At a Glance
| Property | Value |
|---|---|
| Evidence Level | Moderate (pathophysiology well-characterized; treatment evidence growing) |
| Primary Mechanisms | Mitochondrial dysfunction, immune dysregulation, neuroinflammation, HPA axis disruption |
| Common Triggers | Viral infection (EBV, CMV, HHV-6, SARS-CoV-2), bacterial infection, physical trauma, severe stress |
| Key Diagnostic Criteria | Fukuda (1994), Canadian Consensus (2003), IOM/SEID (2015) |
| Key Intervention | TPS (Transcranial Pulse Stimulation) for neurological and cognitive symptoms |
| Prevalence | 0.4-1% of the global population; likely significantly underdiagnosed |
The Disease That Medicine Refused to Take Seriously
If you have chronic fatigue syndrome — or if you suspect you do and have been dismissed by doctor after doctor — I want to start with three words: I believe you.
ME/CFS (Myalgic Encephalomyelitis/Chronic Fatigue Syndrome) is not depression. It is not deconditioning. It is not “all in your head.” It is a multi-system disease with measurable biological abnormalities that has been systematically neglected by the medical establishment for decades. The name itself — “chronic fatigue syndrome” — is an insult to the severity of the condition, like calling a heart attack “chronic chest discomfort syndrome.”
Here is what the evidence shows.
ME/CFS affects an estimated 17-24 million people worldwide [1]. The average time to diagnosis exceeds 4 years. Up to 90% of patients remain undiagnosed. The disease receives less than $15 per patient in annual NIH research funding — a fraction of what comparable conditions receive. These are not my opinions. These are documented facts that should make every physician angry.
In my clinical experience, ME/CFS patients are among the most medically gaslit populations I encounter. They have been told to exercise more (which makes them worse), to see a psychiatrist (who finds no primary psychiatric disorder), or simply to “push through it” (which triggers post-exertional malaise that can set them back weeks). This is not acceptable medicine.
Let me explain what is actually happening in your body.
The Four Pillars of ME/CFS Pathophysiology
ME/CFS is not a single-mechanism disease. It involves at least four interconnected systems, all of which must be understood and addressed for treatment to be effective.
1. Mitochondrial Dysfunction
Mitochondria are the energy-producing organelles in every cell of your body. They convert glucose and fatty acids into ATP — the molecular currency of cellular energy. In ME/CFS, this process is impaired.
Research has demonstrated multiple mitochondrial abnormalities in ME/CFS patients:
- Reduced ATP production: Direct measurements of ATP levels in ME/CFS patients show significant reductions compared to healthy controls [2].
- Impaired oxidative phosphorylation: The electron transport chain — the mitochondria’s primary ATP-generating pathway — functions suboptimally.
- Metabolic switching: ME/CFS patients show a shift away from efficient aerobic metabolism toward less efficient glycolytic and amino acid-based energy production [3]. This is measurable on metabolomic testing and explains the disproportionate fatigue: cells are running on backup generators instead of the main power plant.
- Increased oxidative stress: Dysfunctional mitochondria produce excess reactive oxygen species (ROS), which damage cellular components and further impair mitochondrial function — a vicious cycle.
What I tell my patients: your fatigue is not because you are lazy or deconditioned. Your cells literally cannot produce enough energy to meet normal demands. This is measurable, it is real, and it has a biological basis.
2. Immune Dysregulation
The immune system in ME/CFS is not simply overactive or underactive — it is dysregulated. Specific abnormalities include:
- Chronic immune activation: Elevated pro-inflammatory cytokines (IL-1, IL-6, TNF-alpha) and markers of immune activation are consistently found in ME/CFS patients, particularly in the first 3 years of illness [4].
- Natural killer (NK) cell dysfunction: NK cells in ME/CFS patients show reduced cytotoxic function despite often normal cell counts. This may explain the vulnerability to viral reactivation.
- T-cell exhaustion: CD8+ T-cells show markers of chronic activation and exhaustion, consistent with ongoing antigen stimulation — possibly from persistent viral reservoirs.
- Autoimmune features: A subset of ME/CFS patients have autoantibodies against neuronal receptors (muscarinic and adrenergic receptors), which may contribute to autonomic dysfunction [5].
The overlap with post-COVID syndrome here is striking and not coincidental. Many of the same immune abnormalities found in ME/CFS are now being documented in Long COVID patients. In many cases, Long COVID IS ME/CFS triggered by SARS-CoV-2.
