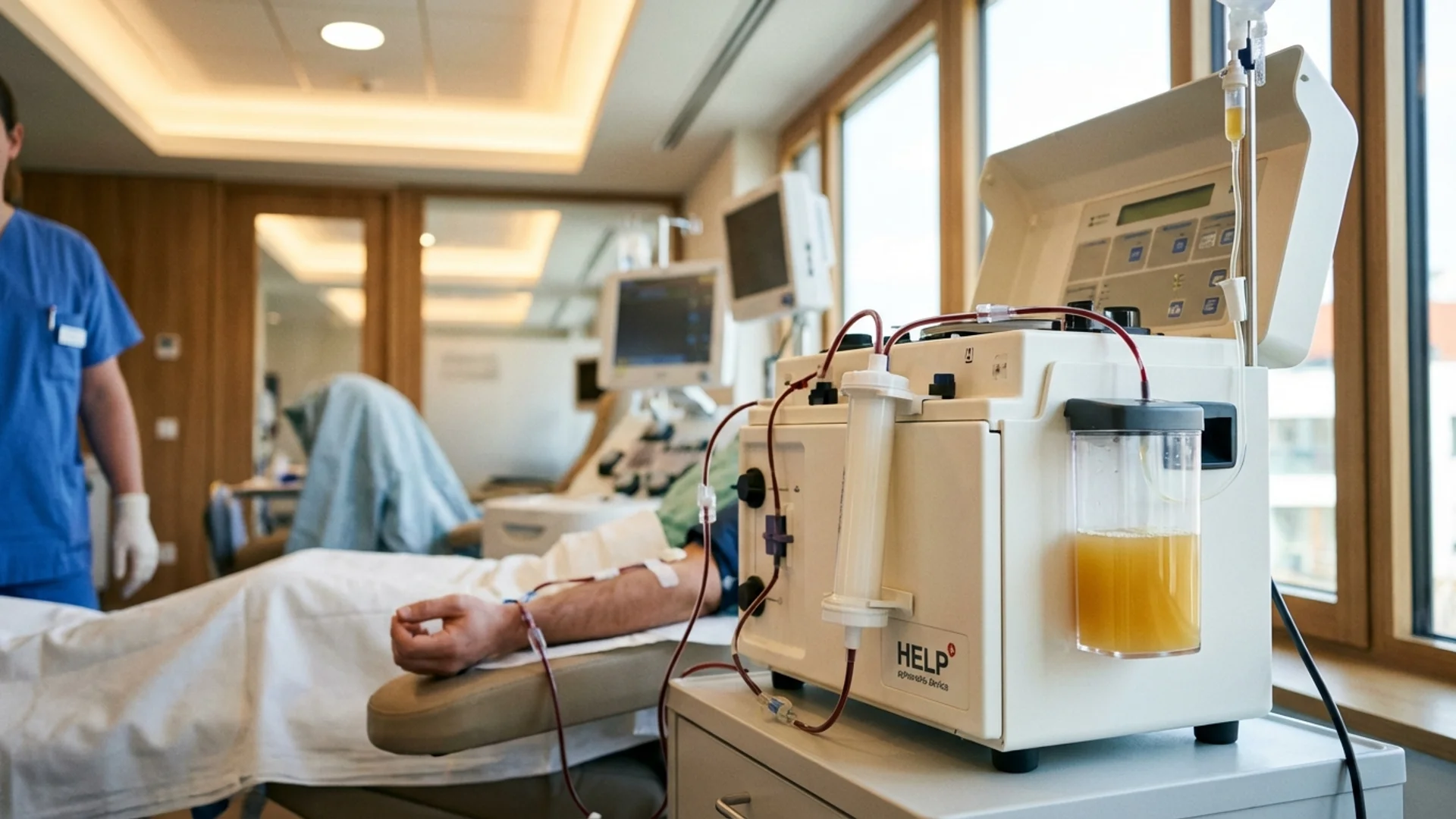
Apheresis — from the Greek aphaeresis, “to take away” — refers to the selective removal of specific blood components through extracorporeal filtration. In the context of chronic infection and post-COVID treatment, apheresis serves a fundamentally different purpose than it does in its traditional applications (plasmapheresis for autoimmune diseases, platelet donation, etc.). Here, it is used to physically remove the inflammatory mediators, autoantibodies, microclots, and pathological proteins that drive chronic symptoms.
The rationale is straightforward: when the body is producing or retaining pathological substances faster than it can clear them, mechanical removal provides immediate relief and creates space for the body’s own repair mechanisms to function.
Types of Apheresis Relevant to Chronic Infection
HELP Apheresis (Heparin-induced Extracorporeal LDL Precipitation)
Originally developed for severe hyperlipidemia, HELP apheresis has been adapted for post-COVID and chronic inflammatory conditions. It removes:

- Fibrinogen (the precursor to fibrin microclots)
- LDL cholesterol
- C-reactive protein
- Inflammatory lipoproteins
In the context of post-COVID, HELP apheresis directly addresses the fibrin amyloid microclot pathology described in my microclot article by removing the fibrinogen that forms these pathological clots.
