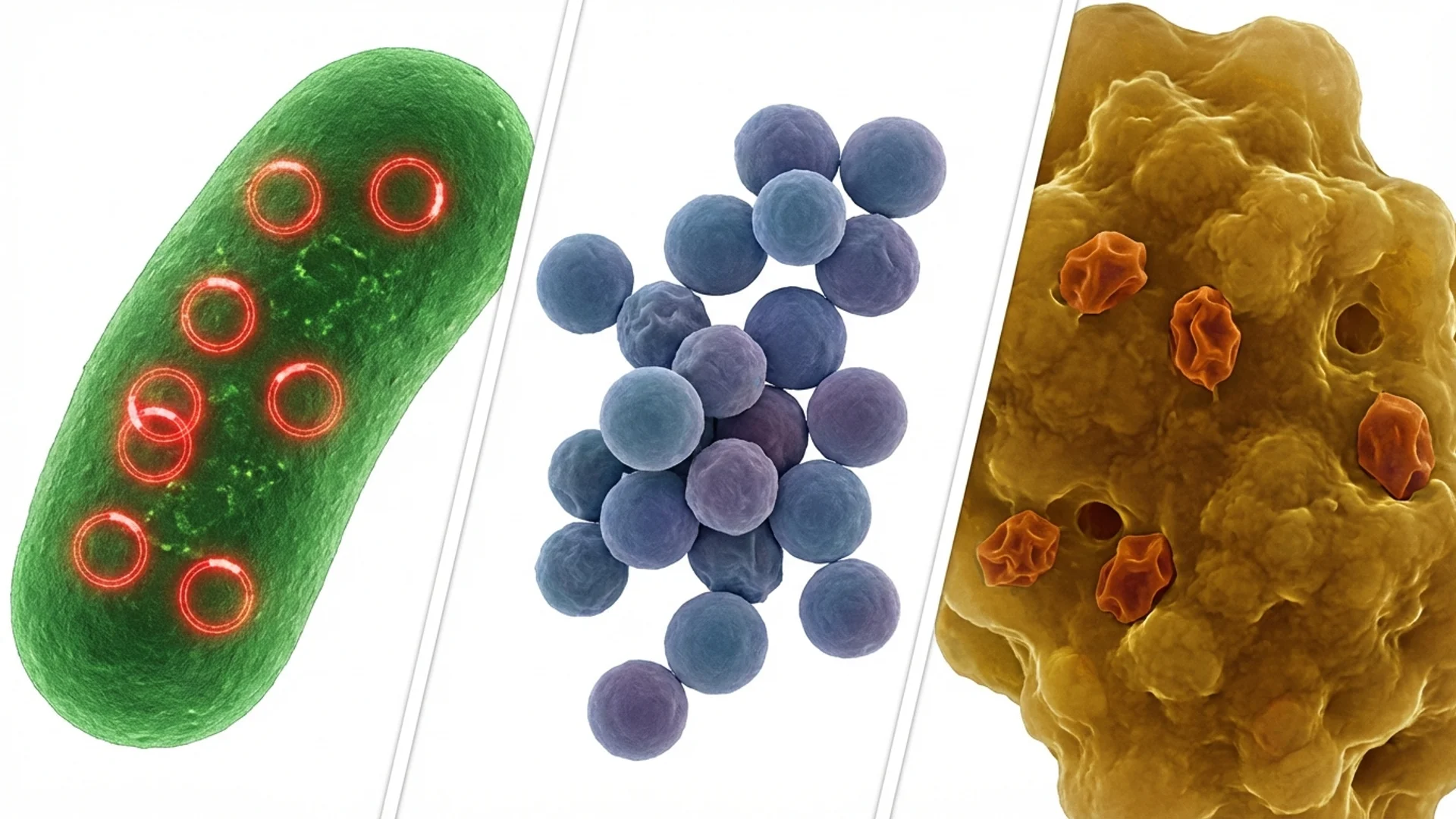
The era of reliable, universal antibiotic efficacy is ending. The World Health Organization has identified antimicrobial resistance as one of the top 10 global public health threats. For patients with chronic infections, this is not an abstract policy concern — it directly affects treatment options and outcomes.