3. HPA Axis Disruption
The hypothalamic-pituitary-adrenal (HPA) axis is the body’s central stress response system. In ME/CFS, it is characteristically blunted:
- Mild hypocortisolism: Cortisol levels are often at the low end of normal or frankly low, not due to adrenal failure but due to hypothalamic underactivity [6].
- Flattened diurnal cortisol curve: The normal morning cortisol peak is reduced or absent.
- Impaired stress response: The adrenal response to ACTH stimulation and stress is attenuated.
This is not “adrenal fatigue” as the wellness industry uses the term. It is a measurable neuroendocrine abnormality with specific characteristics that differ from both Addison’s disease and normal variation.
4. Neuroinflammation and Central Sensitization
PET imaging studies have demonstrated neuroinflammation in ME/CFS patients — activated microglia and astrocytes in specific brain regions [7]. This neuroinflammation:
- Disrupts neurotransmitter balance
- Impairs cognitive processing (the “brain fog” patients describe)
- Increases pain sensitization (central sensitization)
- Disrupts sleep architecture
- May contribute to autonomic dysfunction
This is where TPS (Transcranial Pulse Stimulation) becomes particularly relevant — but I will discuss that in the treatment section.

Viral Triggers: How It Starts
In approximately 70% of ME/CFS cases, the disease onset follows an acute infection [8]. The most commonly implicated pathogens include:
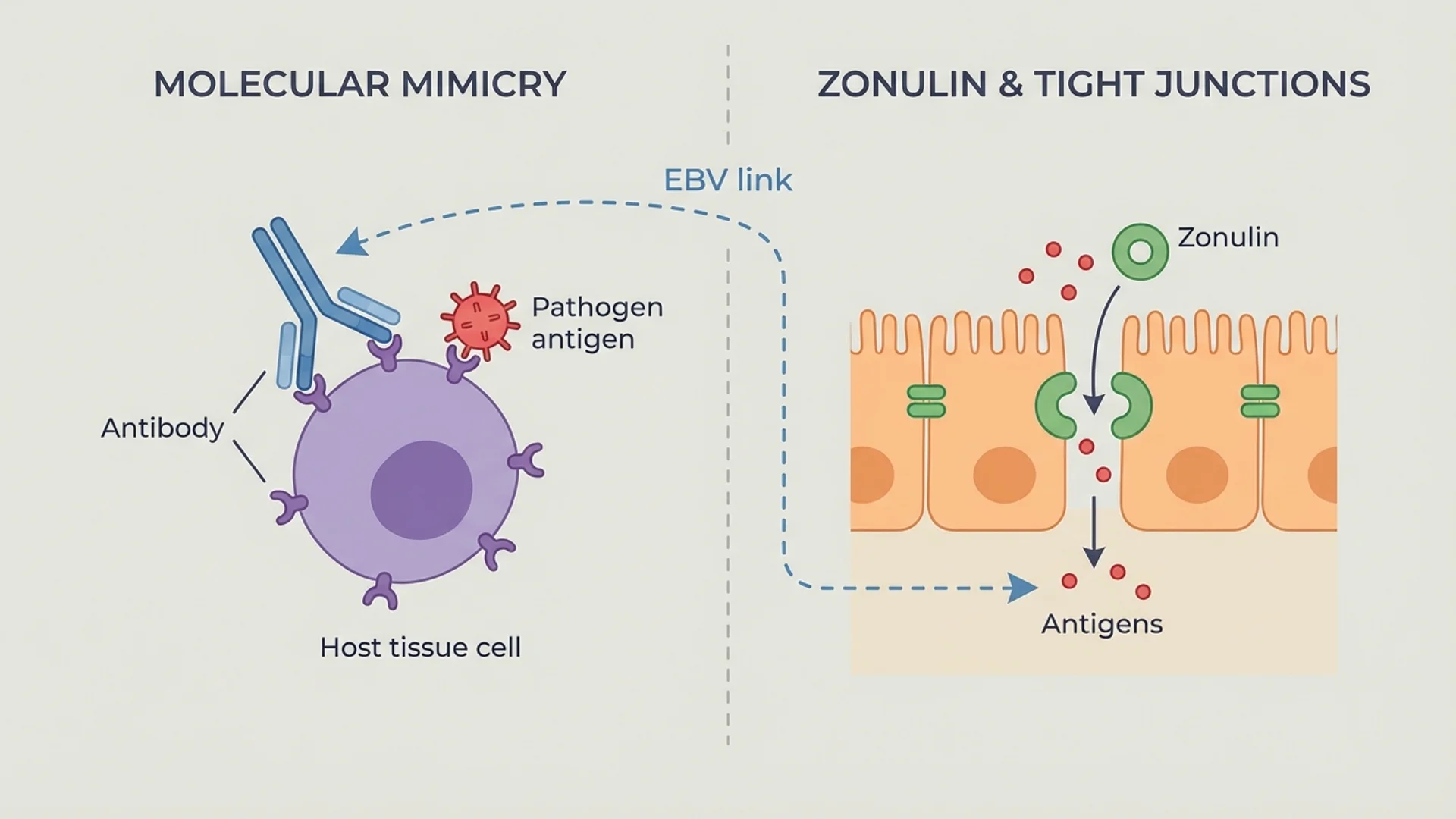
- Epstein-Barr virus (EBV): The most studied trigger. Prospective studies following infectious mononucleosis show that approximately 10% of patients develop ME/CFS criteria at 6 months [9].