Immunoadsorption
Immunoadsorption selectively removes immunoglobulins (antibodies) from the patient’s plasma. In post-COVID and chronic infection, this is relevant for:
- Removing autoantibodies that may be driving autoimmune-mediated symptoms
- Reducing immune complex burden
- Modulating the overall immunoglobulin profile
Plasma Exchange (Plasmapheresis)
The most extensive form of apheresis — replacing the patient’s plasma with donor plasma or albumin solution. This removes all plasma-phase pathological substances but also removes beneficial proteins. It is reserved for severe cases.
Double Filtration Plasmapheresis (DFPP)
A more selective approach that separates plasma components by molecular size, allowing removal of larger molecules (including autoantibodies and inflammatory mediators) while retaining smaller essential proteins (albumin, smaller immunoglobulins).
Clinical Applications
Post-COVID Syndrome
Apheresis has generated significant interest as a treatment for post-COVID, particularly in Germany where several clinics have adopted it. The rationale is compelling:
- Removal of fibrinogen reduces microclot formation
- Removal of inflammatory mediators (CRP, cytokines, complement components) reduces the inflammatory burden
- Removal of autoantibodies addresses autoimmune-mediated symptoms
- Removal of spike protein (where persistent) eliminates the ongoing viral antigen stimulus
Published case series and observational studies have reported improvements in fatigue, cognitive function, and exercise tolerance following apheresis treatment in post-COVID patients [1].
I want to be transparent about the evidence level. We do not yet have large, randomized controlled trials of apheresis for post-COVID. The published data consists of case series, observational cohorts, and individual case reports. The clinical responses I have observed in my practice are consistent with the published reports — many patients experience meaningful improvement — but this does not constitute Level 1 evidence.
Chronic Lyme Disease and Co-Infections
In chronic tick-borne disease, apheresis can serve as an adjunct to antimicrobial therapy by:
- Reducing the inflammatory cytokine burden
- Removing immune complexes that contribute to joint and tissue inflammation
- Supporting detoxification during intensive treatment phases (reducing the Herxheimer reaction burden)
- Removing autoantibodies that may develop through molecular mimicry
I use apheresis selectively in Lyme patients — typically those with high inflammatory burden, significant autoimmune features, or severe Herxheimer reactions during treatment.
What Patients Experience
A typical apheresis session lasts two to four hours. The patient is connected to the apheresis machine via peripheral IV access (occasionally central access is needed). Blood is drawn, processed through the filtration system, and returned to the patient.
Patients often report feeling an improvement in mental clarity and energy within hours of the procedure — sometimes during the session itself. This immediate effect is consistent with the removal of inflammatory mediators that were directly impairing organ function.
The duration of improvement varies. Some patients experience sustained benefit from a series of three to five sessions. Others require periodic maintenance sessions.
Side Effects
Apheresis is generally well-tolerated. Potential side effects include:
- Hypotension during the procedure (managed with fluid administration)
- Citrate-related symptoms (tingling, cramping from the anticoagulant used in the circuit) — managed with calcium supplementation
- Fatigue immediately after the procedure
- Vasovagal reactions
- Rare: infection at the access site, allergic reaction
Serious complications are uncommon in experienced centers.
My Clinical Perspective
In my practice, apheresis is not a standalone therapy. It is a powerful adjunct within a comprehensive treatment program. Its value lies in its ability to produce rapid improvement in patients whose inflammatory burden is too high for other interventions to gain traction.
I think of apheresis as analogous to dialysis in kidney failure — it does mechanically what the body’s own systems currently cannot do efficiently. But just as dialysis does not treat the underlying kidney disease, apheresis does not address the root cause of the inflammation or infection. It creates a window of improved function during which other therapies — antimicrobials, immune modulation, mitochondrial support — can work more effectively.
The patients who benefit most from apheresis in my experience are:
- Post-COVID patients with evidence of significant microclot pathology and endothelial dysfunction
- Chronic infection patients with high inflammatory markers and autoimmune features
- Patients experiencing severe Herxheimer reactions during antimicrobial treatment
- Patients who have not responded adequately to conventional approaches
The Honest Limitations
- Apheresis is expensive and not universally covered by insurance
- The evidence base, while growing, consists primarily of observational data
- Not all patients respond, and the predictors of response are not fully defined
- The procedure requires specialized equipment and trained staff
- Benefits may be temporary without concurrent treatment of the underlying condition
The Bottom Line
Apheresis represents a logical and clinically useful tool for reducing the inflammatory and pathological burden in chronic infection and post-COVID patients. It is most effective when integrated into a comprehensive treatment program rather than used in isolation. The evidence is observational but consistent, and the clinical responses I have observed are compelling enough to make it a regular component of our treatment offerings.
As controlled trial data emerges, I expect the indications and protocols to become more refined. For now, apheresis occupies a position of reasonable clinical utility supported by mechanistic rationale and accumulating observational evidence.

References
- Jaeger BR, et al. Immunoadsorption and HELP Apheresis in Post-COVID Syndrome. Atherosclerosis Supplements. 2022;49:S24.
This content is educational and does not constitute medical advice. Apheresis should be performed at qualified medical facilities with appropriate equipment and trained staff.