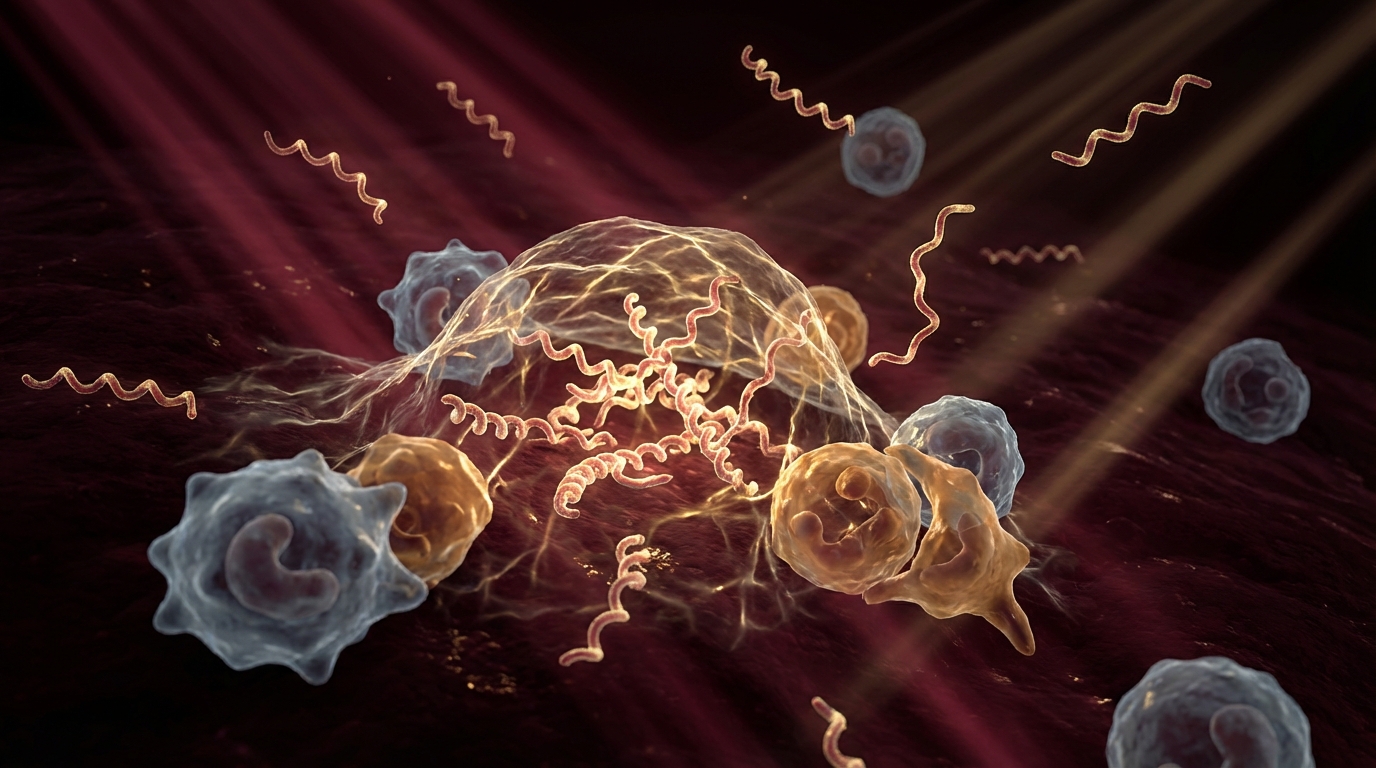
But the conversation about antibiotic resistance in the context of chronic infection is more nuanced than the standard public health framing. In chronic infections, treatment failure is often not about genetic resistance in the traditional sense. It is about persistence — the ability of organisms to survive antibiotic exposure through biofilm formation, intracellular hiding, metabolic dormancy, and morphological variation.
Understanding this distinction is important because it changes the therapeutic approach.
Resistance vs. Tolerance vs. Persistence
Genetic resistance means the organism has acquired mutations or genes that render specific antibiotics ineffective. The bacteria can grow in the presence of the antibiotic at any concentration. This is the type of resistance that public health campaigns focus on, and it is a genuine crisis.

Tolerance means the organism can survive antibiotic exposure for longer periods, even though it is not genetically resistant. Tolerant organisms are not killed as quickly as susceptible ones, but given sufficient duration and concentration, the antibiotic can still work.
Persistence refers to subpopulations of cells — often within biofilms — that enter a metabolically dormant state in which they are effectively invisible to antibiotics that require active metabolism. These persister cells can repopulate the infection after antibiotic therapy ends, causing clinical relapse [1].
In chronic tick-borne disease, all three phenomena can coexist. This is why treatment often requires:
- Combination therapy targeting different mechanisms
- Extended treatment courses
- Biofilm disruption strategies
- Agents that address different metabolic states (actively growing and dormant)
Alternatives and Adjuncts to Conventional Antibiotics
In my practice, I do not view antibiotic alternatives as replacements for pharmaceuticals. I view them as components of a comprehensive strategy that may include conventional antibiotics, non-antibiotic antimicrobials, immune modulation, and physical therapies.
Herbal Antimicrobials
Several botanical medicines have demonstrated antimicrobial activity in laboratory studies, and some have preliminary clinical data:
Cryptolepis sanguinolenta: Demonstrated activity against Borrelia burgdorferi, including persister forms, in vitro. A study by Feng et al. showed that cryptolepis extract was more effective against Borrelia persisters than doxycycline or cefuroxime [2].