- Cytomegalovirus (CMV)
- Human herpesvirus 6 (HHV-6)
- Enteroviruses
- SARS-CoV-2: The pandemic has effectively created a massive natural experiment. The proportion of COVID-19 patients who develop Long COVID meeting ME/CFS criteria provides powerful evidence that post-viral ME/CFS is a real and reproducible phenomenon.
- Coxiella burnetii (Q fever)
The question is not whether these viruses trigger ME/CFS — the evidence clearly supports that they do. The question is why some people develop ME/CFS after infection and others do not. The answer likely involves genetic susceptibility (HLA types, immune gene variants), the severity and duration of the initial infection, and possibly the reactivation of latent viruses during acute illness.
Diagnostic Criteria: Three Frameworks
One of the frustrations of ME/CFS is the existence of multiple diagnostic criteria, none universally adopted. Here are the three you should know:
Fukuda Criteria (1994)
The oldest and most widely used in research:
- Clinically evaluated, unexplained fatigue lasting 6+ months
- Not due to ongoing exertion, not substantially relieved by rest
- Results in substantial reduction in activity levels
- Plus 4 or more of: impaired memory/concentration, sore throat, tender lymph nodes, muscle pain, joint pain, new headaches, unrefreshing sleep, post-exertional malaise
Limitation: Casts too wide a net. Includes patients with fatigue from other causes. Does not require post-exertional malaise (PEM) as mandatory.
Canadian Consensus Criteria (2003)
More specific and clinically useful:
- Fatigue with substantial reduction in activity
- Post-exertional malaise (mandatory) — disproportionate symptom worsening after physical or cognitive exertion
- Sleep dysfunction
- Pain
- Two or more neurological/cognitive manifestations
- At least one autonomic, neuroendocrine, or immune manifestation
Strength: PEM is required. This excludes many patients with fatigue from other causes who do not have the hallmark post-exertional crash.
IOM/SEID Criteria (2015)
The most recent, proposed by the US Institute of Medicine:
- Substantial reduction in ability to engage in pre-illness activities, lasting 6+ months, with fatigue that is not the result of excessive exertion and is not substantially relieved by rest
- Post-exertional malaise (mandatory)
- Unrefreshing sleep (mandatory)
- Plus at least one of: cognitive impairment OR orthostatic intolerance
Strength: Simple, clinician-friendly, makes PEM central. Also proposed renaming the condition “Systemic Exertion Intolerance Disease” (SEID), though adoption has been slow.
My Approach to Diagnosis
In practice, I use the Canadian Consensus Criteria as my primary diagnostic framework because it is the most specific and requires PEM — which I consider the pathognomonic feature of ME/CFS. A patient who does not experience disproportionate symptom worsening after exertion likely has a different condition.
I also run extensive laboratory testing to exclude mimics and identify treatable contributing factors: thyroid function, cortisol profiles, viral serology (EBV, CMV, HHV-6), NK cell function, autoantibody panels, mitochondrial metabolomics, and in selected cases, cerebrospinal fluid analysis.
The Stepwise Treatment Approach
There is no single drug or intervention that cures ME/CFS. What I tell my patients is this: meaningful improvement is achievable for most patients, but it requires a systematic, stepwise approach that addresses the underlying mechanisms in the right order.
Step 1: Stabilize Energy Systems
Before anything else, stop the energy drain.
Pacing: The most important intervention is also the least glamorous. Patients must learn to stay within their “energy envelope” — the amount of activity they can sustain without triggering post-exertional malaise. This is not laziness; it is strategic energy management. Push-crash cycles cause cumulative damage.
