation.
Low HRV indicates sympathetic dominance and is a consistent finding in chronic disease, depression, anxiety, post-COVID dysautonomia, and chronic fatigue.
Key HRV Metrics
- RMSSD (Root Mean Square of Successive Differences): The most commonly used time-domain measure of vagal tone. Higher values indicate better parasympathetic function.
- High-Frequency Power (HF, 0.15-0.4 Hz): The frequency-domain measure most closely associated with vagal activity.
- LF/HF Ratio: Traditionally interpreted as sympathovagal balance, though this interpretation has been debated in recent literature.
How to Track HRV
Consumer-grade devices (Oura Ring, WHOOP, Apple Watch, Garmin) now provide reasonably accurate HRV measurements. For clinical purposes, I recommend:
- Measure at the same time daily (morning, upon waking, is most consistent)
- Track trends over weeks, not individual readings
- Use RMSSD as the primary metric
- Expect HRV to decrease with illness, stress, alcohol, and poor sleep
- Expect HRV to increase with regular exercise, quality sleep, and vagal training
What I tell my patients: HRV is not a diagnostic test. It is a directional biomarker. If your HRV is trending up over weeks of treatment, your autonomic nervous system is moving in the right direction. If it is flat or declining, we need to investigate why.
The Evidence: Clinical Applications
Strong Evidence
- Epilepsy (implanted VNS): Cochrane-reviewed, FDA-approved, long-term data supporting sustained seizure reduction
- Treatment-resistant depression (implanted VNS): FDA-approved, long-term response rates of 50%+ at 2 years
Moderate Evidence
- Cluster headache and migraine (gammaCore): FDA-cleared, RCT-supported
- Rheumatoid arthritis (implanted VNS): Koopman et al. (2016) demonstrated significant reduction in TNF production and clinical disease activity in RA patients with implanted VNS
- Atrial fibrillation (taVNS): RCT data showing reduced AF burden
Emerging Evidence
- Post-COVID autonomic dysfunction: Multiple ongoing trials with taVNS
- Inflammatory bowel disease: Preclinical and early clinical data
- Chronic fatigue syndrome: Mechanistically rational, clinical observation supporting benefit, awaiting controlled trials
- PTSD: RCT data showing benefit of taVNS, replication needed
Safety and Considerations
Implanted VNS
The most common side effects are hoarseness, cough, and throat discomfort during stimulation — these occur because the vagus nerve innervates the larynx. These effects are typically manageable by adjusting stimulation parameters. Surgical risks include infection, nerve damage, and device-related complications, though serious adverse events are uncommon.
Non-Invasive VNS
The safety profile of taVNS and cervical nVNS is excellent. Reported side effects include mild tingling, redness at the electrode site, and occasional dizziness. No serious adverse events have been consistently reported in clinical trials.
Contraindications
- Active implanted cardiac devices (for VNS devices — potential interference)
- Carotid atherosclerosis (for cervical nVNS — theoretical concern)
- Pregnancy (insufficient data for device-based VNS)
Practical Application
For patients interested in vagal activation, I suggest a layered approach:
Foundation (everyone):
- Daily breathwork practice: 5-10 minutes of slow breathing with extended exhale
- Cold exposure: 30-60 seconds of cold water at end of shower, building gradually
- Regular aerobic exercise: the single strongest driver of long-term HRV improvement
- Track HRV with a wearable device to establish baseline and monitor progress
Clinical level (with physician guidance):
- taVNS devices for patients with documented low vagal tone and relevant clinical conditions
- Consider implanted VNS referral for drug-resistant epilepsy or treatment-resistant depression after adequate medication and psychotherapy trials
At our hospital:
- We incorporate vagal tone assessment into our evaluation of chronic inflammatory conditions, post-COVID, and chronic fatigue
- TPS (Transcranial Pulse Stimulation) addresses central neurological components that VNS alone may not reach — these modalities are complementary
- HRV monitoring is part of our treatment response assessment
The Bottom Line
The vagus nerve is the body’s built-in inflammation control and stress recovery system. Vagal stimulation — whether through implanted devices, non-invasive stimulators, or physiological practices like cold exposure and breathwork — has real clinical evidence for epilepsy, depression, and inflammatory conditions. HRV is your best accessible biomarker for tracking vagal tone over time.
The nuance matters: vagal stimulation is not a cure for chronic disease. It is a tool for shifting the autonomic nervous system from a state of chronic sympathetic dominance toward parasympathetic recovery. For many of my patients, that shift is a critical piece of their treatment puzzle.
References
-
Tracey KJ. The inflammatory reflex. Nature. 2002;420(6917):853-859. PMID: 12490958.
-
Panebianco M, Rigby A, Weston J, Marson AG. Vagus nerve stimulation for partial seizures. Cochrane Database Syst Rev. 2015;(4):CD002896. PMID: 25835947.
-
Koopman FA, Chavan SS, Miljko S, et al. Vagus nerve stimulation inhibits cytokine production and attenuates disease severity in rheumatoid arthritis. Proc Natl Acad Sci USA. 2016;113(29):8284-8289. PMID: 27382171.
-
Stavrakis S, Stoner JA, Humphrey MB, et al. TREAT AF (Transcutaneous Electrical Vagus Nerve Stimulation to Suppress Atrial Fibrillation): a randomized clinical trial. JACC Clin Electrophysiol. 2020;6(3):282-291. PMID: 32192678.
-
Bonaz B, Sinniger V, Pellissier S. Vagus nerve stimulation at the interface of brain-gut interactions. Cold Spring Harb Perspect Med. 2019;9(8):a034199. PMID: 30201788.
Disclaimer: This article is for educational purposes. Vagus nerve stimulation devices are medical interventions that should be discussed with a qualified physician. This content does not constitute medical advice for your individual situation.