Japanese knotweed (Polygonum cuspidatum / Reynoutria japonica): Contains resveratrol and other polyphenols with anti-Borrelia activity in vitro.
Cat’s claw (Uncaria tomentosa): Demonstrated activity against Borrelia, including biofilm forms, and has immunomodulatory properties.
Artemisinin (sweet wormwood): Traditional antimalarial with activity against Babesia and other protozoa. Also has anti-Borrelia properties in vitro.
Oregano oil (carvacrol): Broad-spectrum antimicrobial with antibiofilm activity.
I want to be transparent about the evidence level. Most of these findings come from in vitro studies. Whether the concentrations that show activity in a petri dish are achievable at relevant tissue sites through oral supplementation is often unknown. I use herbal antimicrobials as adjuncts to conventional therapy, particularly in patients with prolonged treatment courses where antibiotic cycling is necessary, or in patients who cannot tolerate additional pharmaceutical antibiotics.
Ozone Therapy
Medical ozone (ozone-oxygen mixtures) has demonstrated antimicrobial activity through oxidative mechanisms. Ozone therapy is used at our facility as an adjunct in chronic infection treatment programs. Common modalities include:
- Major autohemotherapy (mixing ozone with the patient’s blood and reinfusing)
- Rectal insufflation
- Topical application for wound infections
The mechanistic rationale is sound: ozone generates reactive oxygen species that damage microbial membranes and biofilm matrices. The clinical evidence is more limited than I would like — controlled trials specifically for tick-borne disease are scarce — but clinical observation over decades at our facility suggests benefit as part of a multimodal approach.
Hyperthermia
Therapeutic hyperthermia — controlled elevation of body temperature to 38.5-40.5 degrees C — leverages the heat sensitivity of many pathogens. Borrelia, in particular, has reduced viability at temperatures above 39 degrees C. Hyperthermia also stimulates immune function and may enhance antibiotic penetration into tissues.
This is one of the modalities most specific to our facility’s approach and one that patients frequently identify as a meaningful component of their treatment.
Phage Therapy
Bacteriophages — viruses that specifically infect and kill bacteria — represent one of the most promising alternatives to antibiotics. Phage therapy has a long history of clinical use in Eastern Europe and Georgia. Western interest is growing as antibiotic resistance escalates.
For chronic infections, phage therapy is still largely in the research and compassionate-use phase in Western medicine. Challenges include identifying the correct phage for each bacterial strain, ensuring phage viability and safety, and navigating regulatory frameworks that were not designed for biological therapies of this type.
I follow this field closely. I expect phage therapy to become a significant clinical tool within the next decade.
Antimicrobial Peptides
Naturally occurring antimicrobial peptides (defensins, cathelicidins) represent another frontier. Some are being developed as pharmaceutical agents. Others can be supported through nutritional and immune-supportive interventions.
Managing Resistance in Practice
In my chronic infection practice, I approach antibiotic resistance pragmatically:
- Use combination therapy. Multiple agents targeting different mechanisms reduce the likelihood of resistance development and address different subpopulations (active, persister, biofilm-embedded).
- Cycle antibiotics. Rotating between antibiotic classes during prolonged treatment courses reduces resistance pressure and may improve efficacy by targeting organisms as they cycle through different metabolic states.
- Incorporate non-antibiotic antimicrobials. Herbal agents, ozone, and hyperthermia provide antimicrobial pressure through mechanisms against which bacterial resistance is less likely to develop.
- Disrupt biofilms. As discussed in my biofilm article, biofilm disruption improves antibiotic access to protected organisms.
- Support immune function. Ultimately, the patient’s immune system is the most important antimicrobial. No external therapy can substitute for a functioning immune response.
- Use antibiotics judiciously. Longer is not always better. Intensive, targeted treatment courses with clear endpoints are preferable to indefinite, low-dose antibiotic exposure.
The Bottom Line
Antibiotic resistance is a real and growing challenge, but the narrative that antibiotics are becoming useless oversimplifies the situation. In chronic infection management, treatment failure is more often about persistence and biofilm protection than about genetic resistance. A comprehensive approach that combines conventional antibiotics with biofilm disruption, non-antibiotic antimicrobials, immune support, and physical therapies expands the therapeutic options considerably.

References
- Lewis K. Persister cells. Annual Review of Microbiology. 2010;64:357-372.
- Feng J, et al. Identification of Additional Anti-Persister Activity against Borrelia burgdorferi from an FDA Drug Library. Antibiotics. 2015;4(3):397-410.
This content is educational and does not constitute medical advice. Antibiotic therapy for chronic infections should be managed by a physician experienced in complex infectious disease.