Mitochondrial support:
- Coenzyme Q10 (200-400mg daily) — essential cofactor for electron transport chain Complex III
- D-ribose (5g, 2-3 times daily) — substrate for ATP synthesis
- NADH (10-20mg daily) — electron donor for Complex I
- Magnesium (glycinate or threonate, 400-600mg daily) — cofactor for over 300 enzymatic reactions including ATP synthesis
- Alpha-lipoic acid (600mg daily) — mitochondrial antioxidant
This is not random supplementation. Each of these targets a specific, documented mitochondrial abnormality in ME/CFS. The evidence is moderate — smaller clinical trials show benefit, but large RCTs are lacking [10].
Sleep optimization: Unrefreshing sleep is universal in ME/CFS and perpetuates the disease cycle. Addressing sleep architecture disturbances is foundational.
Step 2: Address Immune Dysfunction
Once energy systems are stabilized, address the immune drivers.
Identify and treat persistent infections: Test for and treat reactivated EBV, CMV, HHV-6 if titers suggest active replication. In some cases, antiviral therapy (valacyclovir, valganciclovir) produces dramatic improvement, suggesting ongoing viral replication as a disease driver.
Immune modulation:
- Low-dose naltrexone (1.5-4.5mg at bedtime) — modulates toll-like receptor 4, reduces neuroinflammation, upregulates endorphin production. Emerging evidence in ME/CFS with good tolerability [11].
- Thymosin alpha-1 — peptide immunomodulator that restores NK cell function and rebalances T-cell populations. This is investigational for ME/CFS but based on strong mechanistic rationale and positive clinical observations.
Apheresis: For patients with significant inflammatory burden, particularly those with post-viral ME/CFS, therapeutic apheresis can rapidly reduce circulating inflammatory mediators and immune complexes.
Step 3: Restore Neurological Function with TPS
This is where I want to spend particular attention, because TPS (Transcranial Pulse Stimulation) has become one of the most important tools in my treatment of ME/CFS.
TPS uses focused, low-energy shock waves to stimulate specific brain regions non-invasively. Unlike TMS (transcranial magnetic stimulation), which affects only superficial cortical areas, TPS penetrates to deep brain structures — including the hypothalamus, thalamus, and brainstem autonomic centers that are directly implicated in ME/CFS pathophysiology [12].
What TPS targets in ME/CFS:
- Neuroinflammation: TPS has demonstrated the ability to modulate microglial activation and reduce neuroinflammatory markers.
- Hypothalamic function: Direct stimulation of the hypothalamus may address the HPA axis dysfunction central to ME/CFS.
- Autonomic regulation: Stimulation of brainstem autonomic centers can improve the autonomic dysfunction (POTS, blood pressure instability) that plagues many ME/CFS patients.
- Cognitive processing: Targeted stimulation of prefrontal and temporal cortical regions addresses brain fog.
The protocol: Typically 6-12 sessions over 2-6 weeks, with each session lasting 30-45 minutes. The treatment is painless and requires no anesthesia.
What I observe in practice: TPS is not a cure for ME/CFS. But in my clinical experience, it produces more consistent improvement in cognitive function, energy levels, and autonomic regulation than any other single intervention I have used. Patients frequently report that “the fog lifts” — that they can think clearly again for the first time in months or years. This improvement, combined with the other steps in the protocol, creates a positive cascade.
I classify this as clinical observation. TPS is approved in Europe for Alzheimer’s disease based on clinical data, and its application to ME/CFS is extrapolated from that evidence plus mechanistic reasoning and clinical outcomes. We need dedicated ME/CFS trials, and I hope they are coming.

Step 4: Rebuild Capacity
Only after the previous steps have been addressed should patients begin to cautiously expand their activity levels.
Graded activity expansion (not graded exercise therapy): This is an important distinction. The controversial “graded exercise therapy” (GET) recommended by some guidelines has been removed from NICE guidelines in the UK because it caused harm to many ME/CFS patients [13]. What I recommend is different: very gradual, pacing-based activity expansion guided by the patient’s response, never pushing into PEM territory. Increase only when the current level is tolerated consistently.
Continued mitochondrial and immune support: The supplements and interventions from earlier steps continue.
Addressing deconditioning carefully: Some patients have become significantly deconditioned due to prolonged illness. Reconditioning must happen at the patient’s pace, not the physician’s expectations.
Psychosocial support: ME/CFS causes enormous psychological burden — not because it is a psychological disease, but because living with a severe chronic illness that is poorly understood and often dismissed creates depression, anxiety, and grief. Addressing these is part of comprehensive care, not a suggestion that the disease is “mental.”
