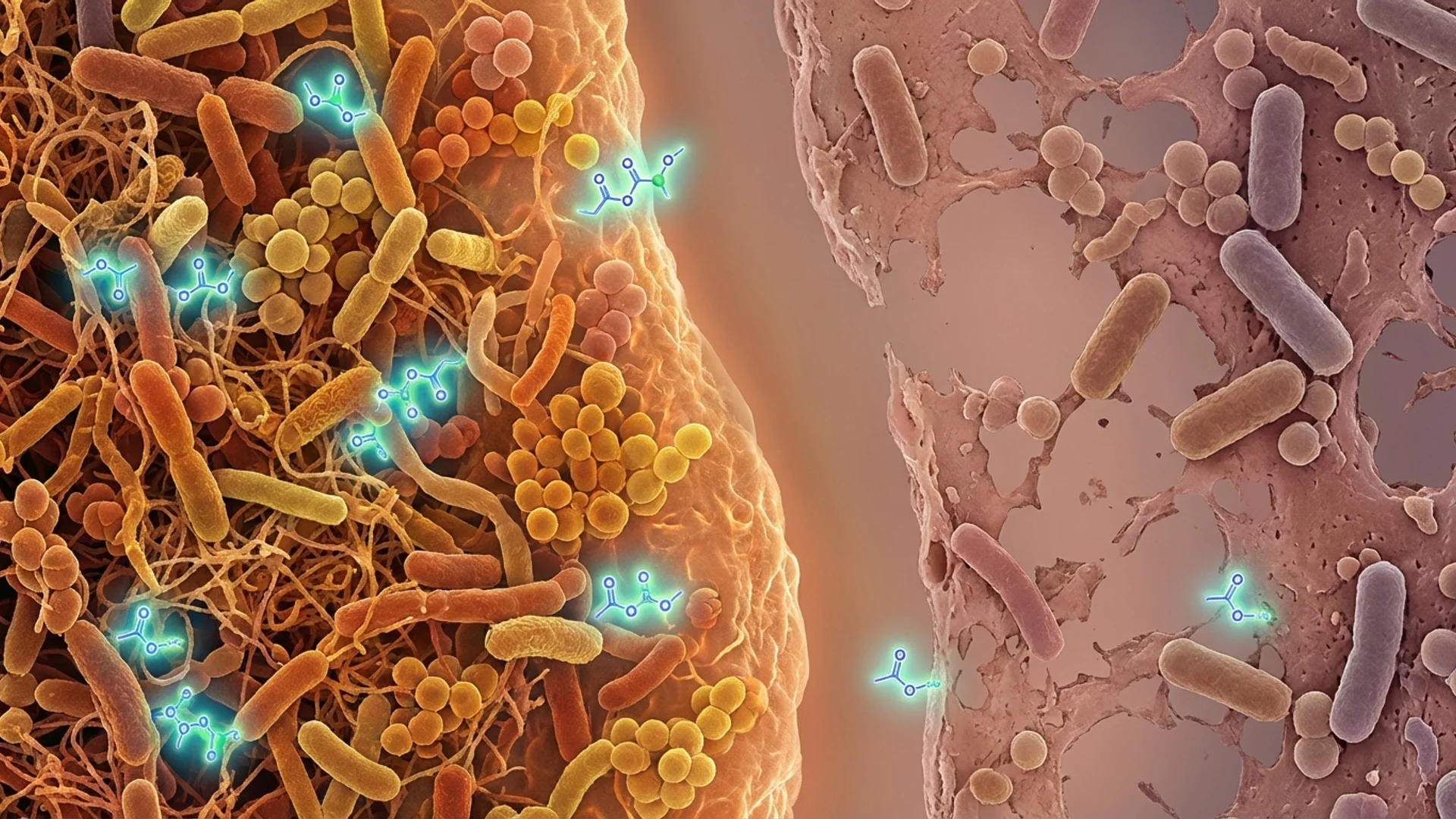
The human gut harbors approximately 38 trillion microorganisms — roughly as many cells as the human body itself. These are not passengers. They are participants in a biological relationship that has co-evolved over millions of years, and their influence on immune function is profound and increasingly well-documented.
Let me be direct: the microbiome field has generated enormous hype alongside genuine science. Not every claim you read about the microbiome is supported by rigorous evidence. What I will present here is what we know with reasonable confidence, what we suspect, and where the gaps remain.
Why Diversity Matters
The single most consistent finding in microbiome research is that microbial diversity is associated with health, while reduced diversity is associated with disease. This correlation has been documented across multiple conditions: inflammatory bowel disease, obesity, type 2 diabetes, autoimmune disease, allergic disease, and depression.