What the Research Actually Says About Prognosis
Let me be honest about outcomes.
Full recovery (return to pre-illness function) occurs in approximately 5-10% of ME/CFS patients, though higher rates are reported in adolescents and those with shorter illness duration [14].
Significant improvement (meaningful reduction in symptoms, expanded functional capacity) occurs in a larger proportion — estimated at 30-50% with appropriate treatment.
Stable chronic illness with management of symptoms is the reality for many patients.
Progressive deterioration occurs in a minority, particularly those with severe presentations.
What changes these numbers is early, appropriate intervention. The longer ME/CFS goes untreated or mistreated (with inappropriate exercise programs, dismissal, or neglect), the more entrenched the pathophysiology becomes. This is why accurate diagnosis and timely treatment matter.
In our clinical experience, patients who receive comprehensive treatment — addressing mitochondrial function, immune dysregulation, and neurological symptoms with TPS — generally fall into the “significant improvement” category. I cannot promise recovery, but I can promise an honest, evidence-based effort that takes the disease seriously.
The Bottom Line
ME/CFS is a multi-system biological disease with measurable abnormalities in mitochondrial function, immune regulation, the HPA axis, and the central nervous system. It is underdiagnosed, underfunded, and undertreated. Effective management requires a stepwise approach: stabilize energy systems, address immune dysfunction, restore neurological function (TPS is a key tool here), and cautiously rebuild capacity. This is not a disease that responds to a single pill or a motivational speech. It responds to physicians who understand the biology, take the patient seriously, and apply the right interventions in the right order.
References
- Lim EJ, Ahn YC, Jang ES, et al. Systematic review and meta-analysis of the prevalence of chronic fatigue syndrome/myalgic encephalomyelitis (CFS/ME). J Transl Med. 2020;18(1):100.
- Myhill S, Booth NE, McLaren-Howard J. Chronic fatigue syndrome and mitochondrial dysfunction. Int J Clin Exp Med. 2009;2(1):1-16.
- Naviaux RK, Naviaux JC, Li K, et al. Metabolic features of chronic fatigue syndrome. Proc Natl Acad Sci USA. 2016;113(37):E5472-E5480.
- Montoya JG, Holmes TH, Anderson JN, et al. Cytokine signature associated with disease severity in chronic fatigue syndrome patients. Proc Natl Acad Sci USA. 2017;114(34):E7150-E7158.
- Loebel M, Grabowski P, Heidecke H, et al. Antibodies to beta-adrenergic and muscarinic cholinergic receptors in patients with Chronic Fatigue Syndrome. Brain Behav Immun. 2016;52:32-39.
- Papadopoulos AS, Cleare AJ. Hypothalamic-pituitary-adrenal axis dysfunction in chronic fatigue syndrome. Nat Rev Endocrinol. 2012;8(1):22-32.
- Nakatomi Y, Mizuno K, Ishii A, et al. Neuroinflammation in patients with chronic fatigue syndrome/myalgic encephalomyelitis: an 11C-(R)-PK11195 PET study. J Nucl Med. 2014;55(6):945-950.
- Chu L, Valencia IJ, Garvert DW, et al. Onset patterns and course of myalgic encephalomyelitis/chronic fatigue syndrome. Front Pediatr. 2019;7:12.
- Hickie I, Davenport T, Wakefield D, et al. Post-infective and chronic fatigue syndromes precipitated by viral and non-viral pathogens: prospective cohort study. BMJ. 2006;333(7568):575.
- Castro-Marrero J, Saez-Francas N, Segundo MJ, et al. Effect of coenzyme Q10 plus nicotinamide adenine dinucleotide supplementation on maximum heart rate after exercise testing in chronic fatigue syndrome. Clin Nutr. 2016;35(4):826-834.
- Bolton MJ, Chapman BP, Van Marwijk H. Low-dose naltrexone as a treatment for chronic fatigue syndrome. BMJ Case Rep. 2020;13(1):e232502.
- Beisteiner R, Matt E, Fan C, et al. Transcranial pulse stimulation with ultrasound in Alzheimer’s disease — a new navigated focal brain therapy. Adv Sci. 2020;7(3):1902583.
- National Institute for Health and Care Excellence. Myalgic encephalomyelitis (or encephalopathy)/chronic fatigue syndrome: diagnosis and management. NICE guideline [NG206]. 2021.
- Cairns R, Hotopf M. A systematic review describing the prognosis of chronic fatigue syndrome. Occup Med. 2005;55(1):20-31.