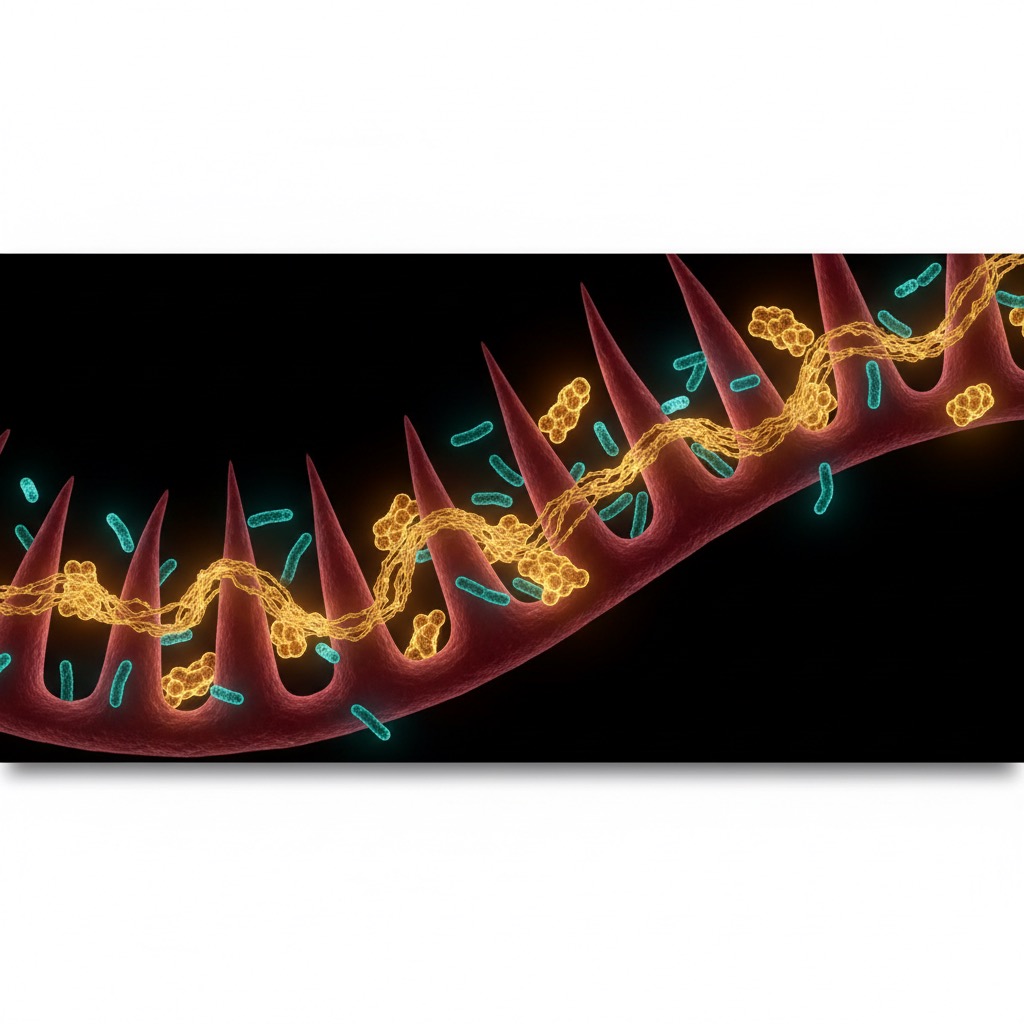
The mechanism is not merely statistical. A diverse microbiome provides:
- Functional redundancy — multiple species can perform the same metabolic functions, providing resilience
- Competitive exclusion — diverse communities are more resistant to pathogenic colonization
- Broader metabolite production — different species produce different short-chain fatty acids, vitamins, and immune-active compounds
- More complete immune education — the immune system requires exposure to diverse microbial signals for proper calibration
The factors that most reliably reduce microbial diversity include antibiotic use (particularly broad-spectrum), a low-fiber, highly processed diet, chronic stress, and limited environmental microbial exposure. These are, not coincidentally, hallmarks of modern Western life.
Key Bacterial Groups and Their Functions
Not all bacteria are equal in their immune effects. Several groups deserve specific attention:
Faecalibacterium prausnitzii is the most abundant bacterium in the healthy human gut and the primary producer of butyrate. It has anti-inflammatory properties mediated through butyrate production and direct interaction with immune cells. Reduced F. prausnitzii abundance is consistently associated with Crohn’s disease and ulcerative colitis. Evidence level: controlled human studies (multiple).
Akkermansia muciniphila resides in the mucus layer and plays a critical role in maintaining mucus barrier integrity. Lower levels are associated with obesity, type 2 diabetes, and impaired responses to cancer immunotherapy. Supplementation with pasteurized A. muciniphila has shown metabolic benefits in an RCT (Depommier et al., Nature Medicine 2019).
Bifidobacterium species are dominant in the infant gut and remain important throughout life. They produce acetate and lactate, lower gut pH (inhibiting pathogenic growth), and support sIgA production. Their abundance declines with age, potentially contributing to immunosenescence.
Lactobacillus species produce lactic acid and bacteriocins (antimicrobial peptides), support gut barrier integrity, and modulate dendritic cell function. Specific strains have strong clinical trial evidence for specific indications (L. rhamnosus GG for diarrhea prevention, L. plantarum 299v for IBS).
Microbiome Testing: What Is Useful
The microbiome testing landscape is cluttered with products of varying clinical utility. Here is my honest assessment.
What Has Clinical Value
PCR-based comprehensive stool analysis (GI-MAP or equivalent) provides clinically actionable information: identification of specific pathogens (Clostridium difficile, Helicobacter pylori, parasites), markers of inflammation (calprotectin, lactoferrin), digestive function markers (elastase, steatocrit), and semi-quantitative assessment of key bacterial groups.
Calprotectin is a fecal marker of intestinal inflammation with strong diagnostic accuracy for differentiating inflammatory bowel disease from irritable bowel syndrome. It is one of the most useful single tests in gastrointestinal assessment.
What Has Limitations
16S rRNA sequencing provides a detailed picture of bacterial composition but has limited clinical applicability. Knowing that you have a specific percentage of Bacteroidetes versus Firmicutes does not, by itself, tell me what to treat. The research value is substantial; the clinical translation is still developing.
Shotgun metagenomics provides even more detailed information, including functional capacity (what the bacteria can do, not just what species are present). This is scientifically powerful but clinically immature — we do not yet have robust frameworks for translating metagenomic findings into treatment decisions for individual patients.
What I tell my patients: a good PCR-based stool analysis gives me the information I need to make treatment decisions. More advanced sequencing is interesting and may become clinically valuable, but it is not where I would start.
Microbiome Restoration
What the Evidence Supports
Dietary diversity remains the single most effective intervention for increasing microbial diversity. The landmark Stanford study (Wastyk et al., Cell 2021) demonstrated that a high-fermented-food diet increased microbial diversity and reduced inflammatory markers more effectively than a high-fiber diet alone — an important finding that suggests fermented foods offer benefits beyond simple prebiotic fiber.
Probiotic supplementation is effective for specific conditions with specific strains, but the evidence does not support the general claim that “taking probiotics” improves immune health. The strain-specificity matters enormously. What works for antibiotic-associated diarrhea (Saccharomyces boulardii — RCT evidence) is not the same as what works for IBS (Bifidobacterium infantis 35624 — RCT evidence).
Prebiotic fiber feeds beneficial bacteria and increases short-chain fatty acid production. PHGG (partially hydrolyzed guar gum), GOS (galactooligosaccharides), and resistant starch have the strongest evidence. Evidence level: multiple RCTs.
Fecal microbiota transplantation (FMT) is extraordinarily effective for recurrent Clostridioides difficile infection (approximately 90% cure rate — RCT evidence). Its application to other conditions (IBD, metabolic syndrome, neurological disease) is under active investigation, with preliminary results that range from promising to disappointing depending on the condition.
What Deserves Continued Research
Postbiotics — the metabolic byproducts of bacterial metabolism (short-chain fatty acids, bacterial cell wall components, enzymes) — may offer a more targeted approach than live bacteria. Supplemental butyrate, for example, provides the immune-modulating benefits of butyrate without depending on the patient’s microbiome to produce it.
Precision probiotics — selecting probiotic strains based on individual microbiome analysis rather than generic formulations — is a logical next step, but the science is not yet mature enough to support reliable clinical recommendations.
Spore-based probiotics (Bacillus coagulans, Bacillus subtilis) survive gastric acid more reliably than conventional probiotics and have accumulating evidence for immune modulation. Preliminary data is positive, but the evidence base is smaller than for Lactobacillus and Bifidobacterium species.
My Clinical Approach
When I see a patient with suspected microbiome dysfunction, the approach follows a logical sequence:
- Test first. A comprehensive stool analysis identifies what is actually present — infections, inflammatory markers, digestive insufficiencies, and the state of major bacterial groups.
- Remove what should not be there. Active infections and overgrowth are addressed before attempting to rebuild.
- Repair the terrain. Gut lining repair (glutamine, zinc carnosine, butyrate) creates an environment where beneficial bacteria can establish.
- Reinoculate with evidence. Specific probiotic strains matched to clinical findings, plus fermented foods.
- Feed the new ecosystem. Prebiotic fiber and dietary diversity sustain the restoration.
- Retest. Follow-up stool analysis at 8-12 weeks confirms whether the intervention has produced the expected changes.
This is not a quick fix. Meaningful microbiome restoration typically requires three to six months, and dietary and lifestyle changes must be sustained to maintain the results.
Disclaimer: This article is provided for educational purposes and reflects one physician’s clinical perspective. It is not a substitute for individualized medical care. Consult a qualified physician before beginning any microbiome restoration protocol.